Brooke E Schroeder1, Jessie Li-Barton2, Jennifer Howell3, Melody Baldwin4, Jordan Schaumberg5, Tracey Reynolds6, Sarah Wright7, Poonam Sharma8, and Sarah K Dotters-Katz9
1BS, Medical Student, Duke University School of Medicine, Durham, United States
2MD, Resident physician, Department of Obstetrics and Gynecology, Duke University Medical Center, Durham, United States
3MD, Professor, Department of Obstetrics and Gynecology, Duke University Medical Center, Durham, United States
4MD, MPH, Assistant Professor, Department of Obstetrics and Gynecology, Duke University Medical Center, Durham, United States
5MD, Assistant Professor, Department of Obstetrics and Gynecology, Duke University Medical Center, Durham, United States
6BA, PIONEER Program Coordinator, Duke University School of Medicine, Durham, United States
7BA, Undergraduate Medical Education Program Coordinator, Duke University Medical Center, Durham, United States
8MD, Associate Professor, Department of Medicine, Duke University Medical Center, Durham, United States
9MD, MMHPE, Professor, Department of Obstetrics and Gynecology, Duke University Medical Center, Durham, United States
ABSTRACT
Background: Longitudinal and amalgamative clerkship models enhance medical education through faculty continuity, mentorship, and targeted feedback. A United States allopathic medical school piloted a 16-week longitudinal clerkship (PIONEER), including one half-day of obstetrics and gynecology (OB/GYN) clinic per week. This study assessed the impact of preceptor continuity on student knowledge and procedural experience during the OB/GYN portion of PIONEER.
Methods: This cross-sectional study (August 2023–July 2024) surveyed PIONEER students on OB/ GYN knowledge, procedural experience, and preceptor continuity. Students were categorized into “high” or “low” continuity experiences based on Likert responses. Outcomes included changes in knowledge and procedural exposure, with secondary analyses comparing procedural opportunities across the academic year and to the OB/GYN traditional block clerkship.
Results: Among 83 respondents (76.1% response rate), 71.1% reported low continuity with OB/GYN preceptors. Knowledge and procedural experience did not differ between continuity groups (all p>0.05). PIONEER students’ procedural opportunities remained consistent across the year and exceeded those of traditional clerkship students (e.g., 25.7-fold increase in students performing >10 breast exams; 1.6-fold increase for pelvic exams).
Discussion: These exploratory findings suggest that meaningful educational experiences can occur in OB/GYN amalgamative longitudinal clerkships even with variable preceptor continuity. Importantly, PIONEER preserved a core benefit of longitudinal models—greater procedural exposure—while highlighting the need for future research to more comprehensively evaluate the contributions of preceptor, patient, and location continuity to student learning.
Key Words: clinical education, obstetrics and gynecology, longitudinal integrated clerkship
Date submitted: 8-June-2025
Email: Brooke E Schroeder (brooke.schroeder@duke.edu)
This is an open access journal, and articles are distributed under the terms of the Creative Commons Attribution-Non Commercial-Share Alike 4.0 License, which allows others to remix, tweak, and build upon the work non-commercially, as long as appropriate credit is given and the new creations are licensed under the identical terms.
