Siobhan Fitzpatrick1, Laura Magaña2, Jack Haywood3, Clare Kerswill4, Celine Tabche5, and Priscilla Robinson6
1MA, Health Workforce Department, World Health Organization, Geneva, Switzerland
2MSc, PhD, Association of Schools and Programs of Public Health, Washington DC, United States
3MFPH, MSc, MBBS, WHO Collaborating Centre for Human Resources for Health, NHS England, Manchester, United Kingdom
4WHO Collaborating Centre for Human Resources for Health, NHS England, Manchester, United Kingdom
5FHEA, PhDc, MSc, ANtr, WHO Collaborating Centre for Public Health Education and Training, School of Public Health, Imperial College London, London, United Kingdom
6PhD, MPH, MHSc(PHP), World Federation of Public Health Associations, Geneva; LaTrobe University, Victoria, Australia
ABSTRACT
Background: Competency-based education has variable uptake in public health, despite calls for effective education-to-employment pathways. A WHO and partners’ Roadmap to strengthen the public health and emergency workforce called for a holistic globally-relevant competency-based framework oriented to practice and delivery of the Essential Public Health Functions (EPHFs). This research answers the question: What are the relevant competencies and practice activities for the breadth of the public health workforce to deliver the 12 globally-relevant EPHFs? Methods: A mixed methods approach was used to build the competency framework, informed by literature review; content analysis of existing frameworks and curricula using the WHO competency model as an organizing framework; and an iterative approach to drafting, consultation and consensus about the framework content. Results: Twenty competencies were identified as relevant to the public health workforce across contexts, geographies and role responsibilities, organized into six domains: community-centeredness; decision-making; communication; collaboration; evidence-informed practice; and personal conduct. Forty practice activities that describe the work required to deliver the EPHFs are organized into five domains: health systems enablers; public health intelligence; public health programs and services; management of resources for public health programs and services; and public health emergency management. Discussion: Whilst the 20 competencies unite the public health workforce, irrespective of occupational group, public health priority or context, practice activities are role-specific and require contextualization. Competencies and practice activities must be interpreted together to provide a holistic approach to competence.
The value of the framework is in its contextualization and application. Different components of the framework provide a common language but can be adapted to inform education and employment. Reflections on the methodology and the framework construct and organization are offered, confirming the WHO competency model application as a lens to interpret content from multiple sources to provide clarity about learning and assessment of educational content.
Key Words: competency-based education, competency framework, essential public health functions, public health, emergencies, workforce, competencies, practice activities, World Health Organization
Date submitted: 1-May-2025
Email:Siobhan Fitzpatrick (fitzpatricks@who.int)
This is an open access journal, and articles are distributed under the terms of the Creative Commons Attribution-Non Commercial-Share Alike 4.0 License, which allows others to remix, tweak, and build upon the work non-commercially, as long as appropriate credit is given and the new creations are licensed under the identical terms.
Citation: Fitzpatrick S, Magaña L, Haywood J, Kerswill C, Tabche C, and Robinson P. Development of the World Health Organization Global competency and outcomes framework for the Essential Public Health Functions. Educ Health 2025;38:91-102
Online access: www.educationforhealthjournal.org
DOI: 10.62694/efh.2025.341
Published by The Network: Towards Unity for Health
Effective education-to-employment pathways align education and workforce systems so that learners can experience a seamless transition between learning in formal education programs and functioning in the workplace. The Lancet Commission,1,2 the World Health Organization (WHO)3 and others call for competency-based education (CBE) that is rooted in health and health system needs, but note that progress towards implementation is variable. CBE is an outcomes-oriented approach that de-emphasizes time in learning,4 and shifts the focus from knowledge to mastery of skills and competencies5 relevant to employment upon course completion.
