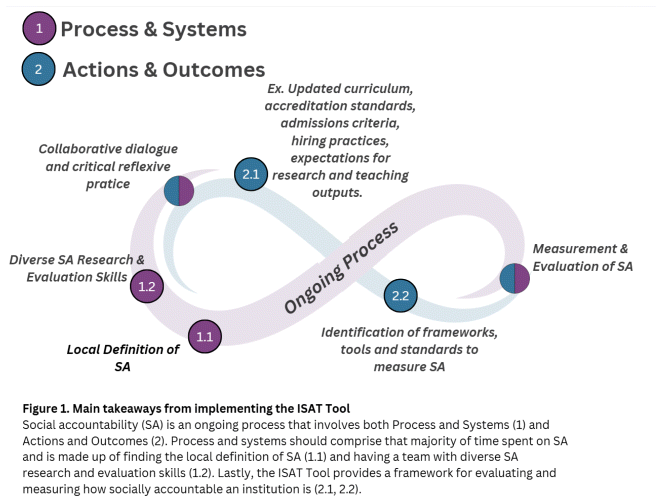
Figure 1 Main takeaways from implementing the ISAT Tool
Sophia Myles1, Chandelle Mensour2, Kerri Z. Delaney3, and Erin Cameron4
1PhD, Adjunct Professor, School of Kinesiology and Health Sciences, Laurentian University, Sudbury, Canada
2MD, Resident, Department of Family Medicine, The Northern Ontario School of Medicine University, Thunder Bay and Sudbury, Canada
3PhD, Postdoctoral Fellow, The Dr. Gilles Arcand Centre for Health Equity, The Northern Ontario School of Medicine University, Thunder Bay, Canada
4PhD, Associate Professor, Medical Education, Director, The Dr. Gilles Arcand Centre for Health Equity, The Northern Ontario School of Medicine University, Thunder Bay, Canada
ABSTRACT
Social accountability has become a key driver of change within health professional education programs worldwide. Over the last two decades, there has been a growing number of frameworks, tools, and standards to help measure social accountability. This paper shares the experiences and lessons learned from one of the institutions that participated in piloting the Institutional Self-Assessment Social Accountability Tool (ISAT). We argue that tools for measuring social accountability are valuable not only because they provide data but, more importantly, because they can embed a dialogic and critical reflective culture within institutions. We describe how the tool expanded our thinking about social accountability to advance it, including what constitutes socially accountable research and who and what fields contribute to this work. We argue that the tool encouraged collaborative critical reflexive practice and offered a process that was incorporated into institutional processes and activities, and simultaneously fostered intra-institutional cooperation. Finally, we contend that the application of quality and equity lenses offers sources of sustainability to advance social accountability in medical education as they encourage the prioritization of social accountability processes to achieve desired outcomes.
Key Words: social accountability, accreditation, medical education, continuous quality improvement, equity
Date submitted: 5-March-2025
Email:Erin Cameron (ercameron@nosm.ca)
This is an open access journal, and articles are distributed under the terms of the Creative Commons Attribution-Non Commercial-Share Alike 4.0 License, which allows others to remix, tweak, and build upon the work non-commercially, as long as appropriate credit is given and the new creations are licensed under the identical terms.
Citation: Myles S, Mensour C, Delaney K, and Cameron E. Applying quality and equity lenses to advance social accountability in medical education. Educ Health 2025;38:187-196
Online access: www.educationforhealthjournal.org
DOI: 10.62694/efh.2025.294
Published by The Network: Towards Unity for Health
Social accountability has become a key driver of change within health professional education programs worldwide.1,2 Increasingly, educational institutions are adopting social accountability missions and mandates3,4 and embedding these within curricula5,6 and accreditation frameworks.7–9 Additionally, health institutions are including social accountability in strategic plans and organizational structures.10,11 At its core, social accountability is about collaborating with local stakeholders to reimagine and reorient institutions to better co-identify and co-address local health and social priorities.12 While there is global consensus for social accountability, and few dispute its value, there is a growing need for critical conversations about measuring and evaluating the impact of social accountability in health professional education.2,13,14
Over the last two decades, there has been a growing number of frameworks, tools, and standards to help measure social accountability.15–20 For example, medical residents have been surveyed21 and checklists have been developed to identify ways for medical schools22 and students23 to assess the extent to which their school is being socially accountable. Recommendations to enhance social accountability in graduate medical education have also been made.21,24 Predominantly, these tools have taken a self-assessment approach, given that the nature of social accountability is contextually dependent. While helpful in generating data, many institutional and programmatic self-assessment tools also provide valuable opportunities for dialogic reflections—a gap within the field. This paper aims to share the experiences and lessons learned from one of the institutions that participated in piloting a new social accountability tool—the Institutional Self-Assessment Social Accountability Tool (ISAT). We will argue that tools for measuring social accountability are valuable not only because they provide data but, more importantly, because they can embed a dialogic and critical reflective culture within institutions.
