

Figure 1 Clinical Pharmacy Training Log
Stephanie WK Teoh1, Tamara Lebedevs2, and Nabeelah Mukadam3
1BPharm(Hons), MClinPharm, Pharmacy Department, King Edward Memorial Hospital, Perth, Australia
2BPharm, PostGradDipPharm, Pharmacy Department, King Edward Memorial Hospital, Perth, Australia
3BPharm(Hons), MPhil (Pharmacy), Pharmacy Department, King Edward Memorial Hospital, Perth, Australia
ABSTRACT
Background: A training program aimed at increasing the knowledge and skillsets of obstetric clinical pharmacists to ensure consistency and quality of service delivery is described here.
Methods: The pharmacy department developed a training program to increase the knowledge and skillsets of pharmacists, particularly those who have not worked as an intern or completed residency training in a women hospital. The training program was designed based on the services offered, departmental size, resources available, and time allotted for training.
Results: Clinical practice guidelines, policy statements, and other sources were used to develop the training materials, consisting of an e-Learning package, followed by face-to-face teaching, demonstration and working under supervision. The self-directed learning module was endorsed by the North Metropolitan Health Services Department of Learning and Development and the trainees who completed the program earned a certificate from the department. From its implementation in August 2023, the department has trained five pharmacists and four intern pharmacists using the new training program.
Discussion: The implementation of a training program to educate pharmacists in obstetric clinical services helped to ensure consistency and competency in the service provision of clinical pharmacists, while ensuring the sustainability of training in the department. Our experience in developing and implementing the education model fostered the transition to structured training in obstetric clinical pharmacy.
Key Words: Pharmacy, Education, Obstetric, Women Health, Clinical Pharmacy
Email: Stephanie WK Teoh (Stephanie.Teoh@health.wa.gov.au)
Date submitted: 12-February-2025
This is an open access journal, and articles are distributed under the terms of the Creative Commons Attribution-Non Commercial-Share Alike 4.0 License, which allows others to remix, tweak, and build upon the work non-commercially, as long as appropriate credit is given and the new creations are licensed under the identical terms.
Citation: Teoh S, Lebedevs T, and Mukadam N. A comprehensive education framework for clinical pharmacy services in an Australian women’s hospital. Educ Health 2025;38:258-268.
Online access: www.educationforhealthjournal.org
DOI: 10.62694/efh.2025.279
Published by The Network: Towards Unity for Health
Undergraduate pharmacy studies cover competencies required for community pharmacists, hospital pharmacists, pharmacists in pharmaceutical manufacturing and in research, and skillsets involving medicine logistics, extemporaneous preparation of medicines, medication counselling, medication reconciliation, over-the-counter medicines and medication management for various medical conditions.1–4 The universities allocate varying amounts of teaching and clinical hours preparing undergraduate students to work in a hospital. A recent study demonstrates that clinical pharmacy services are still underdeveloped and underutilized in countries including most of Central and Eastern Europe.5 Meanwhile, the lack of qualified and well-trained pharmacists has been identified as one of the key barriers to advancement of clinical pharmacy in a study evaluating the clinical pharmacy practice and education in Taiwan, Vietnam and Indonesia.6 A global survey involving 85 countries identified the opportunities for growth and development in hospital pharmacy to advance the profession and ensure that patients worldwide receive the care that they deserve.7
Pregnancy complications, comorbidities, and maternal morbidity have been on the rise due to increased age, higher rates of obesity and preexisting chronic conditions, and higher rates of caesarean delivery.4,8–9 Obstetric pharmacists are increasingly important in the medication management of obstetric patients, including profile review to identify and document past medical history and play an active role in the medication management of diabetes, infection, prevention of venous thromboembolism and providing medicine safety advice for pregnancy and lactation.4,8–11 Obstetric pharmacy services have proved to contribute to fewer hospital days for mothers and their newborns, fewer admissions to the neonatal intensive care unit and more patient care time for the attending physician.8–9 Pharmacists providing clinical care for patients in a women’s health hospital should have proficient knowledge and skills before practicing independently. A lack of training in obstetric clinical pharmacy may be a limitation to pharmacist involvement in this specialty.4 To advance their clinical skillset in obstetrics, pharmacists who have not completed internship or residency in a women’s hospital12 have sought attendance in seminars and short courses, and many learn through institution-based on-the-job training when working on the obstetric wards providing clinical pharmacy services. Pharmacists providing care to hospital patients should possess the knowledge and skills necessary to make that care safe and effective. The pharmacy department should provide adequate training for all staff members who may be called upon to provide care to hospital patients.