This alignment is variable for the public health workforce. Graduates of specialist academic public health programs go into a range of professions, and many public health sector employees lack a public health background.6–8 Often, academic public health programs provide a broad knowledge base that opens many pathways but does not offer a direct vocational route, and in contrast public health content is often omitted from other programs.9–11
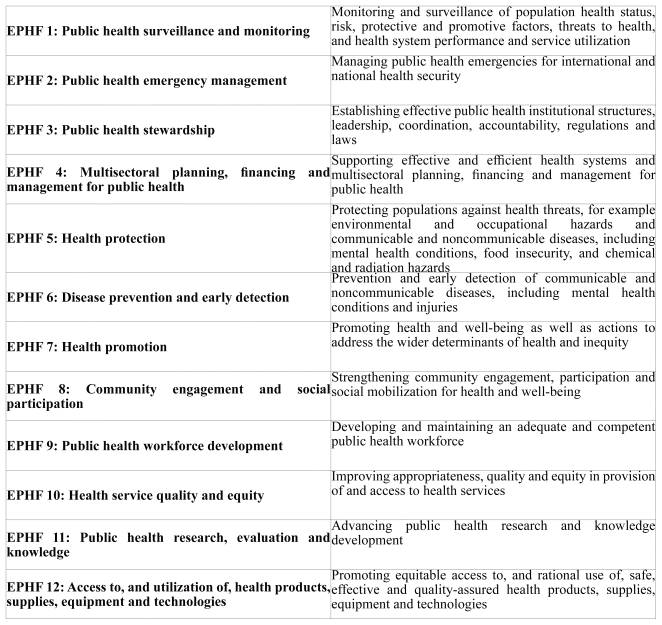
In 2022, the WHO and partner organizations launched a roadmap to strengthen the public health and emergency workforce.12 Underpinning these efforts is the WHO revised set of 12 globally-relevant EPHFs (Table 1).13 The development of a Global competency and outcomes framework for the Essential Public Health Functions (EPHFs) (hereafter, “the Framework”) is therefore a response to the call from the 70+ partner organizations of the Roadmap to strengthen CBE approaches oriented to developing the skills and competencies for employment to deliver the EPHFs.
Table 1 The 12 WHO Global Essential Public Health Functions (adapted from (13))
The public health workforce includes all individuals who contribute to at least one of the EPHFs as part of integrated services and systems. This workforce comprises people who can be conceptually framed in three overlapping groups: core public health personnel, health and care workers, and occupations allied to health. Collaborative intersectoral efforts by a range of occupations are required to achieve the interrelated functions. Often, efforts to strengthen education approaches for these occupational groups are fragmented. This Framework represents the first effort to identify in a holistic common framework the competencies and education outcomes required for public health practice, irrespective of occupational title or geographical context.
The WHO, through previous normative work to strengthen CBE,14 has adopted a common conceptual model that offers a holistic approach to competence (the proficiency of the individual to perform expected job tasks) and intentionally differentiates between the components of competence: the practice activities (core functions of health practice encompassing groups of related tasks), the competencies (the integration and application of knowledge, skills and attitudes in their performance of tasks, demonstrated through behaviors), and the foundational knowledge, skills and attitudes (Figure 1).

Figure 1 WHO competency model.14
The research answers the question: What are the relevant competencies and practice activities for the breadth of the public health workforce to deliver the 12 globally-relevant EPHFs?
Following Batt et al’s six-step approach to competency framework development in health,15 the Roadmap Steering Committee determined the purpose (a reference set of competencies and education outcomes to align education with employment and public health needs), scope (the 12 EPHFs), resources (research team from WHO, Imperial College London and NHS England) and the timeline. The components of the Framework were guided by the research question and the WHO competency model.
The selected methodologies follow common practice to incorporate a combination of literature review and expert consensus, with data derived from content analysis of frameworks identified through a systematic literature review. An iterative and integrative approach to drafting and development was followed incorporating expert consultation and consensus.
A literature review was undertaken to identify existing frameworks and curricula. Details of the literature review including the search terms, inclusion and exclusion criteria, the Preferred Reporting Items for Systematic Review (PRISMA) flow diagram and the final set of 57 included studies are previously published.16 Hand searching of reference lists and an open call for resources identified a further 69 frameworks meeting the inclusion criteria, with a final total of 126.
