Helen Wu1, Biju Wang2, Petra Clark-Dufner3, Robin Pugh Yi4, and Bruce Gould5
1PhD, Associate Professor, Department of Psychiatry, Connecticut Convergence Institute for Translation in Regenerative Engineering, University of Connecticut Health Center, Farmington, United States
2PhD, Researcher, Connecticut Convergence Institute for Translation in Regenerative Engineering, University of Connecticut Health Center, Farmington, United States
3MA, Director, Urban Service Track/Area Health Education Center Scholars Program, University of Connecticut Health Center, Farmington, United States
4PhD, President, Akeso Consulting, Vienna, United States
5MD, Emeritus faculty and Founding Associate Dean of Primary Care; Founding Director, Connecticut Area Health Education Program, University of Connecticut Health Center, Farmington, United States
ABSTRACT
Background: Caregiver burden is associated with declines in physical, emotional, social, and financial functioning. Interprofessional teams of healthcare providers are optimally and uniquely positioned to implement critical steps toward reducing caregiver burden, and preventing and mitigating burnout: identifying informal caregivers, assessing their needs, and referring them to appropriate resources.
Objective: University of Connecticut Medical School Urban Service Track (UST) developed, implemented, and assessed a program to train interprofessional health professions students to understand caregiver burnout, assess informal caregivers for burnout, and refer caregivers to resources known to mitigate burden and burnout. The curriculum’s learning objectives were to train learners to: 1) identify the signs and symptoms of caregiver burden/burnout; 2) assess caregivers’ acute and long-term care needs; 3) refer caregivers to resources to address their specific needs; and 4) develop and offer a comprehensive care plan for caregivers.
Methods: UST developed case studies and guidelines and implemented training with 255 health professions students from Spring 2020 through Spring 2024. All trainees provided at least partial evaluation data.
Results: Assessment of knowledge change showed significant improvement in all targeted areas. Substantial proportions of participants reported intent to apply what they had learned to assess caregiver burden and burnout; share information for addressing these issues with patients, team members, and colleagues; and refer caregivers to resources that can mitigate burden and burnout.
Conclusions: Findings suggest that brief, low-cost, interprofessional training on how to assess and address informal caregiver burnout can be an effective approach to addressing this urgent, prevalent, and costly public health issue.
Key Words: informal caregiver burnout, assessing informal caregivers’ needs
Email: Helen Wu (ZWu@UCHC.edu)
Date submitted: 23-April-2025
This is an open access journal, and articles are distributed under the terms of the Creative Commons Attribution-Non Commercial-Share Alike 4.0 License, which allows others to remix, tweak, and build upon the work non-commercially, as long as appropriate credit is given and the new creations are licensed under the identical terms.
Citation: Wu H, Wang B, Clark-Dufner p, Pugh Yi R, and Gould B. Training clinicians to address caregiver burnout. Educ Health 2025;38:269-273.
Online access: www.educationforhealthjournal.org
DOI: 10.62694/efh.2025.334
Published by The Network: Towards Unity for Health
Approximately one in five American adults is an unpaid caregiver, providing one or more other people who have a long-term medical condition or disability1 with assistance for activities of daily living or medical tasks, making informal caregiving a critical source of long-term care. About 20 percent of caregivers report that their own health is less than good.2 Caregiver burden is associated with declines in physical, emotional, social, and financial functioning, including increased risk of anxiety and depression and potential decreases in work opportunities and income.1,2,3 Stress associated with caregiving can lead to caregiver burnout, which is defined as emotional exhaustion, detachment, and low sense of accomplishment or meaning associated with caregiving.1 In addition to damaging caregiver health, burnout may lead to adverse outcomes for those receiving care, such as premature nursing home placement and other poor health outcomes for patients.4 This urgent public health issue will become more critical as the population ages.1
Interventions such as respite care, referral to support services, educational training, and psychosocial interventions have successfully reduced burden and depression, and improved caregivers’ quality of life.5,6 Steps toward reducing caregiver burden include healthcare professionals’ identifying informal caregivers, assessing their needs, and referring them to appropriate resources.7 Health professionals who receive training in how to identify, assess, and refer informal caregivers have reported increased knowledge and value what they have learned.8 However, currently there are few resources to train health professions students and the healthcare workforce in these essential skills.7,9
UST developed, implemented, and assessed a training program that aims to prepare health professions students to:
The study aimed to assess whether training participants increased their knowledge about informal caregiver roles, tools for identifying signs and symptoms of caregiver burden and burnout, resources for caregiver support, and interprofessional care competencies. The study also assessed trainees’ intentions to apply what they had learned in clinical practice.
UST’s objectives were to train participants to work as a team to: 1) identify signs and symptoms of caregiver burden/burnout; 2) assess caregivers’ acute and long-term care needs; 3) refer caregivers to appropriate resources; and 4) develop and offer comprehensive caregiver care plans. Faculty developed five hypothetical case studies along with training guidelines. Training topics included: 1) the role and work of informal caregivers; 2) tools that offer evidence-based approaches for identifying symptoms of caregiver burnout; 3) resources to assist caregivers in addressing patient needs and their own burden; and 4) and IPEC core competencies.