In 2021, 10 institutions participated in an international project to pilot a new social accountability self-assessment tool within its undergraduate medical education (UME) program.25–27 NOSM U was founded on a social accountability mandate to improve the health of Northern Ontario28,29 and to address a persistent shortage of health professionals in the region.30,31 NOSM U is organized, structured, and designed as a campus for the North, with over 90 partnership communities.32,33 Scholars and leaders at NOSM U have called for critical reflexive practice and the need to consider how institutional processes and activities are continuously meeting the needs of, or impacting, those they serve.34–37
The tool, referred to as the Institutional Self-Assessment Social Accountability Tool (ISAT), was developed by a team of international social accountability leaders, educators, and evaluators and supported by the Pan American Health Organization (PAHO), The Training for Health Equity Network (THEnet), The Network: Towards Unity for Health (TUFH), and Beyond Flexner Alliance (BFA). The ISAT tool was developed to assist institutions in measuring the extent to which they are, and can become more, socially accountable to the public, communities, and people they serve.25,38 To learn more about the ISAT tool, visit https://socialaccountabilityhealth.org/.
NOSM U’s process for implementing the ISAT tool involved reaching out to the NOSM University community for assistance and in identifying leads to gather relevant information to populate each domain of the ISAT tool. A survey was created based on the questions and indicators for each domain of the ISAT tool: (1) identify relevant information, (2) identify supplemental documents, and (3) identify complementary processes (i.e., accreditation, strategic planning performance reviews). Over several months, the information collected was collated and reviewed. A steering committee of domain leads, faculty and medical students reviewed and provided feedback on the self-assessment within each domain before submission. NOSM U’s project leads subsequently participated in an interview with the ISAT review committee, which evaluated the content of the submission, asked questions, and provided feedback on the self-assessment. NOSM U’s results can be found at https://socialaccountabilityhealth.org/institute-list/nosm-northern-ontario-school-of-medicine/.
After completing the process, three members of the NOSM U team (a faculty member, a postdoctoral fellow, and a medical student) reflected on their own experiences in the process and together identified three key lessons learned.
While NOSM U is well known for its social accountability mandate,2,28,29 like all institutions, it must continue to work towards, strive for, and advance efforts to meet the needs of the people, populations, and communities they serve. As communities’ health and social needs and priorities continue to change, which has never been as demonstrably necessary as during the COVID-19 pandemic, schools like NOSM U must continue to adapt and evolve in tandem with their communities (Figure 1). It is incumbent on schools to continuously evaluate, assess, and reflect on how, or the extent to which, they serve and represent communities in a meaningful and equitable way. Approaching programmatic and institutional assessments for social accountability with both an equity and continuous quality improvement (CQI) lens for medical education and research “can improve medical education and help it achieve its goals.”39 Employing CQI for program evaluation, with the added lens of equity, can also be helpful for other assessments such as accreditation.40–44

Figure 1 Main takeaways from implementing the ISAT Tool
There is potential to reconceptualize and redefine social accountability within and among institutions. A recent narrative review conducted to identify implementations of socially accountable medical education found that the World Health Organization’s definition and meaning of social accountability15 has been widely adopted by medical schools with social accountability mandates.45 Despite this seemingly ubiquitous application, inherent in the literature is diverse terminology, including “social responsibility,” “social responsiveness,” “social obligation,”20,46 “social mission,”22 and “social contract”47,48 that relates to, and is potentially used interchangeably with, “social accountability”. Conceptual slippage might result in stakeholders talking past each other in discussions about social accountability. It might also reflect just how complex, contextually specific, and nuanced this construct is.45
Standardization is essential for practical and policy purposes such as accreditation, emphasizing uniformity and comparability of institutions45 as a measure of educational quality and effectiveness, practitioner competence for further training or practice preparedness, and public confidence and trust.49–54 However, it is equally important to encourage an understanding of how different stakeholders approach social accountability and the versions, uses, and meanings they ascribe to it. During our document gathering and community and steering committee consultation process, it became evident that social accountability can be thought about differently and mean different things to different people, even within a single institution (Figure 1). It is, therefore, important to consider who is included in, and actively contributes to, discussions about social accountability. It is also important to encourage broad participation of internal and external stakeholders in these discussions, as well as to ask who is or should be a stakeholder, and who is missing that needs a seat at the table for knowledge brokering purposes.