A global Technical Advisory Group (TAG) was established to advise on the methodological approach, to provide advice on drafting and development, and to recommend best practice to strengthen the utility of the Framework.17 Twenty-three members were appointed in an individual capacity with consideration given to gender, geographical and professional balance.
A further 119 peer reviewers were identified through the Roadmap Steering Committee, the WHO Global Health Workforce Network Education Hub, WHO country and regional offices and headquarters, and the network of WHO Collaborating Centres. Most individuals reviewed three drafts of the Framework. Ten individuals were invited to advise on the conceptualization of the Framework as well as its contents, as Principal peer reviewers. The characteristics of experts are provided in Table 2.
Table 2 Characteristics of TAG members, Principal peer reviewers and peer reviewers (adapted from Annex 3 (16))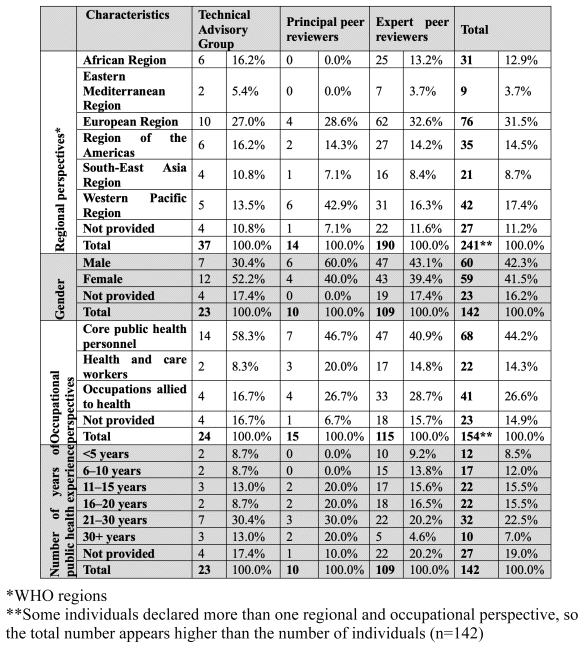
A process of deconstructing the content of the 126 identified frameworks and curricula was followed for the purpose of thematic analysis using the 12 EPHFs as a framing. The WHO competency model was used as a lens to deconstruct statements according to their characteristics: functional (tasks, practice activities); behavioral (competencies, behaviors); knowledge; and other content (attitudes, values, impact statements, goals). A common data extraction template was used, and data were (re)grouped throughout the process.
The competency domains from the WHO (2022) Global Competency and Outcomes Framework for Universal Health Coverage14 were used as a starting point, recognizing that these were informed by analysis of more than 300 competency frameworks relating to health and care workers, inclusive of population health practice activities. The domains, scope and set of practice activities and competencies evolved through the process of iterative drafting and thematic analysis of content from existing competency frameworks.
Content analysis of 31 prioritized frameworks informed the first full draft of the Framework together with a mapping of the EPHF subfunctions and advice from the TAG on the preliminary findings of the research. The frameworks were selected by the Roadmap Steering Committee and TAG based on their influence and impact, the scope breadth, and recent publication date. Content analysis data was shared with experts for review and validation.
Content analysis of the remaining 95 frameworks was used to validate the content, framing and terminology. Peer reviewers also identified grey literature that were synthesized and translated into content for the Framework, particularly where feedback highlighted gaps or omissions.
Iterative Framework drafting enabled integrating insights from the content analysis of existing frameworks, and feedback from review and consultation. With each review, one component of the Framework was validated and the subsequent part reviewed for the first time.
Experts were requested to prioritize their review of specific domains according to their area of expertise. Feedback was invited through tracked changes and comments. Incorporating inputs and arbitration of dissent was handled by the lead author together with the TAG Co-Chairs. With each draft, reviewers were provided with a summary of feedback received, changes made in response to feedback, or a rationale why a change was not made as well as tracked changes or a mapping of high-level changes, for their review and response.
