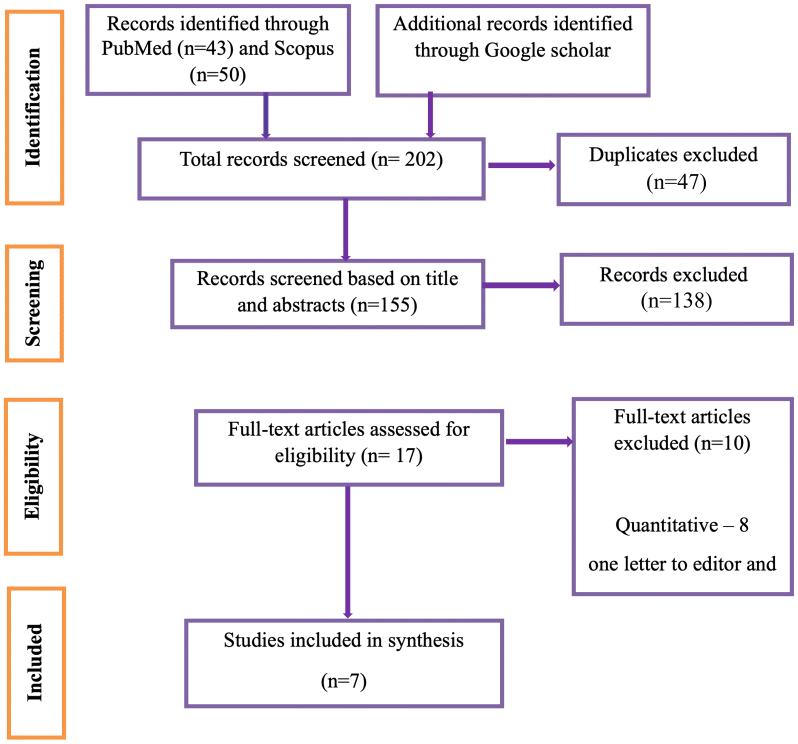
Figure 1 PRISMA flowchart to demonstrate the flow of search resulting in the inclusion of related articles
Amol Dongre1, Pradeep Deshmukh2, and Himanshu Pandya3
1MD (Comm Med), MPS, MHPE, Professor of Community Medicine, Sri Manakula Vinayagar Medical College and Hospital, Pondicherry, India
2MD (Comm Med), Professor and Head, Department of Community Medicine, All India Institute of Medical Sciences, Nagpur, India
3MD, Former Dean, Professor of Medicine and Medical Education, Pramukhswami Medical College, Bhaikaka University, Anand, India
ABSTRACT
Background: Since the implementation of Competency-Based Medical Education (CBME) for undergraduate medical education in India, stakeholders have expressed diverse perspectives. While many appreciated its structured framework and emphasis on competency development, others voiced concerns about implementation challenges, assessment strategies, and overall institutional readiness.
Objective: The present qualitative meta-synthesis explored the converging and diverging factors influencing the implementation of CBME.
Methods: Using a systematic search strategy, we selected seven qualitative and mixed-methods studies published between 2019 and 2025 from PubMed, Scopus, and Google Scholar. The integration of qualitative findings across studies was guided by Critical Interpretative Synthesis. A total of 130 descriptive codes were developed and categorized under six curricular components: competencies, curriculum content, teaching-learning methods, assessment, curriculum governance, and student support and faculty development.
Results: Key challenges included difficulties in framing competency objectives, overlapping content in foundation courses, limited faculty training in self-directed learning and assessments, inadequate support for simulation-based teaching, and misalignment between student priorities and curricular goals. Notable enablers included small-group teaching, simulation-based sessions, well-organized timetables, motivated faculty, and constructive student engagement. However, systemic issues such as infrastructure constraints, inadequate staff, their training in new methodologies, and poor interdepartmental coordination hindered full-scale implementation.
Conclusion: The study explored the collective dissonance experienced by stakeholders across various curricular components. Effective implementation of CBME would require committed faculty, adaptive leadership, and a context-sensitive regulatory framework that enables innovation and local relevance. This synthesis offers insights for educators, curriculum planners, and policymakers to refine CBME design and foster improvements in medical education in India.