Training was provided by a faculty member and a 3rd or 4th year health professions student coach. UST provided trainers with guidelines for time allocation, training goals, and questions tailored for the case study. Student coaches and faculty met prior to training to discuss the case and prepare the training session.
Each training session covered one case study. Two weeks prior to in-person training, students received a case description and assignments to complete. Assignments included viewing a video about addressing burnout among caregivers of people with dementia, reading information about caregiver burnout, reading information about safe prescription of opioids, reviewing instruments for assessing caregivers’ emotional, physical, and mental burden and needs, and visiting websites that offer resources for caregivers. These assignments took approximately an hour to 90 minutes, in total, to complete.
The one-day in-person training sessions lasted approximately three hours. For the first hour, students divided into groups of approximately 10 to discuss identifying caregivers, assessing caregiver burden and burnout, and how to work as a team to prevent and mitigate burnout, in addition to discussing a case study of caregiver burnout. Students discussed signs and symptoms illustrated by the case, how to address them, and which resources would address the caregiver’s needs. Following small group discussions, the full group convened. Small groups presented their care plans and received feedback from trainers and peers. Trainers emphasized the importance of offering interprofessional team-based care. The initial cohort comprised 14 trainees. Subsequent cohorts comprised between 40 and 61 trainees.
Because this training was part of the educational curriculum and no personal identifying information was collected with student evaluations, the University of Connecticut Institutional Review Board determined that the study was exempt from review.
Before and after training, trainees completed an online survey using 5-point Likert scales developed by UST faculty to rate trainees’ targeted areas of knowledge about caregiver burnout and resources available to support caregivers. Self ratings rather than cognitive assessments were used because self ratings indicate self-efficacy and motivation, in addition to perceived competence. Self ratings correlate strongly with external ratings in formative assessments in which raters share a learning purpose, as was the case with current training.10 Following training, participants completed an online survey to provide demographic information, area of discipline, year of training, and perceptions of the degree to which the training achieved learning objectives using 5-point Likert scales. The survey also included open-ended questions about how participants would apply what they had learned in clinical practice, how they would communicate with caregivers, and how training could be improved. Data were collected between Spring 2019 and Spring 2024.
Quantitative data were analyzed with SAS® software. Mantel-Haensen chi-square test was used to compare pre- and post-training ratings. The two-tailed significance threshold was p<0.05. Data analysts reviewed responses to open-ended survey questions to identify key points and themes.
Eligible participants included 255 health professions students who were in their 2nd through 4th years of training between 2019 and 2024. Participants were training for professions in medicine, pharmacy, physician assistant, dentistry, nursing, and social work. All eligible participants participated in training and provided at least some evaluation data (100% response rate).
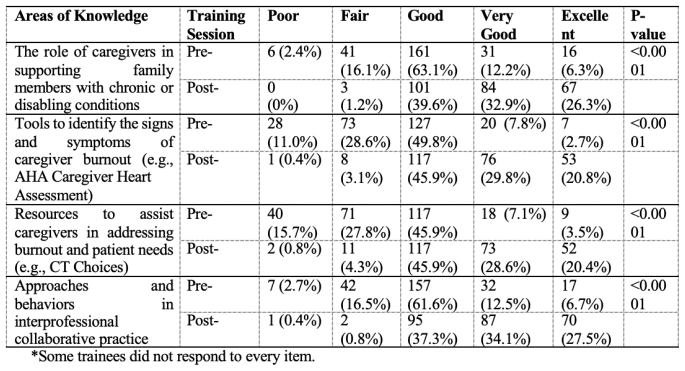
Table 1 summarizes trainees’ ratings of their knowledge of the four targeted topics before and after the training intervention. Chi-square tests indicate that perceived knowledge significantly improved in all targeted areas (p<0.01).
Table 1 Ratings of overall knowledge in caregiver burnout pre-/post-training (n=255*)
Table 2 summarizes trainees’ ratings of their knowledge about each of the five resources and tools discussed during training. Chi-square comparisons showed that perceived knowledge about all resources significantly improved (p<0.01). Following training, respondents indicated the degree to which they perceived that training had met its learning objectives. At least 90 percent of participants agreed or strongly agreed that training had met each of its objectives. The survey included open-ended questions about how participants would apply what they had learned in clinical practice and how training could be improved. Respondents reported that they intended to apply what they had learned in practice and would share information about caregiver support and resources with patients and their caregivers. They suggested that training include a broader range of case studies and more discussions about cases.