More than 8,500 individual comments and suggestions were offered throughout the Framework development, in addition to 30 letters or perspectives. By the third full draft, there was consensus on the content and organization of content within the Framework. Table 3 provides a timeline summary of the development of the framework.
Table 3 Methodology and timeline for the development of the Framework
The data in this study include secondary sources and professional comments. In compliance with the Declarations of Helsinki, approval from an Ethics Committee was not required. Sixteen declarations of conflict of interests and confidentiality agreements were reviewed by the WHO Secretariat; none were deemed to present a true conflict of interest. No individual or entity received payment for participation.
Forty practice activities necessary for the delivery of the EPHFs were identified, each comprising a range of 6–19 tasks (cumulatively, 507 tasks). The practice activities for the EPHFs are role-specific. Some individuals will have responsibilities across multiple areas and others will have responsibilities in just one area.
The 40 practice activities are organized into five domains as shown in Figure 2:
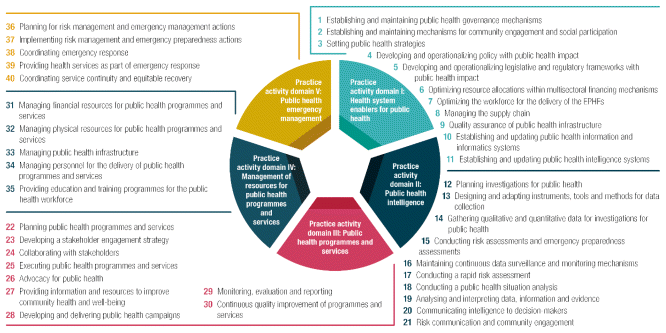
Figure 2 Practice activities for the Essential Public Health Functions, adapted from (16)
Each practice activity is mapped to the relevant EPHFs and their subfunctions. The delivery of each EPHF requires multiple practice activities: each EPHF subfunction requires between 17 and 39 practice activities to deliver. Similarly, each practice activity is relevant to the delivery of between 9 and all 48 of the EPHF subfunctions. For example, practice activities at the systems level relating to governance, policy and strategy underpin the delivery of every EPHF, whereas others are narrower.
Acknowledging that the practice activities are high level and focus on what someone does rather than who should do it, the need for additional guidance to contextualize the content became clear. Illustrative profiles for core public health personnel, health and care workers, occupations allied to health—as well as senior specialists (from any of the three groups) and policy authorities—are provided for each practice activity. Further, each practice activity is accompanied by a curricular guide, identifying the key fields of knowledge that underpin the performance of tasks for the practice activity.
Twenty competencies were identified for the delivery of the practice activities for the EPHFs, each demonstrated through between 3–7 behaviors each (cumulatively, 103 behaviors). Whereas practice activities are role-specific and offer a menu of different education outcomes, the full set of 20 competencies was found to be relevant to all practice activities.
The 20 competencies are organized into six domains as shown in Figure 3:

Figure 3 Competencies for the Essential Public Health Functions, adapted from (16)
The competencies for delivery of the EPHFs unite the public health workforce and are essential for the effective performance of public health across occupational groups, geographies and public health priorities. The different behaviors that demonstrate each competency differ according to the context – namely the practice activity, role responsibility, public health priority, and geography (including language and culture). For example, all the public health workforce needs to communicate actively and attentively (competency 8), but this will differ according to whether the individual is involved in risk communication, policy development or health promotion education.
Competencies feature predominantly on individual development in the education literature.
By contrast, the practice activities are role-specific, although, depending on the context, most practice activities could be primarily led by any occupational group. No individual can single-handedly deliver any of them, just as no individual can provide any single EPHF so, for employers, the Framework offers a menu of different practice activities that might be part of an individual’s role responsibilities, adapted to specific jurisdictional contexts. Practice activities are commonly used in the employment literature to describe task lists, job descriptions and occupational responsibilities (for example,18,19)
The Framework is rooted in the principles of CBE, with an intentional differentiation between the practice activities for public health practice, and the competencies of the individuals who provide them. The importance of interpreting the practice activities and competencies together, forming a holistic approach to competence, cannot be overstated. Public health is not simply following a task list, but the integration of competencies to navigate the complexities of the context. As such, the competencies enable the performance of practice activities, forming the performance-based standard (or passing standard) for competence.