Socially accountable research is usually framed as community-based participatory research (CBPR). With its underlying philosophies of equity and social justice,55 CBPR engages with communities as research partners and builds capacity through participatory and codesign methods.56 It directly addresses issues of power56 between “the researcher and the researched”57 and is used mainly when working with marginalized populations.58 If a primary goal of social accountability in health professional education and research is to address priority community health concerns or needs,11,59,60 we argue there is room for different methods and methodologies beyond just CBPR.61–63 While the ISAT tool specifically refers to community-based research, it also requires schools to demonstrate educational outcomes and societal impacts. This opens opportunities for other types of research, such as longitudinal multi-cohort studies that follow graduates from admissions into practice.
While articulating NOSM U’s current activities and action plan to advance social accountability through research, it became clear that socially accountable research does not ‘belong’ to one ontological or epistemological perspective and associated methods; this unnecessarily limits the questions that may be asked, the approaches used to answer them, the problems that may be identified, and the potential solutions to address them. This also implies that social accountability is not everyone’s responsibility. Pertinently, it was apparent that relationship and partnership building within and beyond institutions is essential to conducting socially accountable research (Figure 1). One might refer to variations of the Partnership Pentagram15,37,64–66 to continually assess who to engage for particular projects.
Social accountability is the foundation of the medical profession’s social contract with society,11 and by extension, the practice of medicine and medical schools.67 Opinions differ about the importance of individual elements of medical school mandates,68 and difficulty in measuring social accountability is frequently identified as a barrier to attaining the social contract.69 If medical schools focus too much on actions and outcomes of being socially accountable and pay insufficient attention to the processes and systems they use to be socially accountable, there is potential to undermine the impact of this philosophy used to educate and train physicians at the institutional level.45
In part, social accountability processes aim to hold accountable those responsible for quality service provision.70 They can be considered complex interventions with several interrelated components, actors, decisions, steps, and change processes.71 As social accountability is a relational process between medical schools and the populations and communities they serve, interventions adapt as they are implemented in specific places.70,72 Failure to adapt place-specific social accountability strategies and activities might result in not conforming to pre-set interventions.70
The ISAT tool is not only a tool, but is a process medical schools can use to engage in critical reflexive practice at the institutional level to internally measure and assess their “process of being accountable.”45 Such self-reflection and - assessments can promote intra-institutional cooperation and dialogue within and across units to inform existing and future quality improvement (QI) processes or platforms, such as accreditation, curriculum development and delivery, or the creation of new social accountability frameworks. Increasing quality measures conducted in isolation may result in the transfer of resources from quality improvement to other quality-performance metrics that might have unintended consequences for the things medical schools and communities aim to achieve.73 Ideally, quality measurement and QI will lead to educational and programmatic improvements and tangible changes required to graduate socially accountable physicians, meaningfully improving patients’ and communities’ engagement with healthcare systems and resulting outcomes from this engagement.74
To facilitate such outcomes, quality and equity lenses such as CQI and social accountability, when applied, can serve as an anchor and source of stability for research in medical education. Socially accountable medical education research can explore how to balance QI activities in a way that allows medical schools to assess quality, cost performance, and outcomes of social accountability initiatives with appropriate metrics.73 Lastly, social accountability research and QI activities might be directed to investigate and assess the implications of increasingly incorporating artificial intelligence to deliver curriculum or engage with communities virtually.75
NOSM U’s pilot test of the ISAT tool for its UME program to advance social accountability metrics in health professions education presented an extremely useful opportunity for critical reflexive practice. The ISAT tool allowed for reflection on the school’s foundational social accountability mandate, how this has been implemented and reflected in NOSM U’s institutional programming, processes, activities, and outcomes, and identifying improvement or change areas.