Citation: Schroeder B, Li-Barton J, Howell J, Baldwin M, Schaumberg J, Reynolds T, Wright S, Sharma P, and Dotters-Katz S. Effect of longitudinal clerkship model and preceptor continuity on student learning and skills in obstetrics and gynecology. Educ Health 2025;38:311-320
Online access: www.educationforhealthjournal.org
DOI: 10.62694/efh.2025.368
Published by The Network: Towards Unity for Health
Longitudinal integrated clerkship (LIC) models and their adaptations, such as amalgamative clerkships, enhance medical student education by promoting stronger faculty mentorship, clinical autonomy, and efficacy in patient-centered care compared to traditional clerkship models.1–5 These benefits have been largely attributed to the continuity with preceptors and clinical space, which allow for more personalized teaching and feedback, as well as integration into clinic workflow.6–10 There also appear to be educational advantages, as students in longitudinal clerkships have demonstrated comparable or superior performance on standardized shelf and board examinations.11 Beyond academic and clinical gains, longitudinal clerkships have been shown to influence students’ career choices, particularly by increasing interest in primary care and rural medicine—fields facing ongoing workforce shortages.11–13 Historically, these longitudinal programs have focused on specialties such as family medicine, pediatrics, and internal medicine. Although Ford et al. included obstetrics and gynecology (OB/GYN) in its longitudinal model, the study did not examine OB/GYN-specific learning or procedural experience.12 Similarly, Beattie et al., based in Australia, noted that general practice obstetrics was an option within their longitudinal clerkship, but only described increased interest in the field, rather than detailing OB/GYN-specific educational outcomes.13
Despite their success in primary care and rural medicine, the effect of longitudinal clerkship models remains underexplored in OB/GYN. Continuity-based clinical experiences in OB/GYN may provide additional opportunities for procedural experience, as preceptors gain more confidence with student capabilities.14 Like in primary care, longitudinal OB/GYN clerkships may improve clinical education, increase student satisfaction, and influence specialty choice.15,16 However, longitudinal preceptorship in OB/GYN presents challenges due to the varied schedules of OB/GYN clinicians, who divide their time between clinic, the operating room, and labor and delivery (including overnight call), and may not be able to precept a student at the same time each week. These barriers highlight the need to examine how different longitudinal clerkship structures function when integrating specialties like OB/GYN.
There have been multiple frameworks proposed for classifying longitudinal clerkships and their adaptations. One widely cited typology by Worley and colleagues outlines three main types:17 First, comprehensive LICs, the most common in the literature, are year-long experiences in which students are paired with specific preceptors and follow a patient panel across settings; these models maximize continuity but are resource-intensive and challenging to implement at scale. Secondly, blended or hybrid LICs combine traditional block rotations with longitudinal experiences for a majority of the year, offering breadth and flexibility but typically reduced continuity.18 Finally, amalgamative clerkships, by contrast, integrate multiple specialties and occupy less than half of the academic year, making them more feasible for institutions but often providing weaker longitudinal relationships. Within these adaptations, continuity may occur at the level of patients, teachers, or location. Continuity-of-location models—where students rotate in the same clinical environment but with different preceptors—have been described as a “stabilizing factor” for learners.19 However, some argue that without sustained student-preceptor relationships, such models may be neither fully integrated nor longitudinal, and it is unclear whether these models can replicate the benefits of more traditional, comprehensive LICs.
This study investigates this question in the context of OB/GYN, a specialty with scheduling challenges, by examining whether continuity-of-location models can still yield meaningful longitudinal and educational benefits. It evaluates how student-perceived preceptor continuity within an amalgamative longitudinal OB/GYN clerkship shapes student learning and procedural experience. Despite the growing interest in longitudinal clerkship models, there is a paucity of literature on how preceptor continuity affects learning experiences in OB/GYN. This study had two aims: (1) to evaluate whether student-perceived preceptor continuity influenced knowledge and procedural experience in an amalgamative OB/GYN clerkship; and (2) to compare student procedural experiences across trimesters and with the traditional OB/GYN clerkship model. In doing so, we seek to better understand how continuity models can be adapted to meet the challenges of OB/GYN education, while preserving the established benefits of comprehensive LICs.
During the 2023–2024 academic year, a United States allopathic medical school introduced PIONEER, a 16-week outpatient amalgamative clerkship model. Because it spans multiple specialties yet occupies less than half of the academic year, the model fits what the literature describes as an “amalgamative clerkship,” an LIC-inspired approach that lengthens each rotation beyond the usual block.17 This structure was selected to ensure every student could participate within a single academic year (one-third of the class rotated in each trimester). Students spent one half-day each week in OB/GYN clinic while simultaneously engaging in several other outpatient disciplines over the full 16 weeks.