This report aimed to describe the development and implementation of a training tool to increase the knowledge and skillset of obstetric clinical pharmacists in an Australian Principal Referral and Specialist Women Hospital. The objective of the implementation of the training program was to ensure consistency and quality in service delivery.
The study hospital, with 300 beds (including 100 neonatal cots), is the only tertiary maternity and gynecological hospital in the state. More than 6,000 births occur annually, and it is the only major referral center in the state for high-risk pregnancies. The Covid-19 pandemic has created job opportunities in the pharmacy department in the study hospital to cover sickness, staff furlough in the pharmacy and to assist with nursing and midwifery workforce shortages.13 This has resulted in the employment of new pharmacists who had not previously cared for high-risk obstetric patients, and who had not received formal training in caring for either of those types of patients during pharmacy school. The department had to explore an effective clinical pharmacy training program, other than the conventional training which only involved face-to-face and on-the-job training. There was also the concern of training fatigue, with a small team of clinical pharmacists. The pharmacy department did not have the financial resources to invest in the services of staff from a school of pharmacy, so therefore had explored the creation of an in-house training module.
The training program was compiled by the Deputy Chief Pharmacist for Clinical Services as there was no dedicated Staff Development Pharmacist in the department. The development of the training module was prioritized, as accomplishing this task and assuring that our personnel were highly proficient, without compromising patient care, was highly important.
Clinical practice guidelines, policy statements, and other sources were reviewed to guide the development of the training materials. While published training for obstetric clinical pharmacists for other hospital settings was not located, the training program (Figure 1) was compiled according to the national standard of practice in women’s and newborn health for pharmacy services.14 The training program involved an e-Learning package compiled by the pharmacy department, followed by face-to-face teaching, demonstration, and working under supervision. The contents of the e-Learning package are shown in Figure 2.


Figure 1 Clinical Pharmacy Training Log

Figure 2 Modules in the Self-Directed Learning Package
The learning objectives of the training program included: (1) Gain an overview of hospital pharmacy practice; (2) Understand medication management in a clinical setting; (3) Outline the processes involved with medication reconciliation, medication history taking, and discharge medication reconciliation; (4) Describe processes involved with medication supply for in-patients; and (5) Identify resources available to support clinical decisions, and to provide medicine information to healthcare professionals and patients.
The progress of the training was communicated with the pharmacy team via departmental meetings and emails. This enhanced the opportunity for the innovation and development of system-based solutions, and translated to ownership of the process and successful implementation.
This activity was exempted from ethics review, conducted as part of an educational training program for operational requirements, where any outcomes or documentation were provided for training use only.
From August 2023, the trainee pharmacist received the training program outline with the link to the e-Learning package at least one week prior to starting obstetrics clinical training. The trainee pharmacist would complete section one of the training program by accessing the self-directed learning module. One important component of the training is to ensure the pharmacists are familiar with the available information sources, which are readily accessible to all pharmacists, supporting research on medication-related issues, and facilitating the provision of pharmacy care in the medication use process. The self-directed learning module was endorsed by the North Metropolitan Health Services Department of Learning and Development (NMHS L&D) and is published on the L&D training hub. The trainees who completed the program earned a certificate of completion.
Following the self-directed learning modules, the pharmacist would shadow an experienced senior clinical pharmacist on the ward, learning by observation, demonstration and performing the duties under supervision. Finally, the pharmacist would be evaluated using a departmental assessment tool, miniCEX (Figure 3).