As a result of these reflections, we learned that social accountability is something that medical schools must continue to work towards as the health and social needs and priorities of the communities they serve change. We also learned that there is potential to expand our thinking about social accountability to advance it, including what constitutes socially accountable research as well as who and what fields produce this work, and that this construct might be reconceptualized and redefined within and among singular institutions; such definitions should be devised locally.
Critical reflexive practice, including self-reflection and self-assessment, offers a process that can be incorporated into institutional processes and activities and simultaneously foster intra-institutional cooperation. The application of quality and equity lenses can be sources of sustainability to advance social accountability in medical education, in that they can encourage the prioritization of social accountability processes to achieve desired outcomes.
1. Ventres W, Boelen C, Haq C. Time for action: key considerations for implementing social accountability in the education of health professionals. Advances in Health Sciences Education. 2018; 23(4): 853–862. https://doi.org/10.1007/s10459-017-9792-z.
Crossref
2. Noya F, Carr S, Thompson S. Social accountability in a medical school: is it sufficient? A regional medical school curriculum and approaches to equip graduates for rural and remote medical services. BMC Medical Education. 2024; 24(1): 526–536. https://doi.org/10.1186/s12909-024-05522-y.
Crossref PubMed PMC
3. Ross BM. The socially accountable professor in higher education. Journal of Education and Learning. 2018; 7(5): 181–187. https://doi.org/10.5539/jel.v7n5p181.
Crossref
4. Noya FC, Carr SE, Thompson SC. Attracting, recruiting, and retaining medical workforce: a case study in a remote province of Indonesia. International Journal of Environmental Research and Public Health. 2023; 20(2): 1435–1453. https://doi.org/10.3390/ijerph20021435.
Crossref PubMed PMC
5. Guignona M, Halili S, Cristobal F, Woolley T, Reeve C, Ross SJ, Neusy A-J. A curriculum for achieving Universal Health Care: a case study of Ateneo de Zamboanga University School of Medicine. Frontiers in Public Health. 2021; 9: 612035. https://doi.org/10.3389/fpubh.2021.612035.
Crossref PubMed PMC
6. Karunathilake I, Kristina TN. Curriculum design of community-based education, toward social accountability of health profession education. In: Claramita M, Findyartini A, Samarasekera DD, Nishigori H, editors. Challenges and opportunities in health professions education: perspectives in the context of cultural diversity. Singapore: Springer Nature Singapore; 2022. p. 87–109.
Crossref
7. Walling E, Lachance E, Yeo L, Koepke K, Wasik A, Woollard R. Key drivers of social accountability in nine Canadian medical schools. Medical Teacher. 2021; 43(2): 182–188. https://doi.org/10.1080/0142159X.2020.1832205.
Crossref
8. Sayek I, Turan S, Batı AH, Demirören M, Baykan Z. Social accountability: a national framework for Turkish medical schools. Medical Teacher. 2021; 43(2): 223–231. https://doi.org/10.1080/0142159X.2020.1841889.
Crossref
9. Puschel K, Riquelme A, Sapag J, Moore P, Díaz LA, Fuentes-López E, Burdick W, Norcini J, Jiménez de la Jara J, Campos H, Valdez JE, Llosa MP, Lamus-Lemus F, Yulitta H, Grez M. Academic excellence in Latin America: Social accountability of medical schools. Medical Teacher. 2020; 42(8): 929–936. https://doi.org/10.1080/0142159X.2020.1770712.
Crossref PubMed
10. Boelen C, Woollard B. Social accountability and accreditation: a new frontier for educational institutions. Medical Education. 2009; 43(9): 887–894. https://doi.org/10.1111/j.1365-2923.2009.03413.x.
Crossref PubMed
11. Rourke J. Social accountability: a framework for medical schools to improve the health of the populations they serve. Academic Medicine. 2018; 93(8): 1120–1124. https://doi.org/10.1097/ACM.0000000000002239.
Crossref PubMed
12. Boelen C, Blouin D, Gibbs T, Woollard R. Accrediting excellence for a medical school’s impact on population health. Education for Health. 2019; 32(1): 41–48. https://doi.org/10.4103/efh.EfH_204_19.
Crossref PubMed
13. Leinster S. Evaluation and assessment of social accountability in medical schools. Medical Teacher. 2011; 33(8): 673–676. https://doi.org/10.3109/0142159X.2011.590253.