Medical students still completed a four-week inpatient OB/GYN clerkship separately from the outpatient portion. After Institutional Review Board (IRB) approval and exemption (Pro00111517), this cross-sectional study was conducted from August 2023 to July 2024 to evaluate students’ OB/GYN outpatient experiences during the first year of the PIONEER curriculum. Participants were asked to complete a voluntary, anonymous survey, and students were informed that responses would be kept confidential and would not affect their grades or clerkship evaluations. The study sample included all medical students who participated in the 16-week PIONEER outpatient OB/GYN clerkship during the 2023–2024 academic year and completed the end-of-course survey. The study population therefore represents students enrolled in the PIONEER curriculum at our institution, while the target population includes medical students participating in longitudinal or amalgamative OB/ GYN clerkships more broadly, for whom these findings may provide preliminary insights.
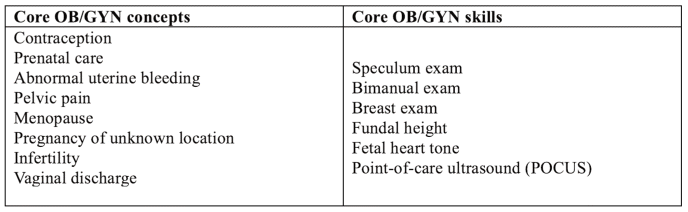
A 13-item e-survey was developed to assess comfort with OB/GYN-specific topics and common office procedures, as well as perceived preceptor continuity (concepts and skills evaluated are summarized in Table 1). The survey was piloted for clarity and reviewed by subject matter experts. Then, all clerkship students were asked to complete the anonymous 13-item e-survey at the end of their PIONEER clerkship, with two reminder emails. The change in skill comfort and knowledge was defined as the difference between Likert-scale responses, using a retrospective pre/post survey design. Students were also asked to estimate how many procedures they personally observed and how many they performed (defined as “hands-on”) during their 16-week PIONEER block. Total procedural participation was defined as the number of observed plus “hands-on” procedures.
Table 1 Core OB/GYN concepts and skills. Metrics assessed in the end-of-clerkship survey administered to longitudinal clerkship students, based on APGO Medical Student Educational Objectives. Students rated their comfort with each concept or skill before and after PIONEER on a scale from 1 (Extremely uncomfortable) to 5 (Extremely comfortable).
For the primary aim of the study, students were divided into “high continuity” and “low continuity” OB/GYN experiences based on predefined response groupings to distinguish differences in perceived preceptor consistency. Given the lack of established thresholds in the literature, these groupings were determined based on face validity, with responses reflecting the student’s perception of consistent preceptor exposure classified as “high continuity” (e.g. “I had good continuity, AND it was better than other specialties”) and those indicating limited continuity classified as “low continuity” (e.g. “I did not have good continuity in OB/GYN”). This approach allowed for a practical comparison of student experiences within the continuity-of-location model.
For the secondary aim, we examined whether the timing of PIONEER within the academic year influenced observed and hands-on procedural experiences. We also compared students’ observed and hands-on procedural experiences in PIONEER to those of traditional clerkship students from the prior academic year (2022–2023). For the former clerkship model, the data was collected from an end of the clerkship feedback survey (100% response rate), which asked students to report their estimated number of procedures in a categorical fashion (none, 1–5, 6–10, >10).
Data were analyzed using descriptive statistics and bivariate analyses (Mann-Whitney U tests for pairwise comparisons, Kruskal-Wallis tests for multi-group comparisons, and Fisher’s exact test for categorical comparisons), chosen due to the non-parametric nature of the data. Statistical significance was set at p<0.05. Analyses were conducted using Python 3.12.7 with relevant libraries (e.g., SciPy, Pandas).
In total, 89 of 109 (81.6%) medical students responded to the survey, with response rates of 80.5% (n = 29/36, 1st), 81.1% (n = 30/37, 2nd), and 66.7% (n = 24/36, 3rd) per trimester. Of these students, six were missing responses (by trimester: n=2 from 1st, n=1 from 2nd, and n=3 from 3rd) about perceived continuity and were excluded (total included n = 83). Nearly three-quarters of students (n = 59/83, 71.1%) reported that they perceived a lack of continuity with their OB/GYN preceptors.
All skills and knowledge improved over the rotation for both groups (Table 2). The only significant difference in student comfort between groups was for menopause-related concepts (p=0.01). No significant differences were observed in other knowledge areas or comfort with procedures (Table 2). Additionally, the differences in OB/GYN conceptual knowledge and procedural comfort between the two groups are unlikely to be educationally significant, as all group means remained within one Likert scale point of each other.