Key Words: Curriculum, Competency based Medical Education, Undergraduate, India
Date submitted: 10-June-2025
Email: Amol Dongre (cm.amol@smvmch.ac.in)
This is an open access journal, and articles are distributed under the terms of the Creative Commons Attribution-Non Commercial-Share Alike 4.0 License, which allows others to remix, tweak, and build upon the work non-commercially, as long as appropriate credit is given and the new creations are licensed under the identical terms.
Citation: Dongre A, Deshmukh P, and Pandya H. Converging and diverging factors for CBME curriculum for Indian medical graduates: insights from a qualitative meta-synthesis. Educ Health 2025;38:367-379
Online access: www.educationforhealthjournal.org
DOI: 10.62694/efh.2025.372
Published by The Network: Towards Unity for Health
In 2019, the erstwhile Medical Council of India (MCI) introduced the Competency-Based Medical Education (CBME) curriculum to ensure that medical graduates acquire essential competencies through a structured, outcome-based approach rather than the traditional medical education system. The traditional curriculum in India was focused on knowledge acquisition with compartmentalization of disciplines.1 In contrast, new CBME curriculum shifted the focus to competencies such as clinical skills, communication, professionalism, leadership and teamwork, lifelong learning, critical thinking and research skills.2 While building on principles from the 1997 regulations,3 CBME introduced an outcome-driven model aligned with global trends. It emphasizes both horizontal and vertical integration while preserving subject-based instruction.4,5 This transformation strengthened curricular governance, with enhanced roles for Curriculum Committees, Medical Education Units, supported by the National Faculty Development Programme. All medical colleges regulated by the medical regulator in India, both private and government, except Institutions of National Importance (INIs) across the country are mandated to implement the new CBME curriculum.6
Following its implementation for undergraduate medical education in India, stakeholders expressed a range of perspectives. Some welcomed CBME’s structured approach,7 justified its rationale in the Indian context;8 while others raised concerns on factors influencing medical education in India and institutional preparedness.9 Several published reactions highlight these diverse viewpoints, underscoring the need for continuous evaluation and adaptation. As the CBME curriculum continues to be implemented, it is important to understand and manage stakeholder experiences and challenges to improve its acceptance and effectiveness.
Qualitative meta-synthesis is a systematic method for synthesizing findings from multiple qualitative studies to generate comprehensive and collective insights into complex phenomena.10 Unlike individual qualitative studies, qualitative meta-synthesis aggregates diverse perspectives, offering a broader understanding of recurring patterns, contradictions, and contextual nuances. In complex tasks like curriculum reform, where institutional differences make standard evaluations difficult, meta-synthesis helps identify the factors that facilitate or hinder its adoption. By integrating findings from various studies, it builds shared understanding of cross-cutting problems, explores interpretive variations, and offers directions to faculty development programmes, and institutional readiness. This approach is particularly valuable in resource-constrained settings, where large-scale formative quantitative evaluations are often unfeasible due to logistical and financial constraints.
The purpose of the present qualitative meta-synthesis was to collate the converging and diverging factors reported during the implementation of various curricular components within the CBME framework for medical undergraduates in India.
We referred to Preferred Reporting Items for Systematic Reviews and Meta-Analysis (PRISMA) for evidence-based reporting. As the present meta-synthesis was based on qualitative data from educational research, it was not eligible for registration in the Prospective Register of Systematic Reviews. We have preregistered it to Open Science Framework (OSF) Registries.11 We used Nested Knowledge platform, which is a comprehensive software platform designed to manage the systematic review and meta-analysis process.12 The steps followed in qualitative meta-synthesis are described below.
Given the purpose of the study, nature of studies included and the type of data, we decided to use a combination of the Kirkpatrick framework13 and Critical Interpretative Synthesis (CIS).14 Collating contextual findings from qualitative studies that employed varied approaches for a common purpose posed a significant challenge, requiring careful abstraction to ensure methodological coherence across diverse frameworks. To address the complexity of the topic, we used CIS as a guiding framework to systematically integrate qualitative findings across studies. While CIS is conventionally employed for theory generation, we adopted a pragmatic application of this approach to support the structured aggregation and interpretation of findings relevant to our context. Within CIS, three strategies employed were: 1) Reciprocal Translational Analysis (RTA); 2) Refutational Synthesis; and 3) Line of Argument (LOA) synthesis. RTA helped us identify shared themes. Refutational synthesis allowed us to examine and make sense of contradictory findings. LOA synthesis then brought together these diverse insights to generate general interpretations that reflect the breadth and complexity of the evidence. This approach enabled a comprehensive, context-sensitive synthesis that aligns with our purpose of informing practice rather than generating a theory.