Crossref PubMed
14. Reeve C, Woolley T, Ross SJ, Mohammadi L, Halili Jr SB, Cristobal F, Siega-Sur JL, Neusy AJ. The impact of socially-accountable health professional education: a systematic review of the literature. Medical Teacher. 2017; 39(1): 67–73. https://doi.org/10.1080/0142159X.2016.1231914.
Crossref
15. Boelen C, Heck JE. Defining and measuring the social accountability of medical schools. Geneva: World Health Organization Division of Development of Human Resources for Health; 1995.
16. Larkins SL, Preston R, Matte MC, Lindemann IC, Samson R, Tandinco FD, Buso D, Ross SJ, Pálsdóttir B, Neusy AJ, on behalf of the Training for Health Equity Network (THEnet). Measuring social accountability in health professional education: development and international pilot testing of an evaluation framework. Medical Teacher. 2013; 35(1): 32–45. https://doi.org/10.3109/0142159X.2012.731106.
Crossref
17. Ross SJ, Preston R, Lindemann IC, Matte MC, Samson R, Tandinco FD, Larkins SL, Palsdottir B, Neusy AJ. The training for health equity network evaluation framework: a pilot study at five health professional schools. Education for Health. 2014; 27(2): 116–126. https://doi.org/10.4103/1357-6283.143727.
Crossref PubMed
18. Abdalla ME. Suggested new standards to measure social accountability of medical schools in the accreditation systems. Journal of Case Studies in Accreditation and Assessment. 2014; 3. Available from: https://files.eric.ed.gov/fulltext/EJ1060602.pdf
19. Barber C, Van Der Vleuten C, Leppink J, Chahine S. Social accountability frameworks and their implications for medical education and program evaluation: a narrative review. Academic Medicine. 2020; 95(12): 1945–1954. https://doi.org/10.1097/ACM.0000000000003731.
Crossref PubMed
20. Boelen C, Dharamsi S, Gibbs T. The social accountability of medical schools and its indicators. Education for Health. 2012; 25(3): 180–194. https://doi.org/10.4103/1357-6283.109785.
Crossref
21. Bradley LJ, Clem J, Godsil R, MacFarlane J, Foster PP. Racial anxiety among medical residents: institutional implications of social accountability. Journal of Health Care for the Poor and Underserved. 2019; 30(4 Suppl): 105–115. https://doi.org/10.1353/hpu.2019.0121.
Crossref PubMed PMC
22. Batra S, Orban J, Guterbock TM, Butler LA, Mullan F. Social mission metrics: developing a survey to guide health professions schools. Academic Medicine. 2020; 95(12): 1811–1816. https://doi.org/10.1097/ACM.0000000000003324.
Crossref PubMed PMC
23. Dijk S, Glasner J, Purdy K, Bhiri M, Ramalho R, Ross S. Social accountability in medical schools: student toolkit [Internet]. International Federation of Medical Students’ Association; 2017. Retrieved February 20, 2022, from https://ifmsa.org/wp-content/uploads/2017/09/Toolkit-on-Social-Accountability_Final-v.32.pdf
24. Kaufman A, Scott M, Andazola J, Fitzsimmons-Pattison D, Parajón L. Social accountability and graduate medical education. Family Medicine. 2021; 53(7): 632–637. https://doi.org/10.22454/FamMed.2021.160888.
PubMed
25. Utomo PS, Govender K, De Kempeneer A, Torres N. The Institutional Self-Assessment Social Accountability Tool (ISAT): nurturing social accountability progress in medical and health professions education. Social Innovations Journal. 2022; 14(4). Available from https://socialinnovationsjournal.com/index.php/sij/article/view/3763
26. Hatcher S, Cyr J, Girard J. The ISAT Self-Assessment Tool for social accountability of faculties of medicine: from theory to practice. Social Innovations Journal. 2023; 21. Available from https://socialinnovationsjournal.com/index.php/sij/article/view/6790
27. Gulf Medical University. QA IE unit workshop: Institutional Self-Assessment Social Accountability Tool (ISAT) [Internet]; 2022. Retrieved December 27, 2024, from https://gmu.ac.ae/qa_news/qaie-unit-workshop-institutional-self-assessment-social-accountability-tool-isat/
28. Strasser R, Lanphear J, McCready W, Topps M, Hunt D, Matte M. Canada’s new medical school: the Northern Ontario School of Medicine – social accountability through distributed community engaged learning. Academic Medicine. 2009; 84(10): 1459–1464. https://doi.org/10.1097/ACM.0b013e3181b6c5d7.