When contextualizing the Framework to inform education outcomes, or for employment or workforce planning, all the competencies are used, and the practice activities (and tasks and curricular guides) must be contextualized. Figure 4 further illustrates how the different components of the Framework can be applied to education and employment.
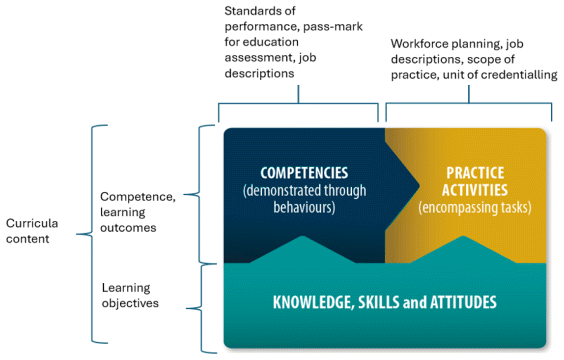
Figure 4 The application of the different components of the Global Competency and Outcomes Framework for the EPHFs, adapted from (14, 16)
The Framework is accompanied by guidance to adapt to standards (authoritative statements) or frameworks (menus of content for contextualization), as well as to inform curricula redesign. The Framework must be contextualized to the role responsibilities, environmental and social context including the available tools, resources and teams, as well as public health priorities. This approach to educational design is equally relevant to employment as to pre-service, in-service and specialization education programs.
The implementation of CBE across public health generally requires a culture shift from academic groundings in public health, to programs oriented to job responsibilities. Transitioning to fully CBE programs may occur incrementally. It requires resources, trained faculty, supervised practical experience and pathways from formal education programs to decent employment that values the learned skills and competencies. Implementation of the principles of CBE requires deliberate and concerted intersectoral effort across health, education and employment, together with regulatory bodies.
The mixed methods approach enabled the triangulation of existing literature and public health practice insights through the expert consultation. The goal was not to create an “average” of existing frameworks but to synthesize and organize content using the WHO competency model aligned with the 12 EPHFs. The free text comments provided valuable feedback for iterative drafting.
Existing frameworks use a range of conceptual approaches to identify ‘competencies’, often using the term as synonymous with all education outcomes. Further, many frameworks included content that would not be categorized as an education outcome, for example encompassing impact statements (e.g. improves the fairness of the system) or system rather than individual responsibilities (e.g. mobilizes emergency resources). The research also identified many duplications and overlapping content within frameworks; for example, by including the word ‘effectively’ in some statements but not others, the implication is that only certain statements need to be conducted ‘effectively’. Using the WHO competency model enabled analysis of content statements according to characteristics (behavioral, functional, knowledge or other), and improved clarity in writing and presentation of content.
Some existing publications that were used to inform the drafting of the Framework used levels or other differentiators between different groups of content. In our analysis, we identified different axes including supervision level; task complexity; context predictability; and task impact. These levels are related exclusively to the practice activity, and not to the competencies. We also identified some levels relating to the learning journey, however, some frameworks blurred boundaries; for example, listing knowledge as a first level, a task/practice activity second, and then a top-level stated policy development about that task (a distinct practice activity). In our construction of this Framework, we opted not to develop levels, acknowledging the different learning journeys and pathways to complexity, impact, and autonomy that are part of contextualization.
The final Framework is high-level, principles-based, and at the same time, detailed. The specificity of practice activities and tasks linked with public health priorities could be exponential. Thus, through this research, practice activities and tasks were organized according to their high-level summary task and practice activities in general terms. This requires further contextualization to elaborate the range of specific programs, services and priority EPHFs. Users looking for specific public health priorities or terms such as “climate change”, “antimicrobial resistance” or “pandemic preparedness” may not find the content they relate to straight away, as it requires contextualization.. Dissemination efforts should focus on implementation approaches and the Framework’s relevance across occupational groups.