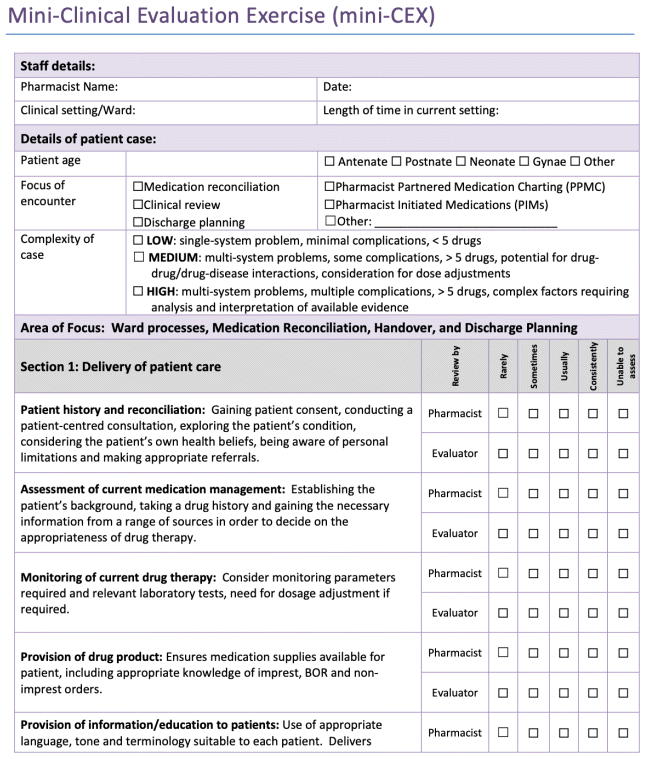


Figure 3 Mini-Clinical Evaluation Exercise (mini-CEX)
MiniCEX evaluates the pharmacists’ skillset while performing medication reconciliation, clinical review, clinical handover and discharge planning. Learning objectives of the training program were reviewed in the delivery of patient care, problem solving and professional skills. We hope the pharmacists are sufficiently skilled to ensure quality and safety of medication management in patient care, emphasizing collaborative care and patient interaction.
From the implementation in August 2023, the department has trained five pharmacists and four intern pharmacists using the new training program. These pharmacists and intern pharmacists were able to meet the departmental requirements, and all have been rostered on the ward areas following the training program. Feedback was sought from the pharmacists following the implementation of new training program in the fortnightly Clinical Pharmacist Meeting. The training program was received positively by the department as the new program was readily accessible online, enabled the trainee to develop basic concepts of clinical pharmacy before being orientated to the ward, and enabled the trainer pharmacist to deliver training more effectively and sustainably in a structured manner.
The implementation of a training program to educate non-residency trained pharmacists in obstetrics enabled the consistent and high quality of pharmacy services, while ensuring the sustainability of the training provided by the department. The training program was designed based on the services offered, departmental size, resources available, and time allotted for training. The training package was a valuable tool to provide established, structured procedure for orienting new personnel to the pharmacy, the hospital and health system.
Inadequate FTEs for training module development and competing responsibilities for the clinical supervisors were among the various challenges of implementation. Other implementation challenges related to the time demands required to complete the self-directed learning training course. This was addressed by recognizing the need of dedicated desktop time for the trainee, instead of starting training on the ward in conventional clinical training. Another limitation of this implementation is the lack of formal evaluation of the effectiveness or impact of the training. Future study in the evaluation, including pre-post self-assessment data or qualitative feedback from participants and trainers, is warranted. The user experience of the initiative is specific to a single hospital, with a small number of staff, therefore the formal recognition and applicability needs to be conducted with a larger number of pharmacists to ensure institutional utility in other settings.
Our experience in developing and implementing the education model fostered the transition to structured training in obstetric clinical pharmacy. Through these activities, we hope to further develop pharmacists’ knowledge and skills necessary to make that care safe and effective for the patient, and that they are competent and feel more confident in performing clinical pharmacy services.
The unique challenges of the maternity population require careful consideration for hospital pharmacists and pharmacy departments. The pharmacy department must ensure the clinical pharmacy services meet the needs for obstetric populations. The implementation of a training program to educate pharmacists in obstetric clinical services helped to ensure consistency and competency in the service provision of clinical pharmacists, while ensuring the sustainability of training in the department.
The authors would like to acknowledge Ms Susan Shearer and Ms Claire Broderick for their contributions in the compilation of clinical pharmacy training log. The authors would also like to acknowledge the Pharmacy Department at Fiona Stanley Hospital in Western Australia and Ms Melanie Utting for sharing their Mini-Clinical Evaluation Exercise (MiniCEX). The authors would also like to thank Ms Claire Broderick for developing the MiniCEX in the study hospital.