Table 2 Change in knowledge and comfort for OB/GYN concepts and skills based on studentperceived preceptor continuity. Measure is the difference between Likert scale* pre- and post-PIONEER (values expressed as means (+/− standard deviations))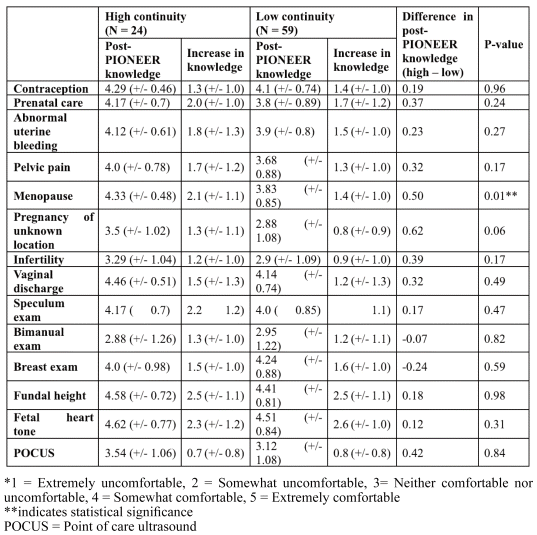
For procedural experience, students in the high continuity group tended to perform more fetal heart tone assessments compared to the low continuity group (16 vs. 13, p=0.05). No other statistically significant differences were found in the number of procedures students observed, performed, or participated in, based on perceived preceptor continuity (Table 3). While students in the high continuity group performed more procedures on average for most skills (n = 15/24, 62.5%), these differences were not statistically significant and are unlikely to be of educational importance, with the largest difference being five fetal heart tone assessments (Table 3).
Table 3 Number of observed and performed procedures based on student-perceived preceptor continuity (values expressed as means (rounded to the nearest whole number) (+/− standard deviations))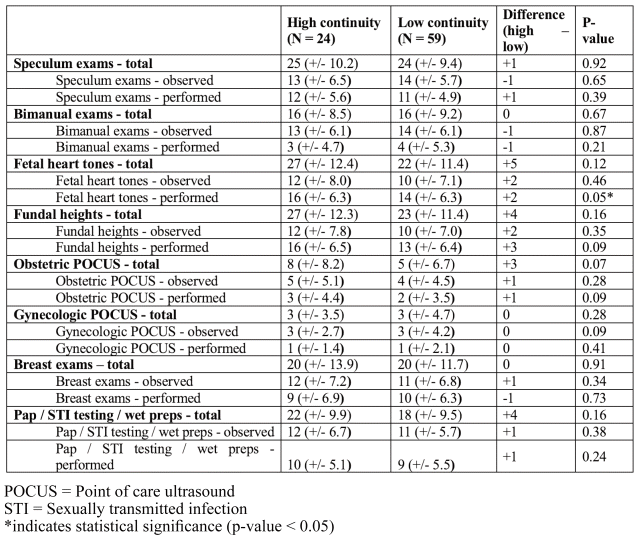
Across trimesters, students observed an average of 14 pelvic exams, 14 bimanual exams, 11 breast exams, 10 fetal heart tones, and 11 fundal heights. Additionally, they reported performing 11 pelvic exams, 4 bimanual exams, 9 breast exams, and 14 fetal heart tones/fundal heights. The only statistically significant difference across trimesters was for observed and performed gynecologic point of care ultrasound, with the third trimester reporting the least (Table 4). However, students rarely had the opportunity to observe (mean 2.79, range 0–20) or perform (mean 0.82, range 0–10) these procedures, with high variability in opportunity. Otherwise, there was no significant difference in procedural opportunities based on which trimester the student rotated in (all p>0.05).
