Sam Woodworth1 and Christopher Smith2
1MD, Clinical Assistant Professor in the Department of Medicine, Tufts University School of Medicine, Division of Hospital Medicine, Maine Medical Center, Portland, United States
2MD, Associate Professor of Medicine, Harvard Medical School, Director, Internal Medicine Residency Program, Beth Israel Deaconess Medical Center, Boston, United States
ABSTRACT
Facial recognition is an important aspect of human communication, facilitating the transfer of nuanced emotional information. While the ubiquitous adoption of face masks during the COVID-19 pandemic (2020 to 2023) was essential in the fight to curb viral transmission, there may have been unintended consequences for human interaction, including miscommunication and misinterpreted emotions. Although in 2025 there are no longer universal mask mandates in clinical and educational settings, it is an opportune time for teaching physicians to reflect on lessons learned and to strengthen their communication skills going forward. After all, masks are still required in certain clinical situations, and there may come another time when physicians are required, for the safety of their patients, their learners, and themselves, to don masks regularly. In this article, the authors review the basic neuroscience underpinning face processing and how this neural network can become disrupted, resulting in face blindness. They also discuss current evidence on how face masks might interfere with emotional state identification. Finally, the authors explore ways to enhance communication and avoid miscommunication within the medical team – whether masks are being worn, or not.
Key Words: communication, facial recognition, medical team, COVID-19
Email: Sam Woodworth (samuel.woodworth@mainehealth.org)
Date submitted: 1-April-2025
This is an open access journal, and articles are distributed under the terms of the Creative Commons Attribution-Non Commercial-Share Alike 4.0 License, which allows others to remix, tweak, and build upon the work non-commercially, as long as appropriate credit is given and the new creations are licensed under the identical terms.
Citation: Woodworth S and Smith C. Strategies to sustain emotional communication within the medical team in the presence of face masks. Educ Health 2025;38:284-287.
Online access: www.educationforhealthjournal.org
DOI: 10.62694/efh.2025.311
Published by The Network: Towards Unity for Health
As humans, we strive to make connections with those around us. Social development starts automatically at birth. A human newborn is limited to a visual distance of about 12 inches but responds immediately to facial stimuli and starts to prefer familiar faces.1,2 Throughout early childhood, there is constant learning and refinement of the skills needed to emote effectively and to understand the emotions of others. While we often turn to verbal communication in our relationships, the depth and breadth of non-verbal communication cannot be understated. The expansive emotional information encoded in our facial expressions is perhaps the most powerful means of non-verbal human communication. The ability to extract meaning from a face allows for the construction of complex, multidirectional connections to those around us. Undoubtedly, there is an innate, human interest in the recognition of a face.
During the early phases of the COVID-19 pandemic, mask-wearing became omnipresent. Many were obligated to push forward in work and life with 60–65% of their faces obscured. This was true for teaching physicians, who while working to reduce the spread of infection, sought to maintain high-quality care and to innovate curricula for learners. Although the benefits of mask-wearing are indisputable (i.e., preventing illness and saving the lives of innumerable patients/practitioners), it is worthwhile to consider some unintended, deleterious consequences for teaching physicians caused by wearing face masks during the COVID-19 pandemic. Such consequences include miscommunication, weakened communication, and devitalized emotional connections among members of the medical team.
A 2020 study evaluated the effect of surgical masks on emotional state recognition ability and demonstrated a clear performance drop when participants viewed masked faces.3 Another study from 2022 similarly found that facial coverings disrupted the interpretation of several emotional expressions (e.g., happiness, surprise, disgust, and fear).4 Unfortunately, such ambiguity in facial perception occurred throughout the pandemic at a time when emotional sensitivity and strengthened human connections were needed all the more. These findings should be of particular interest to teaching physicians given the need for clarity when communicating a wide range of emotionally complex information to patients, colleagues, and learners alike.
Now, more than five years after the first reports of COVID-19, hospital systems have long lifted mask mandates, a welcome decision symbolizing emergence from the pandemic. It is important to reflect upon lessons we learned from mask-wearing during the pandemic – and to look ahead. At some point in the not-too-distant future, for the safety of our patients, our learners, and ourselves, it seems likely that we will again need to don masks. In addition, at a time of heightened social stress with an imperative to communicate with clarity, the need for compassion and understanding is greater than ever.