1. Curtin University. (2025) Undergraduate: Bachelor of Pharmacy. Available from: https://www.curtin.edu.au/study/offering/course-ug-bachelor-of-pharmacy-honours--bh-pharm/
2. University of Western Australia. (2025) Undergraduate and Postgraduate: Bachelor of Human Sciences (Pharmaceutical Health) and Master of Pharmacy. Available from: https://www.uwa.edu.au/study/courses/bachelor-of-human-sciences-pharmaceutical-health-and-master-of-pharmacy
3. Kvarnström K, Niittynen I, Kallio S, Lindén-Lahti C, Airaksinen M, Schepel L. (2023). Developing an in-house comprehensive medication review training program for clinical pharmacists in a finnish hospital pharmacy. International Journal of Environmental Research and Public Health. 20(12):6158. https://doi.org/10.3390/ijerph20126158. PMID: 37372745; PMCID: PMC10298518.
Crossref PubMed PMC
4. Gnadt S. (2020). Clinical pharmacy and obstetrics. American Journal of Health-System Pharmacy. 77(23):1941–1944. https://doi.org/10.1093/ajhp/zxaa289
Crossref PubMed
5. Urbańczyk K, Guntschnig S, Antoniadis V, Falamic S, Kovacevic T, Kurczewska-Michalak M, Miljković B, Olearova A, Sviestina I, Szucs A, Tachkov K. (2023). Recommendations for wider adoption of clinical pharmacy in Central and Eastern Europe in order to optimise pharmacotherapy and improve patient outcomes. Frontiers in Pharmacology. Aug 2;14:1244151.
Crossref
6. Lin HW, Yang LC, Mafruhah OR, Nguyen HT, Cao TT, Yam FK. (2020). Evolution of clinical pharmacy practice and pharmacy education in Taiwan, Vietnam, and Indonesia: A narrative review. Journal of the American College of Clinical Pharmacy. Aug;3(5):947–58.
Crossref
7. Doloresco F, Vermeulen LC. (2009) Global survey of hospital pharmacy practice. American Journal of Health-System Pharmacy. Mar 1;66(5_Supplement_3):s13–9.
Crossref PubMed
8. Briggs GG. Pharmacists in obstetrics. (2018). American Journal of Health-System Pharmacy. 75(3):92. doi:10.2146/ajhp170662. PMID: 29371188.
Crossref PubMed
9. Small, S. M., Paratore, P. D., Peterson, S. D., Lucia, R. A., Reiter, P. D. (2023). Obstetric clinical pharmacy: A necessary birth of a new specialty. American Society of Health-System Pharmacists, 80(15), 1026–1031. https://doi.org/10.1093/ajhp/zxad092
Crossref
10. Temple ME, Jakubecz MA, Link NA. (2013) Implementation of a training program to improve pharmacy services for high-risk neonatal and maternal populations. American Journal of Health-Systems Pharmacy. 70(2):144–9. https://doi.org/10.2146/ajhp110681. PMID: 23292268.
PubMed
11. Ragland D, Briggs GG, Wasik M et al. (2012). Obstetrical opportunities: will pharmacy ever realize them? Annals of Pharmacotherapy. 46:297–300. https://pubmed.ncbi.nlm.nih.gov/22298603/
Crossref PubMed
12. Advanced Pharmacy Australia. (2025) Resident Training Program – accredited hospital pharmacy sites. Available from: https://prod.shpa.bond.software/workforce-research/training-programs/accreditation/training-program-accreditation---hospital-pharmacy/accredited-sites
13. Mukadam N, Ferenti MF, Teoh SWK, Banka M. (2024). Obstetric assistant pharmacist: innovative workforce solution during surges in workforce shortage and demand. Global Journal On Quality And Safety In Healthcare 7 (3): 115–117. https://doi.org/10.36401/JQSH-23-43
Crossref PubMed PMC
14. Dwyer J, Clark M, Grzeskowiak L, Lau C, Lebedevs T, Luttrell K, McGuire T, O’Hara K, Soo JY, Mellor Y. Standard of practice in women’s and newborn health for pharmacy services. Journal of Pharmacy Practice and Research. 2024 Aug;54(4):333–51. https://doi.org/10.1002/jppr.1941
Crossref
© Education for Health.
Education for Health | Volume 38, No. 3, July-September 2025