We included all primary studies that utilized qualitative and mixed methods research on the Competency-Based Medical Education (CBME) curriculum for undergraduate medical education in India. To ensure comprehensive coverage, we employed a broad search strategy, prioritizing sensitivity to avoid missing potential studies. The search strategy for Google Scholar and Scopus was:
CBME AND undergraduate AND curriculum AND India. For PubMed it was: (((("cbme"[All Fields]) AND ("undergraduate"[All Fields])) AND ("curriculum"[All Fields])) AND ("india"[All Fields])).
We searched electronic databases such as Medline and Scopus for published articles from 2019 to 2025. Additionally, we conducted searches on Google Scholar, reviewing all articles appearing within the first 15 pages of search results.
In initial mapping, we obtained a total of 202 articles. After removing 47 duplicates, we screened the titles and abstracts of the remaining 155 articles. We excluded 138 articles from the initial screening as they were not relevant to the study’s purpose. We then assessed the full text of 17 articles and excluded 10 primary studies based on the following inclusion criteria: Original qualitative and mixed-methods research related to the CBME curriculum for medical undergraduates, published between 2019 and 2025. Articles included must have used qualitative research designs and presented rich interpretative data in the form of descriptions of themes or illustrative quotes from the participants. Ten articles were excluded for the following reasons: eight were quantitative studies, one was a letter to the editor, and one was not relevant to the topic. The process of selecting articles for the study followed the Preferred Reporting Items for Systematic Reviews and Meta-Analyses (PRISMA) flow diagram shown below (Figure 1). We then assessed the full text of all seven selected articles15–21 to identify the parts of primary studies that relate to the purpose of the meta-synthesis. The background details of the selected studies and their code contribution are given in Table 1.

Figure 1 PRISMA flowchart to demonstrate the flow of search resulting in the inclusion of related articles
Table 1 Details of articles used in the qualitative meta-synthesis and their code contribution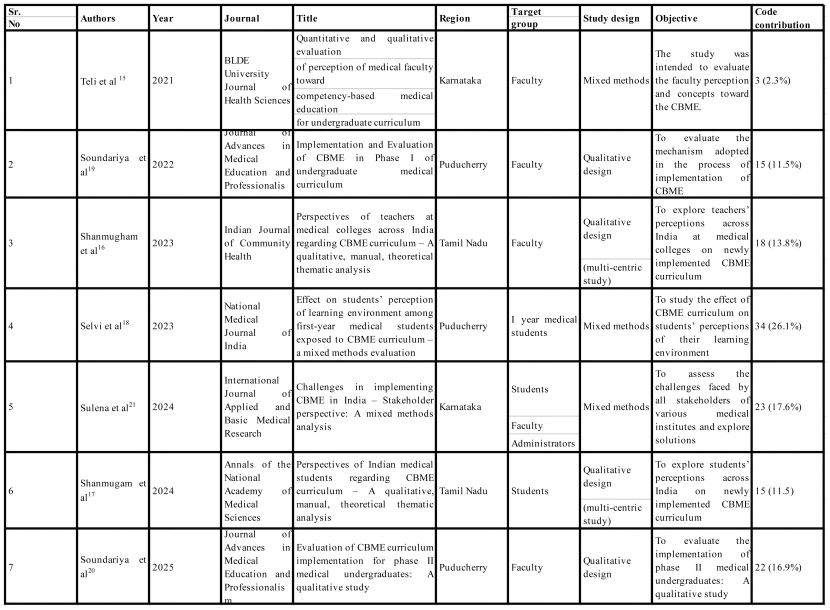
We adopted a pragmatic orientation in conducting this meta-synthesis, where studies of various qualitative designs are integrated. Given our objective to aggregate and describe, we decided to remain open by following a ‘meta-analytic principle’ that values the contribution of each study.22 However, to balance inclusivity and rigor, authors also applied Critical Appraisal Skills Programme (CASP)23 checklist questions to assess methodological quality and ensure that selected studies met minimum standards. The final decision on inclusion of the study was made in consensus among all authors. While the authors could not make a decision on one CASP question “Has the relationship between researchers and participants been adequately considered?” due to insufficient information in primary studies, they unanimously agreed that all articles met the criteria for the remaining nine questions. In addition, Table 1 outlines the distribution of codes derived from each study, indicating the extent of their contribution to the overall meta-synthesis.