Table 2 Knowledge ratings of specific caretaker resources pre- and post-training.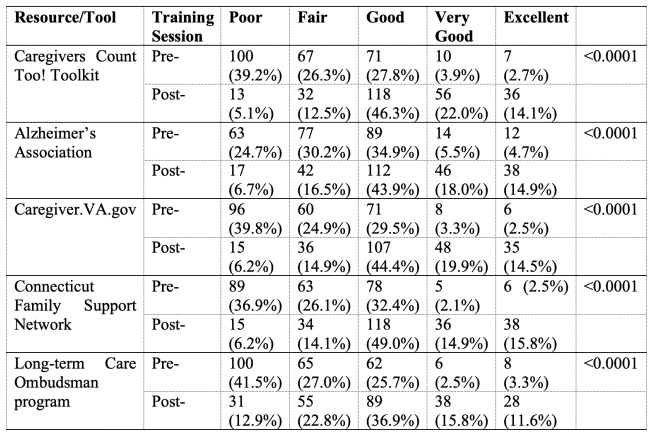
Previous research has identified a need for healthcare providers to understand the role of their patients’ who are informal caregivers, to be able to identify these caregivers, and to mitigate burden through care planning and use of support resources.1,3,5–9 Results indicate that the UST curriculum is a promising approach for addressing these training needs. Following training, students of multiple health professions expressed their intent to apply what they had learned in their practice to identifying caregivers, developing plans to mitigate caregiver burden and prevent burnout, and referring informal caregivers to resources for mitigating caregiver burden and burnout. As the population ages, the number of people with chronic diseases and disabilities will increase, along with the need for informal caregiver support. Primary care providers are uniquely poised to identify these caregivers and provide them with the resources they need.
The current study assessed the effects of training on knowledge and intent to implement lessons learned in practice. Future studies should assess the degree to which trainees identify, assess, and provide resources to caregivers in professional practice, and how these practices affect caregiver and patient outcomes. As training the healthcare workforce to identify and support informal caregivers becomes the norm, core competencies and curricula should be identified and standard measures to evaluate these competencies should be developed.
The UST curriculum is a promising approach to training primary care professionals from multiple disciplines to address this priority public health issue.
1. Gérain P, Zech E. Informal caregiver burnout? Development of a theoretical framework to understand the impact of caregiving. Frontiers in Psychology. 2019; 10: 1748. https://www.frontiersin.org/journals/psychology/articles/10.3389/fpsyg.2019.01748/full
Crossref PMC
2. Edwards VJ, Bouldin ED, Taylor, CA, Olivari BS, McGuire LC. Characteristics and health status of informal unpaid caregivers—44 states, District of Columbia, and Puerto Rico, 2015–2017. MMWR Morbidity and Mortality Weekly Report. 2020; 69: 183–188. https://pubmed.ncbi.nlm.nih.gov/32078592/
Crossref
3. Frederick D. Mitigating burden associated with informal caregiving. Journal of Patient Experience. 2018 Mar; 5(1):50–5. https://doi.org/10.1177/2374373517742499
Crossref PubMed PMC
4. Kaminishi KS, Safavi R, Hirsch CH. Caregiver burnout. In Geriatric Psychiatry, Hategan A, Bourgeois, J, Hirsch C, Giroux C. (Eds) 2018 Springer. (pp. 691–708). https://doi.org/10.1007/978-3-319-77128-1_19
Crossref
5. Czaja SJ, Lee CC, Perdomo D, Loewenstein D, Bravo M, Moxley, PhD JH, Schulz R. Community REACH: An implementation of an evidence-based caregiver program. Gerontologist; 2018 Mar 19;58(2): e130–7. https://doi.org/10.1093/geront/gny001
Crossref PubMed
6. Hughes S, Shuman SB, Wiener JM, Gould E. Research on supportive approaches for family and other caregivers. Research summit on dementia care: Building evidence for services and supports. 2017 Mar. https://aspe.hhs.gov/reports/research-supportive-approaches-family-other-caregivers-0
7. Blackie M, Baughman KR, Palmisano B, Sanders M, Sperling D, Scott E, Radwany S, Drost J, Thomas J. Building provider–caregiver partnerships: Curricula for medical students and residents. Academic Medicine. 2019 Oct 1; 94:10,1483–8. https://doi.org/10.1097/ACM.0000000000002806
Crossref PubMed
8. Yanamadala M, Kaprielian VS, Grochowski CO, Reed T, Heflin MT. A problem-based learning curriculum in geriatrics for medical students. Gerontology and Geriatrics Education, 2018; 39:2, 122–131, https://doi.org/10.1080/02701960.2016.1152268
Crossref
9. Parmar J, Anderson S, Duggleby W, Holroyd-Leduc J, Pollard C, Brémault-Phillips S. Developing person-centred care competencies for the healthcare workforce to support family caregivers: Caregiver centred care. Health and Social Care in the Community. 2021 Sep;29(5):1327–38. https://doi.org/10.1111/hsc.13173
Crossref
10. Andrade H. A critical review of research on student self-assessment. Educational Counseling Psychology Faculty Scholarship. 2019. 22. https://scholarsarchive.library.albany.edu/edpsych_fac_scholar/22
© Education for Health.
Education for Health | Volume 38, No. 3, July-September 2025