Table 4 Number of observed and performed procedures compared across trimesters (values expressed as means (rounded to the nearest whole number) (+/− standard deviations))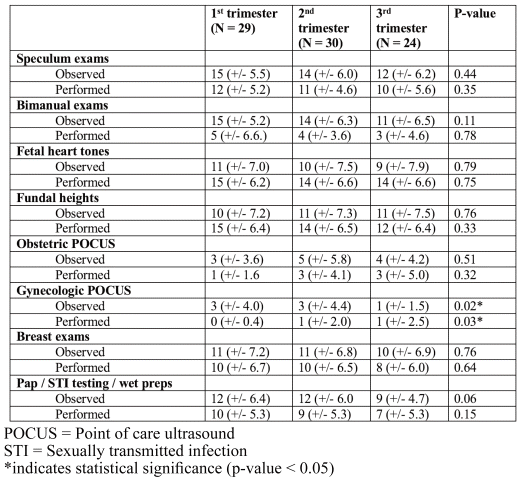
Because PIONEER students also completed the standard 4-week inpatient OB/GYN block, the analyses below isolate only the procedures they logged during their weekly outpatient PIONEER sessions and compare them with the total (inpatient + outpatient) procedures reported by students in the traditional clerkship. This framing highlights the increased outpatient experience provided by the PIONEER model while acknowledging that differences in reporting periods temper the strength of conclusions.
PIONEER outpatient time alone yielded significantly higher numbers of breast exams than the traditional clerkship (p<0.01, Table 5). In 2022–23, 39.8% (n = 43/108) of traditional clerkship students reported not performing any breast examinations, while only 1.8% (n = 2/108) performed 10 or more. In contrast, among PIONEER students, only 3.8% (n = 3/80) had no opportunity to perform a breast exam, and nearly half (n = 37/80, 46.2%) performed 10 or more.
Table 5 Number of observed and performed procedures compared to traditional clerkship model (values expressed as N (%))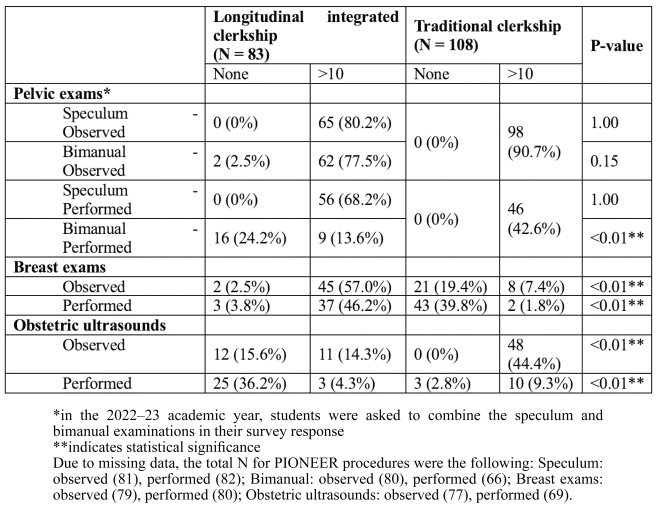
Pelvic examinations in 2022–23 were assessed using a combined estimate of speculum and bimanual exams, limiting direct statistical comparisons. In the traditional model, 42.6% (n = 46/108) of students reported performing greater than 10 pelvic examinations (either speculum or bimanual). Among PIONEER students, 68.2% (n = 56/82) performed more than 10 speculum exams. However, PIONEER students reported far less experience with bimanual exams, with just 13.6% performing more than 10 exams (n = 9/66).
When considering outpatient PIONEER encounters alone, students logged fewer obstetric ultrasounds than peers in the traditional clerkship’s full curriculum (p < 0.01, Table 5). Additional details are provided in Table 5.
Longitudinal integrated clerkships have been shown to enhance student clinical experience, increase standardized test scores, and influence career choices.1,11–13 However, preceptor continuity, a presumed contributor to these benefits, can be difficult to maintain in OB/GYN, particularly in clinical schedules that rely on fixed rotation days. Our study examines an amalgamative clerkship model in OB/GYN—inspired by LIC principles but not a traditional LIC—and compares student educational experiences and procedural opportunities based on student-perceived continuity with preceptors. We found no significant differences in student knowledge or procedural experience based on perceived preceptor continuity. However, these results are limited in power by the low number of students with high perceived preceptor continuity. PIONEER students reported significantly greater experience with breast examinations compared to those in the traditional clerkship model, and more PIONEER students reported performing greater than 10 speculum examinations. In contrast, traditional clerkship students performed a higher volume of obstetric ultrasounds, likely reflecting differences in clinic placement and access to ultrasound-heavy settings such as labor and delivery. This suggests that procedural opportunities for students may vary not only by curriculum structure but also by clinical site characteristics and the types of patients encountered.