The published qualitative results from seven selected studies were extracted to form the corpus for analysis. The data consisted of narratives, participant quotes, categories and themes. We carried out descriptive coding of all relevant text data from the results sections of selected papers using the free version of QDA Miner Lite software. As part of CIS, under RTA, we identified common themes and metaphors across multiple studies to develop a cumulative understanding of the subject matter. This approach allowed us to synthesize insights from diverse sources, strengthening overarching conceptual frameworks. Under Refutational Synthesis, we examined contradictions and disagreements between studies, critically evaluating divergent perspectives to challenge assumptions and refine interpretations. Finally, LOA Synthesis was applied when studies focused on different aspects of a phenomenon. This method integrates varied perspectives by assembling distinct pieces of evidence across curricular components, creating a comprehensive and coherent argument that enhances the depth of analysis.
The descriptive results were presented as converging and diverging factors under various headings of curricular components. Converging factors refer to supportive forces or viewpoints that strengthen a particular change, while diverging factors represent resisting or opposing forces that work against it. The first author (AD) conducted the initial analysis, which was then reviewed by the other two authors (PD and HP) through an iterative process of discussion, revision, and re-analysis. The description of themes, interpretation and discussion of manuscript was written in consensus. Text enclosed in square brackets represents the author’s statement, while text in Italics denotes direct quotes from the primary studies.
We followed the 'Enhancing Transparency in Reporting the Synthesis of Qualitative Research' framework for meta-synthesis.24
The present qualitative meta-synthesis did not require submission to the ethics committee clearance as per the addendum to National Ethical Guidelines for Biomedical and Health Research involving human participants by the Indian Council of Medical Research (2024).25
Seven studies were included in the present qualitative meta-synthesis, primarily led by private medical colleges in the southern region of India. The coded content is organized into curricular categories. We used 130 descriptive codes to code the relevant content and then organized it under six categories, with competencies (1), curriculum content (28) and teaching-learning methods (24), curriculum governance (28), student support and educational environment (19), student assessment (17), and faculty development (13). A summary is presented in Figure 2 where the size of the arrows approximately represents the number of items under the given category.

Figure 2 Converging and diverging factors across various CBME curricular components
Abbreviations: FC- Foundation Course, ECE-Early Clinical Exposure, FAP – Family Adoption Programme, AETCOM – Attitude, Ethics and Communication, SDL – Self-directed learning
Framing objectives to numerous competencies (under CBME curriculum) was perceived as a challenge necessitating the refresher training for it.19 Coordination and preparing a lesson plan for an integrated session was reported to be a time-taking activity.19
The curriculum, incorporating both vertical and horizontal integration of content,18 has been analyzed through several converging and diverging factors. Students found the Foundation Course instrumental in helping them adjust to their new academic environment.17 Ice-breaking activities and sports played a crucial role in fostering peer connections within the cohort.17 However, while the Foundation Course was considered important, its extended duration was perceived as overwhelming by some students, leading to content overlap, repetition, and exhaustion—factors that risked fostering an aversion to the subject.17,20 Faculty suggested reducing the duration of the Foundation Course to enhance its effectiveness.16
Students noted that Early Clinical Exposure (ECE) sessions helped bridge basic science concepts with clinical situations. Similarly, Cardiopulmonary Resuscitation (CPR) and Basic Life Support (BLS) sessions instilled a sense of professional identity.17 Competency sessions related to disability cultivated a deeper understanding of patient needs—“The session on disability competencies made me realize the huge population with disabilities and their special needs.”17 However, ECE sessions in Phase 1 were reported to be overwhelming for teachers and distracting for students. Faculty observed that premature clinical exposure led students to jump to conclusions without fully grasping basic science concepts, diminishing the effectiveness of these sessions.16
Students felt that ethics classes in the Attitude, Ethics and Communication (AETCOM) module, alongside extracurricular activities, had a meaningful impact.18 They noted that AETCOM sessions sensitized them to their responsibilities as future professionals. The inclusion of ethics, empathy, and communication topics was highly appreciated by students, as these are not routinely taught.21 Observing simulated doctor-patient interactions helped students identify weaknesses in their communication skills. Sessions on “breaking bad news” and yoga were deemed beneficial, although students expressed a desire for expert guidance in yoga.17 Despite its importance, AETCOM sessions were often perceived by students as overly theoretical,21 indicating a need for a more interactive and applied approach.