Crossref PubMed
29. Ross B. Critical pedagogy as a means to achieving social accountability in medical education. International Journal of Critical Pedagogy. 2015; 6(2): 169–186.
30. Glazier RH, Gozdyra P, Yeritsyan N. Geographic access to primary care and hospital services for rural and northern communities: report to the Ontario Ministry of Health and Long-Term Care [Internet]. Toronto: Institute for Clinical Evaluative Sciences; 2011. Retrieved February 20, 2022, from: https://www.ices.on.ca/wp-content/uploads/2023/06/Full-report-32.pdf
31. Health Quality Ontario. Health in the North: a report on geography and the health of people in Ontario’s two northern regions [Internet]. Toronto: Springer; 2017. Retrieved February 20, 2022 from: http://www.hqontario.ca/portals/0/Documents/system-performance/health-in-the-north-en.pdf
32. Strasser R. Delivering on Social accountability: Canada’s Northern Ontario School of Medicine. The Asia-Pacific Scholar. 2016; 1(1): 1–6. https://doi.org/10.29060/TAPS.2016-1-1/OA1014.
Crossref
33. Strasser R, Hogenbirk J, Jacklin K, Maar M, Hudson G, Warry W, Cheu H, Dubé T, Carson D. Community engagement: a central feature of NOSM’s socially accountable distributed medical education. Canadian Medical Education Journal. 2018; 9(1): e33–e43. PMID: 30140333.
Crossref
34. Hogenbirk JC, Timony PE, French MG, Strasser RP, Pong RW, Cervin C, Graves L. Milestones on the social accountability journey: family medicine practice locations of Northern Ontario School of Medicine graduates. Canadian Family Physician. 2016; 62: e138–e145. PMID: 27427565.
PubMed PMC
35. Wenghofer EF, Hogenbirk JC, Timony PE. Impact of the rural pipeline in medical education: practice locations of recently graduated family physicians in Ontario. Human Resources for Health. 2017; 15(1): 16. https://doi.org/10.1186/s12960-017-0191-6.
Crossref PubMed PMC
36. Hogenbirk JC, Robinson DR, Strasser RP. Distributed education enables distributed economic impact: the economic contribution of the Northern Ontario School of Medicine to communities in Canada. Health Economics Review. 2021; 11(1): 20. https://doi.org/10.1186/s13561-021-00317-z.
Crossref PubMed PMC
37. Markham R, Hunt M, Woollard R, Oelke N, Snadden D, Strasser R, Betkus G, Graham S. Addressing rural and Indigenous health inequities in Canada through socially accountable health partnerships. BMJ Open. 2021; 11(11): e048053. https://doi.org/10.1136/bmjopen-2020-048053.
Crossref PubMed PMC
38. The Network: Toward Unity for Health. Indicators for social accountability tool in health profession education. Self assessment guide and tool. Authors; 2024. Retrieved October 3, 2024, from: https://socialaccountabilityhealth.org/wp-content/uploads/2024/03/ISAT_2.0_Implementation_Guide_ENGLISH.pdf
39. Wong BM, Headrick LA. Application of continuous quality improvement to medical education. Medical Education. 2021; 55(1): 72–81. https://doi.org/10.1111/medu.14351.
Crossref
40. Barzansky B, Hunt D, Moineau G, Ahn D, Lai CW, Humphrey H, Peterson L. Continuous quality improvement in an accreditation system for undergraduate medical education: benefits and challenges. Medical Teacher. 2015; 37(11): 1032–1038. https://doi.org/10.3109/0142159X.2015.1031735.
Crossref PubMed
41. Akdemir N, Peterson LN, Campbell CM, Scheele F. Evaluation of continuous quality improvement in accreditation for medical education. BMC Medical Education. 2020; 20(1): 1–6. https://doi.org/10.1186/s12909-020-02124-2.
Crossref
42. Prihatiningsih TS, Kamal Y, Woollard R, Fisher J, Abdalla ME, Boelen C. Social accountability and accreditation: impacting health system performance and population health. Social Innovations Journal. 2020; 3. Available from: https://socialinnovationsjournal.com/index.php/sij/article/view/528
43. Ahn D. Current trend of accreditation within medical education. Journal of Educational Evaluation for Health Professions. 2020; 17: 30. https://doi.org/10.3352/jeehp.2020.17.30.