Our findings provide new insight into the implications of differential preceptor continuity within an LIC-type model. A large majority of students in our cohort reported perceiving “low continuity” with their OB/GYN preceptors, suggesting that a model emphasizing continuity of location (e.g., the same clinical placement at the same time each week) may not effectively facilitate preceptor consistency with OB/GYN generalists’ varied schedules. Despite this, we found no significant differences in student educational growth or procedural opportunities based on preceptor continuity, a novel finding that, to our knowledge, has not been previously explored.
PIONEER students logged more procedures than peers in the traditional 4-week clerkship, reflecting an established advantage of longitudinal clerkships: extended exposure over time allows for greater hands-on experience and familiarity with clinic workflow. Most existing literature on longitudinal integrated clerkship (LIC) models highlights the benefits of increased clinical autonomy compared to traditional block rotations—a trend supported by our findings—even though prior studies have rarely addressed OB/GYN specifically.20–22 Beyond autonomy, our results also align with previous work showing that longitudinal OB/GYN clerkships provide students with greater procedural exposure than traditional models.14 This finding suggests that the benefits commonly associated with comprehensive LICs, such as increased procedural engagement, can be preserved in a shorter, amalgamative clerkship model.
Additionally, while patient continuity was not assessed in our study, our findings suggest that other features of continuity—such as becoming familiar with clinic workflow and forming relationships with the broader care team—may explain why students still experienced educational benefits within a continuity-of-location model, even without consistent preceptor pairings.19 This represents an important consideration for the design of longitudinal clinical curricula for specialties such as OB/GYN, where physicians frequently divide their time across multiple settings—outpatient clinic, labor and delivery, and the operating room. In contrast to family and internal medicine, where LICs are often designed around fixed clinic days, OB/GYN schedules are less predictable, complicating efforts to achieve sustained preceptor continuity. Yet, these preliminary findings suggest that longitudinal placements may still provide meaningful learning experiences.
Our data also demonstrate that procedural experience and autonomy did not vary based on trimester of the academic year, despite the fact students are expected to have more clinical experience and efficiency as the year continues.23 This contrasts with prior literature that have suggested student hands-on experience increase during mid- and late-year clerkship rotations.24, 25 However, these studies primarily focused on traditional block OB/GYN clerkships, whereas ours examines a longitudinal outpatient model and its associated procedures. This suggests that either the lower-acuity outpatient setting, the longitudinal structure, or a combination of both may help mitigate the seasonal differences in student procedural experience observed in block rotations.
This study is subject to several limitations that warrant consideration. First, as a single-center study, the generalizability of our findings to other academic clinical settings may be limited. Second, the small sample size of the high-continuity group and lower response rate of the third trimester students limits statistical comparisons. Additionally, the measure of “perceived continuity” relied on students’ subjective impressions rather than a documented count of how many times they worked with the same preceptor, making it an imprecise metric. The lack of a clear definition for “performed” and “observed” procedures may have introduced variability in the data collection process, potentially affecting the accuracy and consistency of these results. Because PIONEER does not meet the strict definition of an LIC (e.g., consistent preceptor-patient continuity across the year), our findings may be more applicable to amalgamative clerkship structures rather than classic LICs. Lastly, we were unable to examine the effect of continuity on other proposed benefits of longitudinal clerkships such as preceptor recommendation letters, exam scores, and patient-centered care, which should be explored in future research.
In summary, this study describes educational outcomes from an amalgamative clerkship model in OB/GYN and provides exploratory insight into how perceived preceptor continuity shapes student learning. While many of the findings were expected—such as greater procedural exposure with more outpatient time—our results also suggest that meaningful clinical learning and procedural experience can occur in an amalgamative structure even when preceptor continuity is inconsistent, underscoring the results that other factors such as clinic workflow familiarity and longitudinal patient exposure may also contribute to student growth.