The Family Adoption Programme (FAP) faced faculty criticism due to vague norms and expectations—for instance, guideline suggesting that enrollment of families outside the field practice area and preferably underserved by the public health system.16 [FAP is a longitudinal community-based activity, where the student is assigned to a few families typically from rural and underserved area to adopt and follow throughout their medical course]. Students proposed the inclusion of research-related sessions and activity-based teaching to enhance engagement.18 The faculty emphasized the need to align curriculum content with the National Level Exit Exam to sustain student interest.21
Teaching-learning methods were evaluated based on students' and faculty members' perspectives. Students appreciated small group teaching, case-based learning, self-directed learning (SDL) sessions, tutorials, E-learning, and hospital visits.18 They also found reinforcement sessions beneficial.17,18,20 Visits to health centers were perceived as a valuable experience by students. At first, they had only seen such health centers in their residential areas, but later, through formal exposure visits organized by the Department of Community Medicine, they developed the deeper understanding of their important role in healthcare delivery.18
Integrated sessions and ECE were perceived as engaging.17 Overall, students felt that simulation-based training, training using scenarios were impactful in better student engagement.21
Faculty members expressed a need for clarity on conducting SDL sessions and requested training to improve their delivery.17,19,21 Furthermore, faculty raised concerns that the SDL approach might not be suitable for all students [as all might not be ready or capable of self-directed learning].21 Additionally, they lacked orientation on preparing materials for active learning strategies.20 Other challenges included the extensive time required for planning integrated sessions, structuring SDL sessions in absence of guidelines, allocating adequate time, and ensuring systematic execution.20 Simulation-based teaching was also emphasized as a critical component for maintaining curriculum effectiveness.20,21
Maintaining reflective writing for ECE, SDLs, logbooks, and subject records was considered time-consuming and burdensome for students.17 Similarly, handwritten assignments were viewed as a challenge, prompting suggestions to transition to online typed submissions, given the tech-savviness of the present generation.
Students found multiple-choice question (MCQ) tests welcoming, as they struggled to construct logical long-answer responses within the stipulated time.17 Students considered MCQs as one of the strengths of the CBME curriculum.18 However, faculty faced challenges in designing MCQ-based assessments due to the extensive groundwork required. Additionally, there was limited awareness among faculty regarding various formative assessment tools applicable to lectures and small-group teaching, resulting in reduced utilization of formative assessment for integrated learning. The assessment of the affective domain and written reflections remained infrequent, primarily due to difficulties in objectively assessing these components.20 In addition, faculty perceived challenges in conducting assessments in integration sessions.20
Faculty also lacked training in the practical aspects of Objective Structured Clinical Examinations (OSCE) and Objective Structured Practical Examinations (OSPE), further complicating efforts to enhance assessment methodologies.20 Providing feedback to large numbers of students posed an additional challenge. Students expressed concerns over excessive documentation requirements in logbooks and suggested streamlining these processes.21
Several systemic challenges were identified, including a lack of student preparedness, their prioritization of training for postgraduate entrance exam over curriculum-based learning, and inadequate faculty training.21 Additionally, resource constraints—particularly in infrastructure—alongside the need for more frequent assessments, hindered the development of a robust evaluation framework.15 Faculty emphasized the necessity of improving facilities such as skills laboratory and Information Technology (IT) support to enhance the overall assessment system.21
A well-organized timetable and adequate resources, such as increased availability of cadavers, were identified as converging factors contributing to effective curriculum implementation.21 However, faculty with the MSc qualification were neither perceived as effective in facilitating sessions on ECE, AETCOM, and the Foundation Course, nor in supporting students in achieving professional competence.17 Non-medical faculty were observed to face difficulties in teaching clinical concepts, though they were considered suitable for tutoring roles – “Faculty with MSc qualification can be considered as tutors for teaching paramedics” (p.34).16