As we started to remove our masks in response to decreasing COVID-19 cases, many working in health care shared the peculiar experience of seeing a coworker’s or learner’s entire face for the first time (often despite having worked together for an extended period and in uncertain, trying circumstances). For some, it may have been a moment of surprise, curiosity, or possibly dissonance; a sudden realization of how our brains had been working automatically to make masked faces complete. To unpack this experience, we can start by exploring the neurological underpinnings of human facial perception and how it can go awry. Reflecting on how masks might hinder one’s ability to process all of the information built into facial expressions, teaching physicians can become more mindful in those situations still requiring face masks (e.g., caring for patients on airborne or droplet precautions) and develop strategies to bolster emotional communication throughout the medical team.
So how do we process faces? What is it about the human brain that makes us react immediately and instinctively when presented with a face? Neuroscientists have employed a reductionist approach to study facial perception in a close relative to humans—the macaque monkey. Using both fMRI imaging and electrical recordings from individual neurons, researchers have delineated discrete anatomical areas of neurons in the brain dedicated to recognizing faces.5–7 The neurons of interest seem to be active only in response to complete representations of faces – they are quiescent when presented with a partial face or individual facial features. These specialized groups of neurons are known as Face Patches. In the human brain, analogous groups of neurons are present in the fusiform gyrus, located within the inferior, medial temporal lobe.8 There are likely significant social benefits to near-instantaneous face processing, hence the appearance of Face Patches in the evolution of the primate brain.
While the human brain is hardwired for facial perception, there can also be an inability to recognize faces, including one’s own (either congenitally or as the result of acquired injury to the fusiform gyrus). First described in 1947 by the German neurologist Joachim Bodamer, this condition is called prosopagnosia or face blindness.9 Prosopagnosia affects up to 2–3% of the human population10 and can lead to significant psychosocial hardship. An inability to recognize others can strain relationships and cause difficulties at school and later in the workplace. Prosopagnosia may engender conjectures of poor attention or memory loss, causing unnecessary stress and heightened anxiety/depression. Interestingly, neuropsychological deficits have been described in patients with Long COVID, including a case report of new onset prosopagnosia in a 28-year-old woman.11 There have also been discussions about whether the universal presence of face masks during the COVID-19 pandemic could have disrupted early childhood development of facial perception, leading to prosopagnosia in some children.12
Where do we go from here? First, we should all pause and take a look around the medical team, smiling. We should recognize and celebrate the wealth of non-verbal emotional information visible in the unmasked faces around us. This should also be a moment, however, to analyze and practice ways to enrich our communication beyond facial expressions. There remain certain clinical settings that will always require face masks. Furthermore, seasonal mask mandates may be necessary depending on the burden of respiratory virus transmission. So, now while we can, it will benefit us to reflect upon and practice how to create a safe learning environment, and best communicate with our patients, learners, and the multidisciplinary team.
There are steps that teaching physicians can take to avoid miscommunication within the medical team – whether or not face masks are being worn (see Table 1). Practicing multidimensional communication, we can work to improve patient care and medical education, both in the present moment and for the future times when we may need to don masks regularly again.
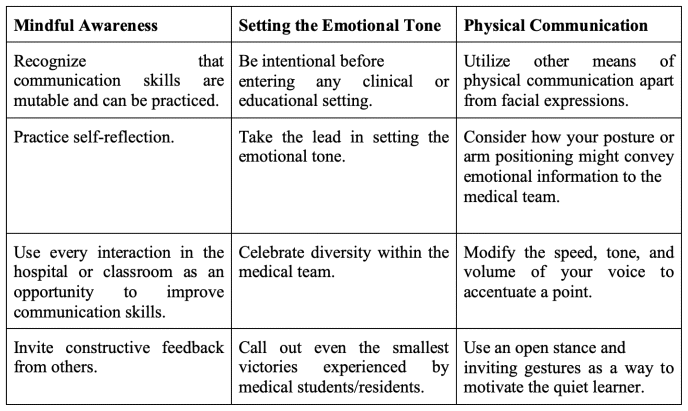
Table 1 Steps that teaching physicians can take to avoid miscommunication among members of the medical team – whether or not face masks are being worn
First of all, there must be an awareness that communication skills are mutable and can be practiced. This demands mindfulness and self-reflection. Teaching physicians should view each interaction with a patient, colleague, or learner as an opportunity to improve. Communication is multidirectional and thus multiple viewpoints should be considered when examining an individual encounter. Try reflecting on an especially difficult clinical or educational experience. How could you have made your point more clearly? Did you effectively listen? Additionally, it is important to invite constructive feedback as a way to improve your communication skills and build trust among team members.
Teaching physicians also need to take the lead in setting the emotional tone for the medical team. This requires thoughtful preparation prior to entering any clinical or educational setting. An energized team is more likely to approach the practice of medicine with excitement, nurturing a deeper sense of purpose. Teaching physicians should explicitly celebrate the diversity of backgrounds and perspectives of team members. The balance of expertise and experience should be regarded as a source of creativity. Try to call out and reward even seemingly small victories, which medical students and residents experience, day in and day out. It goes a long way to tell someone that you like what he or she did, and that it helped a patient.