Because this was a single-institution study with limited power, the findings should be interpreted as a foundation for future work. Nonetheless, the PIONEER model illustrates how amalgamative clerkships can still provide benefits similar to traditional LIC models, despite challenges achieving high continuity with preceptors. Importantly, these results provide a basis for multi-institutional studies to more rigorously evaluate the educational value of amalgamative clerkship models and to guide the extension of longitudinal clerkship models in OB/GYN.
1. Bell SK, Krupat E, Fazio SB, Roberts DH, Schwartzstein RM. Longitudinal pedagogy: a successful response to the fragmentation of the third-year medical student clerkship experience. Academic Medicine. 2008; 83(5): 467–475. https://doi.org/10.1097/ACM.0b013e31816bdad5
Crossref PubMed
2. Teherani A, Irby DM, Loeser H. Outcomes of different clerkship models: longitudinal integrated, hybrid, and block. Academic Medicine. 2013; 88(1): 35–43. https://doi.org/10.1097/ACM.0b013e318276ca9b
Crossref
3. Walters L, Greenhill J, Richards J, Ward H, Campbell N, Ash J, Schuwirth LW. Outcomes of longitudinal integrated clinical placements for students, clinicians and society. Medical Education. 2012; 46(11): 1028–1041. https://doi.org/10.1111/j.1365-2923.2012.04331.x
Crossref PubMed
4. Gaufberg E, Hirsh D, Krupat E, Ogur B, Pelletier S, Reiff D, Bor D. Into the future: patient-centredness endures in longitudinal integrated clerkship graduates. Medical Education. 2014; 48(6): 572–582. https://doi.org/10.1111/medu.12413
Crossref PubMed
5. Ogur B, Hirsh D. Learning through longitudinal patient care-narratives from the Harvard Medical School-Cambridge Integrated Clerkship. Academic Medicine. 2009; 84(7): 844–850. https://doi.org/10.1097/ACM.0b013e3181a85793
Crossref PubMed
6. Hirsh DA, Ogur B, Thibault GE, Cox M. “Continuity” as an organizing principle for clinical education reform. New England Journal of Medicine. 2007; 356(8): 858–866. https://doi.org/10.1056/NEJMsb061660
Crossref PubMed
7. Poncelet A, Bokser S, Calton B, Hauer KE, Kirsch H, Jones T, Lai CJ, Mazotti L, Shore W, Teherani A, Tong L, Wamsley M, Robertson P. Development of a longitudinal integrated clerkship at an academic medical center. Medical Education Online. 2011; 16(https://doi.org/10.3402/meo.v16i0.5939
Crossref PubMed PMC
8. Mazotti L, O’Brien B, Tong L, Hauer KE. Perceptions of evaluation in longitudinal versus traditional clerkships. Medical Education. 2011; 45(5): 464–470. https://doi.org/10.1111/j.1365-2923.2010.03904.x
Crossref PubMed
9. Bates J, Konkin J, Suddards C, Dobson S, Pratt D. Student perceptions of assessment and feedback in longitudinal integrated clerkships. Medical Education. 2013; 47(4): 362–374. https://doi.org/10.1111/medu.12087
Crossref PubMed
10. Snow SC, Gong J, Adams JE. Faculty experience and engagement in a longitudinal integrated clerkship. Medical Teacher. 2017; 39(5): 527–534. https://doi.org/10.1080/0142159x.2017.1297528
Crossref PubMed
11. Latessa R, Beaty N, Royal K, Colvin G, Pathman DE, Heck J. Academic outcomes of a community-based longitudinal integrated clerkships program. Medical Teacher. 2015; 37(9): 862–867. https://doi.org/10.3109/0142159x.2015.1009020
Crossref PubMed
12. Ford CD, Patel PG, Sierpina VS, Wolffarth MW, Rowen JL. Longitudinal Continuity Learning Experiences and Primary Care Career Interest: Outcomes from an Innovative Medical School Curriculum. Journal of General Internal Medicine. 2018; 33(10): 1817–1821. https://doi.org/10.1007/s11606-018-4600-x