The systematic literature review and subsequent consultation was conducted in English only, thereby omitting any resources or insights that may have been available in other languages. Efforts to mitigate the impact of this limitation included specific outreach to involve experts from a range of countries and contexts.
The search terms for the systematic review identified less than half of the competency frameworks that were subsequently included in the development of the Framework. A broader set of search terms could be defined from the EPHFs, as well as different public health priorities. Many existing frameworks and curricula are found in grey literature, and so our final search included both systematic review of the published peer-reviewed literature and the grey literature. Although we cannot claim that every competency framework relevant to the field of public health was identified, we are confident we identified more frameworks than other similar research. This helped mitigate any unintended bias introduced through the selective inclusion or omission of existing works.
The WHO Global competency and outcomes framework for the EPHFs16 unites the education outcomes and employment roles for an otherwise fragmented and increasingly specialized public health workforce into a comprehensive competency-based framework. The Framework provides guidance, and a reference set of competencies and education outcomes, for aligning education with employment and public health needs to build and maintain the workforce required to deliver the EPHFs to meet public and population health needs. Further, through the focus on practice activities it highlights the intersectoral and interprofessional approaches needed to deliver the EPHFs.
The Framework provides a common language between education and employment and can be used to guide the design of education programs oriented to public health employment that deliver EPHFs, as well as the job requirements for public health.
The methodology adopted in this Framework confirmed the utility of the WHO conceptual model as a lens through which to interpret content from multiple other sources irrespective of language or terminology. Further, it confirms that the differentiation between practice activities (that describe work tasks), competencies (of the individual) and knowledge, skills and attitudes (component learning objectives) matters, because they are learned differently, assessed differently, and demonstrated differently in practice.
The value of the Framework is in its contextualization and application. Implementation and uptake of CBE requires deliberate and concerted effort across actors and sectors as part of efforts to strengthen the public health workforce capacity. Workforce planners and educators of the public health and emergency workforce are encouraged to use the Framework16 to orient the workforce to meet public and population health needs.
1. Frenk J, Chen L, Bhutta ZA, Cohen J, Crisp N, Evans T, Fineberg H, Garcia P, Ke Y, Kelley P, Kistnasamy B, Meleis A, Naylor D, Pablos-Mendez A, Reddy S, Scrimshaw S, Sepulveda J, Serwadda D, Zurayk H. Health professionals for a new century: transforming education to strengthen health systems in an interdependent world. Lancet. 2010 Dec 4;376(9756):1923–1958. https://doi.org/10.1016/S0140-6736(10)61854-5
Crossref PubMed
2. Frenk J, Chen LC, Chandran L, Groff EOH, King R, Meleis A, Fineberg HV. Challenges and opportunities for educating health professionals after the COVID-19 pandemic. Lancet. 2022;400(10362):1539–1556. https://doi.org/10.1016/S0140-6736(22)02092-X
Crossref PubMed PMC
3. World Health Organization. Global Strategy for Human Resources for Health: 2030. Geneva: World Health Organization; 2016. Retrieved 30 April 2025 from https://www.who.int/publications/i/item/9789241511131
4. Frank JR, Mungroo R, Ahmad Y, Wang M, De Rossi S, Horsley T. Toward a definition of competency-based education in medicine: a systematic review of published definitions. Medical Teacher. 2010;32(8):631–637. https://doi.org/10.3109/0142159X.2010.500898
Crossref PubMed