Several administrative challenges were recognized by faculty as diverging factors. These included delays in uploading educational materials to the Learning Management System (LMS), delays in distributing logbooks, and the difficulty of adapting to frequent curriculum changes mandated by regulatory bodies.20 Effective curriculum governance was found to depend on departmental coordination, adequate financial and human resources, thorough pre-planning, and ensuring a solid groundwork. Finally, periodic evaluation and incremental improvement in the skills module was felt to be a challenge.20
Apart from one study that emphasized student support—including assistance for low achievers, motivation, faculty guidance, peer collaboration, infrastructure, and a ragging-free campus18 —these aspects received limited attention in other studies. Students proposed integrating more extracurricular activities and outings to enhance engagement. Additionally, insufficient sensitization regarding CBME contributed to disengagement with curricular changes, diminished motivation, lower attendance, and a tendency to prioritize preparation for postgraduate entrance exam over regular coursework.21
A strong faculty team—characterized by motivation, expertise, dedication, punctuality, care, and approachability—was identified as a key converging factor in driving meaningful curricular change.18 However, resistance to new developments was prevalent among senior teachers [experienced professors], who believed the traditional curriculum was sufficient.16,21 The faculty hesitated to adopt newer methodologies due to concerns over increased workload.21 There were concerns about the insufficient faculty-to-student ratio and the limited preparedness for the implementation of CBME, particularly among clinical faculty.16
To address these challenges, the need for training senior residents and assistant professors in medical education—particularly interactive teaching—was emphasized, as many are actively involved in instruction but lack formal training in pedagogical techniques.21 Poor interdepartmental collaboration, lack of teamwork and limited awareness among faculty from clinical departments further hindered effective curriculum implementation/learning.21
The present qualitative meta-synthesis could explore various converging and diverging factors for various components in CBME curriculum. Students seem to have a positive response to the educational reforms under CBME curriculum. Faculty, however, reported to have faced more challenges due to disruptions in established practices, contextual constraints, and frequent changes in curriculum guidelines and greater student-faculty ratio. These findings suggest dissonance due to a break in the status quo that demands substantial adaptation and governance, forcing administrators and educators to modify their ongoing approaches while navigating institutional and policy-based complexities. According to Lewin’s framework, this state is called a state of disequilibrium, where faculty tend to experience dissonance due to disruption of prior norms. Application of such adaptive frameworks in managing challenges have a potential to alleviate faculty resistance, ensure long-term commitment,26 and provide contextual solutions.27
Since 2009, erstwhile MCI and subsequently NMC have implemented National Faculty Development Programs (FDPs) to train, guide and support faculty at all medical colleges in India.28 FDPs for capacity building in CBME have included Basic Course Workshop (BCW), Revised Basic Course Workshop (rBCW), and Basic Course in Medical Education (BCME) that train faculty members at the level of Assistant Professor and above with at least three years’ experience. Advance Course in Medical Education (ACME) and Curriculum Implementation Support Program (CISP I to III) are designed for faculty who become members of curriculum committee and Medical Education Unit after having completed the basic course.29 NMC-accredited Nodal and Regional Centers conduct the training of faculty through institutional nomination. The Foundation for Advancement of International Medical Education and Research (FAIMER) significantly contributed to the faculty development movement in India by training fellows through educational innovation projects with an emphasis on leadership and change management skills.30 Many of these fellows serve as faculty at NMC nodal centers and lead medical education units at their institutions.31