Crossref PubMed PMC
13. Beattie J, Binder M, Beks H, Fuller L. Influence of a rural Longitudinal Integrated Clerkship on medical graduates’ geographic and specialty decisions: a constructivist grounded theory study. BMC Medical Education. 2024; 24(1): 795. https://doi.org/10.1186/s12909-024-05793-5
Crossref
14. Melo J, Kaneshiro B, Kellett L, Hiraoka M. The impact of a longitudinal curriculum on medical student obstetrics and gynecology clinical training. Hawai’i Journal of Medicine Public Health. 2014; 73(5): 144–147
15. Frattarelli LC, Kamemoto LE. Obstetrics and gynecology medical student outcomes: longitudinal multispecialty clerkship versus traditional block rotations. American Journal of Obstetrics and Gynecology. 2004; 191(5): 1800–1804. https://doi.org/10.1016/j.ajog.2004.07.066
Crossref PubMed
16. Davidson A, Shore E, Shirreff L, Shah A, Shah R. Validating an Obstetrics and Gynaecology Longitudinal Integrated Clerkship Curriculum at the University of Toronto: A Four-Year Review. Journal of Obstetrics and Gynaecology Canada. 2021; 43(3): 372–375. https://doi.org/10.1016/j.jogc.2020.06.020
Crossref
17. Worley P, Couper I, Strasser R, Graves L, Cummings BA, Woodman R, Stagg P, Hirsh D. A typology of longitudinal integrated clerkships. Medical Education. 2016; 50(9): 922–932. https://doi.org/10.1111/medu.13084
Crossref PubMed
18. Teherani A, Irby DM, Loeser H. Outcomes of different clerkship models: longitudinal integrated, hybrid, and block. Academic Medicine. 2013; 88(1): 35–43. https://doi.org/10.1097/ACM.0b013e318276ca9b
Crossref
19. Ellaway RH, Graves L, Cummings BA. Dimensions of integration, continuity and longitudinality in clinical clerkships. Medical Education. 2016; 50(9): 912–921. https://doi.org/10.1111/medu.13038
Crossref PubMed
20. Hauer KE, O’Brien BC, Hansen LA, Hirsh D, Ma IH, Ogur B, Poncelet AN, Alexander EK, Teherani A. More is better: students describe successful and unsuccessful experiences with teachers differently in brief and longitudinal relationships. Academic Medicine. 2012; 87(10): 1389–1396. https://doi.org/10.1097/ACM.0b013e31826743c3
Crossref PubMed
21. Bonnie LHA, Cremers GR, Nasori M, Kramer AWM, van Dijk N. Longitudinal training models for entrusting students with independent patient care?: A systematic review. Medical Education. 2022; 56(2): 159–169. https://doi.org/10.1111/medu.14607
Crossref
22. Mylopoulos M, Kulasegaram KM, Weyman K, Bernstein S, Martimianakis MAT. Same but Different: Exploring Mechanisms of Learning in a Longitudinal Integrated Clerkship. Academic Medicine. 2020; 95(3): 411–416. https://doi.org/10.1097/acm.0000000000002960
Crossref
23. Doyle C, Wilkerson L, Wimmers PF. Clinical clerkship timing revisited: Support for non-uniform sequencing. Medical Teacher. 2013; 35(7): 586–590. https://doi.org/10.3109/0142159x.2013.778393
Crossref PubMed
24. Schneider KM, Landen DA, Monga M. Seasonal variation in medical student experience in an obstetrics and gynecology clerkship. American Journal of Obstetrics and Gynecology. 2008; 198(5): e25–27. https://doi.org/10.1016/j.ajog.2007.09.048
Crossref PubMed
25. Lambert K, Engle D, Baldwin M, Temming L, Dotters-Katz SK. Timing of the obstetrics and gynecology clerkship and “hands-on” participation in deliveries. American Journal of Obstetrics Gynecology MFM. 2024; 6(12): 101527. https://doi.org/10.1016/j.ajogmf.2024.101527
Crossref
© Education for Health.
Education for Health | Volume 38, No. 4, October-December 2025