5. Frank JR, Snell LS, Cate OT, Holmboe ES, Carraccio C, Swing SR, Harris P, Glasgow NJ, Campbell C, Dath D, Harden RM, Iobst W, Long DM, Mungroo R, Richardson DL, Sherbino J, Silver I, Taber S, Talbot M, Harris KA. Competency-based medical education: theory to practice. Medical Teacher. 2010;32(8):638–645. https://doi.org/10.3109/0142159X.2010.501190
Crossref PubMed
6. Hare Bork R, Robins M, Schaffer K, Leider JP, Castrucci BC. Workplace perceptions and experiences related to COVID-19 response efforts among public health workers—public health workforce interests and needs survey, United States, September 2021–January 2022. MMWR Morbidity and Mortality Weekly Report. 2022;71(29):920–924. https://doi.org/10.15585/mmwr.mm7129a3
Crossref PubMed PMC
7. Leider JP, Harper E, Bharthapudi K, Castrucci BC. Educational attainment of the public health workforce and its implications for workforce development. Journal of Public Health Management and Practice. 2015;21 Suppl 6(Suppl 6):S56–68. https://www.jstor.org/stable/48517197
Crossref PubMed PMC
8. Frank MW, Weihofen A, Schmucki MD, Nocera S, Paccaud F. Public health workforce in Switzerland: a national census. Zurich: Foundation Swiss School of Public Healthplus; 2013. Retrieved 30 April 2025 from https://ssphplus.ch/assets/downloads/publications/public-health-february-2013b.pdf
9. Watts RD, Bowles DC, Fisher C, Li IW. What do public health graduates do and where do they go? An analysis of job destinations and mismatch in Australian public health graduates. International Journal of Environmental Research and Public Health. 2021;18(14). https://doi.org/10.3390/ijerph18147504
Crossref PubMed PMC
10. Magaña L, Biberman D. Training the next generation of public health professionals. American Journal of Public Health. 2022;112(4):579–581. https://doi.org/10.2105/AJPH.2022.306756
Crossref PubMed PMC
11. Thibault GE. The future of health professions education: Emerging trends in the United States. FASEB Bioadvances. 2020;2(12):685–694. https://doi.org/10.1096/fba.2020-00061
Crossref PubMed PMC
12. World Health Organization. National workforce capacity to implement the essential public health functions including a focus on emergency preparedness and response: roadmap for aligning WHO and partner contributions. Geneva: World Health Organization; 2022. Retrieved 30 April 2025 from https://www.who.int/publications/i/item/9789240060364
13. World Health Organization. Defining essential public health functions and services to strengthen national workforce capacity. Geneva: World Health Organization; 2024. Retrieved 30 April 2025 from https://www.who.int/publications/i/item/978924009143614.
14. World Health Organization. Global Competency and Outcomes Framework for Universal Health Coverage. Geneva: World Health Organization; 2022. Retrieved 30 April 2025 from https://www.who.int/publications/i/item/9789240034662
15. Batt AM, Tavares W, Williams B. The development of competency frameworks in healthcare professions: a scoping review. Advances in Health Sciences Education Theory and Practice. 2020;25(4):913–987. https://doi.org/10.1007/s10459-019-09946-w
Crossref
16. World Health Organization. Global competency and outcomes framework for the Essential Public Health Functions. Geneva: World Health Organization; 2024. Retrieved 30 April 2025 from https://www.who.int/publications/i/item/9789240091214
17. World Health Organization. Call for expressions of interest: Technical Advisory Group on education for public health and emergency workforce roadmap 2022. Retrieved 30 April 2025 from https://www.who.int/news-room/articles-detail/call-for-expressions-of-interest--technical-advisory-group-on-education-for-public-health-and-emergency-workforce-roadmap.
18. International Labour Organization. The International Standard Classification of Occupations- ISCO-08. Geneva: International Labour Organization; 2008. Retrieved 30 April 2025 from https://isco.ilo.org/en/isco-08/
19. World Health Orgnaization. Workload Indicators of Staffing Need (WISN) User Manual, 2nd edition. Geneva: World Health Organization; 2023. Retrieved 30 April 2025 from https://www.who.int/publications/i/item/9789240070066
© Education for Health.
Education for Health | Volume 38, No. 2, April-June 2025