Crossref PubMed PMC
44. Orban J, Xue C, Raichur S, Misak M, Nobles A, Casimir J, Batra S. The scope of social mission content in health professions education accreditation standards. Academic Medicine. 2022; 97(1): 111–120. https://doi.org/10.1097/ACM.0000000000004437.
Crossref
45. Ross BM, Cameron E. Socially accountable medical education: our story might not be yours. Higher Education Studies. 2021; 11(1): 114–120. Available from: https://files.eric.ed.gov/fulltext/EJ1288775.pdf
Crossref
46. Abdolmaleki M, Yazdani S, Momeni S, Momtazmanesh N. Social accountable medical education: a concept analysis. Journal of Advances in Medical Education Professionalism. 2017; 5(3): 108–115. PMID: 28761884.
PubMed PMC
47. Dharamsi S, Ho A, Spadafora SM, Woollard R. The physician as health advocate: translating the quest for social responsibility into medical education and practice. Academic Medicine. 2011; 86(9): 1108–1113. https://doi.org/10.1097/ACM.0b013e318226b43b.
Crossref PubMed
48. Buchman S, Woollard R, Meili R, Goel R. Practising social accountability: from theory to action. Canadian Family Physician. 2016; 62(1): 15–18. PMID: 26796826.
PubMed PMC
49. Blouin D, Tekian A, Kamin C, Harris IB. The impact of accreditation on medical schools’ processes. Medical Education. 2018; 52(2): 182–191. https://doi.org/10.1111/medu.13461.
Crossref
50. Shiffer CD, Boulet JR, Cover LL, Pinsky WW. Advancing the quality of medical education worldwide: ECFMG’s 2023 medical school accreditation requirement. Journal of Medical Regulation. 2019; 105(4): 8–16. https://doi.org/10.30770/2572-1852-105.4.8.
Crossref
51. Blouin D. Accreditation of Canadian undergraduate medical education programs: a study of measures of effectiveness. Academic Medicine. 2020; 95(6): 931–937. https://doi.org/10.1097/ACM.0000000000003065.
Crossref
52. Javidan AP, Raveendran L, Rai Y, Tackett S, Kulasegaram KM, Whitehead C, Rosenfield J, Houston P. Fostering trust, collaboration, and a culture of continuous quality improvement: a call for transparency in medical school accreditation. Canadian Medical Education Journal. 2020; 11(5): e102–e108. https://doi.org/10.36834/cmej.70061.
PubMed PMC
53. Bedoll D, van Zanten M, McKinley D. Global trends in medical education accreditation. Human Resources for Health. 2021; 19(1): 70. https://doi.org/10.1186/s12960-021-00588-x.
Crossref PubMed PMC
54. Baniadam K, Arfeen Z, Rashid MA, Ho MJ, Tackett S. Public availability of information from WFME-recognized accreditation agencies. Human Resources for Health. 2021; 19(1): 78. https://doi.org/10.1186/s12960-021-00621-z.
Crossref PubMed PMC
55. Wilson E. Community-based participatory action research. In: Liamputtong P, editor. Handbook of research methods in health social sciences. Singapore: Springer; 2019.
Crossref
56. Baum F, MacDougall C, Smith D. Glossary: Participatory action research. Journal of Epidemiology and Community Health. 2006; 60(10): 854–857. https://doi.org/10.1136/jech.2004.028662.
Crossref PubMed PMC
57. Tremblay MC, Martin DH, McComber AM, McGregor A, Macaulay AC. Understanding community-based participatory research through a social movement framework: a case study of the Kahnawake Schools Diabetes Prevention Project. BMC Public Health. 2018; 18(1): 1–7. https://doi.org/10.1186/s12889-018-5412-y.
Crossref
58. Cargo M, Mercer SL. The value and challenges of participatory research: strengthening its practice. Annual Review of Public Health. 2008; 29(1): 325–350. https://doi.org/10.1146/annurev.publhealth.29.091307.083824.
Crossref PubMed
59. Boelen C. Coordinating medical education and health care systems: the power of the social accountability approach. Medical Education. 2018; 52(1): 96–102. https://doi.org/10.1111/medu.13394.