Finally, teaching physicians should work to utilize other means of physical communication apart from facial expressions. Much can be gleaned from one’s posture or arm positioning (e.g., crossed, open and extended, akimbo). The speed, tone, and volume of one’s voice can be regulated to accentuate a point. Thoughtful, intentional eye contact and head nods ensure an understanding of great attention and care. Just think of the quiet learner – a welcoming wave or subtle opening of one’s stance can be inviting and serve to motivate someone who might otherwise feel too shy to participate. These other forms of body language can help to maintain an empathic and intriguing environment. They can also serve as a way to generate excitement. Showing true enthusiasm and passion for medicine and teaching can inspire others to adopt a similar approach.
Facial recognition helps to facilitate, ease, and enliven human communication – our brains are hardwired for it. Driven by necessity and safety concerns, masks became ubiquitous during the COVID-19 pandemic. Such face coverings, however, may lead to unintentional face blindness and prompt miscommunication or misinterpreted emotions. It is important for teaching physicians to recognize the innate power of facial perception and work to improve their communication skills. With a focus on self-reflection, energetic leadership, and multifaceted body language, they can create a shared emotional understanding among members of the medical team, and foster meaningful excitement about the practice of medicine.
1. Simion F, Leo I, Turati C, Valenza E, Dalla Barba B. How face specialization emerges in the first months of life. Progress in Brain Research. 2007;169–185. https://doi.org/10.1016/s0079-6123(07)64009-6
Crossref PubMed
2. Farzin F, Hou C, Norcia AM. Piecing it together: Infants’ neural responses to face and object structure. Journal of Vision. 2012;12(13):6–6. https://doi.org/10.1167/12.13.6
Crossref
3. Carbon CC. Wearing Face Masks Strongly Confuses Counterparts in Reading Emotions. Frontiers in Psychology. 2020 Sep 25;11(2526). https://doi.org/10.3389/fpsyg.2020.566886
Crossref PubMed PMC
4. Wong HK, Estudillo AJ. Face masks affect emotion categorisation, age estimation, recognition, and gender classification from faces. Cognitive Research: Principles and Implications. 2022 Oct 8;7(1). https://doi.org/10.1186/s41235-022-00438-x
PubMed PMC
5. Tsao DY, Schweers N, Moeller S, Freiwald WA. Patches of face-selective cortex in the macaque frontal lobe. Nature Neuroscience. 2008 Jul 11;11(8):877–879. https://doi.org/10.1038/nn.2158
Crossref PubMed PMC
6. Freiwald WA, Tsao DY, Livingstone MS. A face feature space in the macaque temporal lobe. Nature Neuroscience. 2009 Aug 9;12(9):1187–1196. https://doi.org/10.1038/nn.2363
Crossref PubMed PMC
7. Freiwald WA, Tsao DY. Functional Compartmentalization and Viewpoint Generalization Within the Macaque Face-Processing System. Science. 2010 Nov 4;330(6005):845–851. https://doi.org/10.1126/science.1194908
Crossref PubMed PMC
8. Kanwisher N, McDermott J, Chun MM. The Fusiform Face Area: A Module in Human Extrastriate Cortex Specialized for Face Perception. The Journal of Neuroscience. 1997 Jun 1;17(11):4302–4311. https://doi.org/10.1523/jneurosci.17-11-04302.1997
Crossref PubMed PMC
9. Bodamer J. Die prosop-agnosie. Archiv für Psychiatrie und Nervenkrankheiten Vereinigt mit Zeitschrift für die Gesamte Neurologie und Psychiatrie. 1947;179(1–2):6–53. https://doi.org/10.1007/bf00352849
10. Grüter T, Grüter M, Carbon CC. Neural and genetic foundations of face recognition and prosopagnosia. Journal of Neuropsychology. 2008 Mar;2(1):79–97. https://doi.org/10.1348/174866407x231001
Crossref
11. Kieseler ML, Duchaine B. Persistent prosopagnosia following COVID-19. Cortex: a Journal Devoted to the Study of the Nervous System and Behavior. 2023 May 1;162:56–64. https://doi.org/10.1016/j.cortex.2023.01.012
Crossref PubMed PMC
12. Joseph RA, Carter B. Prosopagnosia (face blindness) and child health during the COVID-19 pandemic. Nursing Children and Young People. 2023 Jul 6;35(4):28–34. https://doi.org/10.7748/ncyp.2023.e1454
Crossref
© Education for Health.
Education for Health | Volume 38, No. 3, July-September 2025