Crossref
60. Fitzgerald M, Shoemaker E, Ponka D, Walker M, Kendall C. Global health and social accountability: an essential synergy for the 21st century medical school. Journal of Global Health. 2021; 11: 03045. https://doi.org/10.7189/jogh.11.03045.
Crossref PMC
61. Pearson D, Walpole S, Barna S. Challenges to professionalism: social accountability and global environmental change. Medical Teacher. 2015; 37(9): 825–830. https://doi.org/10.3109/0142159X.2015.1044955.
Crossref PubMed
62. Marill MC. Pressured by students, medical schools grapple with climate change: medical students see gaps in the curriculum and work to fill them. Health Affairs. 2020; (39)12: 2050–2055. Available from: https://www.healthaffairs.org/doi/full/10.1377/hlthaff.2020.01948
Crossref
63. Bekti RSAW. Linking social entrepreneur education to strengthen a medical school’s social accountability mission. Social Innovations Journal. 2020; 3. Available from: https://socialinnovationsjournal.com/index.php/sij/article/view/457
64. Boelen C. Towards unity for health: challenges and opportunities for partnership in health development: a working paper [Internet]. Geneva: World Health Organization; 2000. Retrieved February 24, 2022, from: https://apps.who.int/iris/bitstream/handle/10665/66566/WHO_EIP_OSD_2000.9.pdf?sequence=1isAllowed=y
65. Woollard RF. Caring for a common future: medical schools’ social accountability. Medical Education. 2006; 40(4): 301–313. https://doi.org/10.1111/j.1365-2929.2006.02416.x.
Crossref PubMed
66. Agarwal S, Heltberg R, Diachok M. Scaling-up social accountability in world bank operations. Washington, DC: World Bank; 2009.
67. Rourke J. Last page: social accountability of medical schools. Academic Medicine. 2013; 88(3): 430. https://doi.org/10.1097/ACM.0b013e3182864f8c.
Crossref
68. Hall J, Mirza R, Gill P. Leading the way toward a socially-accountable medical education system. Canadian Medical Education Journal. 2019; 10(1): e128–e131. PMID: 30949268.
Crossref PubMed PMC
69. Mullan F, Chen C, Petterson S, Kolsky G, Spagnola M. The social mission of medical education: ranking the schools. Annals of Internal Medicine. 2010; 152(12): 804–811. https://doi.org/10.7326/0003-4819-152-12-201006150-00009.
Crossref PubMed
70. Boydell V, McMullen H, Cordero J, Steyn P, Kiare J. Studying social accountability in the context of health system strengthening: innovations and considerations for future work. Health Research Policy and Systems. 2019; 17(1): 1–6. https://doi.org/10.1186/s12961-019-0438-x.
Crossref
71. Moore G, Audrey S, Barker M, Bond L, Bonell C, Cooper C, Hardeman W, Moore L, O’Cathain A, Tinati T, Wight D. Process evaluation in complex public health intervention studies: the need for guidance. Journal of Epidemiology and Community Health. 2014; 68(2): 101–102. https://doi.org/10.1136/jech-2013-202869.
Crossref
72. Moncrieffe J. Relational accountability: complexities of structural injustice. Bloomsbury Publishing; 2011.
Crossref
73. Meyer GS, Nelson EC, Pryor DB, James B, Swensen SJ, Kaplan GS, Weissberg JI, Bisognano M, Yates GR, Hunt GC. More quality measures versus measuring what matters: a call for balance and parsimony. BMJ Quality Safety. 2012; 21(11): 964–968. https://doi.org/10.1136/bmjqs-2012-001081.
Crossref PubMed PMC
74. Margolius D, Ranji SR. Quality improvement, quality measurement and medical education: a brewing culture clash? BMJ Quality Safety. 2015; 24(8): 477–479. https://doi.org/10.1136/bmjqs-2015-004482.
Crossref PubMed
75. Anawati A, Fleming H, Mertz M, Bertrand J, Dumond J, Myles S, Leblanc J, Ross B, Lamoureux D, Patel D, Carrier R, Cameron E. Artificial intelligence and social accountability in the Canadian health care landscape: A rapid literature review. PLOS Digital Health. 2024; 3(9): e0000597. https://doi.org/10.1371/journal.pdig.0000597.
Crossref PubMed PMC
© Education for Health.
Education for Health | Volume 38, No. 2, April-June 2025