Given the complex nature of the education system—where stakeholders are interwoven in a non-linear network, emergent behaviors tend to be unpredictable, and the trajectory of change is shaped by cumulative reactions and responses.32 Consequently, the persistence of dissonance, even after considerable capacity-building efforts, is an inherent feature of such a complex system rather than a reflection of inefficacy. A deeper understanding of both converging and diverging factors enables institutions to navigate challenges more effectively and refine adaptive strategies that actually work. In this context, a collaborative approach—wherein faculty actively co-develop strategies tailored to their specific institutional needs—proves more effective than singular, externally imposed interventions, as it fosters ownership, contextual relevance, and sustained impact.33 Finally, in such complex and uncertain educational settings, decision-makers at all levels are encouraged to practice adaptive leadership—asking challenging questions, pushing out of their comfort zones and managing the resulting distress.34
Scoping reviews of medical education research in India indicate that most studies have primarily concentrated on Kirkpatrick Level 1 evaluations (satisfaction) among undergraduate students, often relying on survey methods.35,36 For a successful change, educational researchers should be aware of the complexity of educational problems, the nature of evidence in educational research37 and focus on problem-solving rather than just fact-finding or verifying research.38 To support this, Design-Based Research (DBR) in education stands out for its emphasis on real-world practitioner concerns, fostering close collaboration among educators, designers, and researchers. By integrating context-specific characteristics into interventions, DBR ensures that solutions are not only theoretically sound but also practically relevant, leading to sustainable and adaptive improvements in educational systems.39 Change leaders need to consider the results of local research, also political, public, regulatory, and institutional influences while consensus-building for change management is vital. Kotter’s eight-step management model offers a structured approach to bridge the gap between research evidence, decision-makers at policy level and practitioners at institute level. It emphasizes the need to create a sense of urgency, establish a guiding coalition, articulate and communicate a clear change vision, empower actions, and inspire teams to drive meaningful transformation.40 Educational projects focused on solving context-specific problems should be funded and recognized as a key component of the professional development of faculty.38
The strength of this paper lies in its critical interpretive synthesis, which not only integrated diverse perspectives into a cohesive framework, but grounded the discussion and recommendations in reflexive analysis of the data, informed by contextual insights, and aligned with the existing literature to ensure relevance and coherence. By consolidating diverse insights from reported qualitative studies, it offered a comprehensive understanding of the appropriately complex subject.
Though all included studies were led by private colleges in southern India, three qualitative studies adopted a multicentric approach, incorporating perspectives from various institutions in other regions of the country. Contextual challenges in government medical colleges may be underrepresented. Hence, in future more studies from such settings can offer value in producing their context-specific insights. Notably, all uncoded text data was re-reviewed post-coding to ensure no data was overlooked. In addition to understanding the factors influencing CBME curriculum implementation, future educational projects should focus on documenting change management strategies that facilitate the effective implementation of curriculum in their settings.
In conclusion, this meta-synthesis examined the complex challenges shaping CBME implementation in India, highlighting key challenges and the need for change-oriented research to improve outcomes. It offers practical insights for curriculum planners and emphasizes the importance of faculty career development in leadership and change management. The success of CBME curriculum implementation would thus depend on committed faculty, adaptive institutional leadership, and a context-sensitive regulatory framework that goes beyond requiring passive compliance to one that actively supports innovation, collaboration, and locally relevant reforms.
1. Kaushik A, Jaiswal A, Singh AK, Rizvi G. Challenges to New Undergraduate Medical Curriculum Due to COVID-19 Pandemic and Possible Solution in India. Medical Journal of Dr DY Patil Vidyapeeth 2022;15(3):319. https://doi.org/10.4103/mjdrdypu.mjdrdypu_263_20
Crossref
2. UG Curriculum | NMC. https://www.nmc.org.in/information-desk/for-colleges/ug-curriculum/ (accessed 24 May2025)
3. Graduate Medical Education Regulations, 1997 | NMC. Retrieved from: https://www.nmc.org.in/rules-regulations/graduate-medical-education-regulations-1997/ (accessed 27 Jul2025)
4. Medical Council of India. Regulations on Graduate Medical Education (Amendment), 2019 [Gazette notification]. Gazette of India (Extraordinary, Part III – Sec 4). 2019.https://www.nmc.org.in/ActivitiWebClient/open/getDocument?path=/Documents/Public/Portal/Gazette/GME-06.11.2019.pdf
5. National Medical Commission. Guidelines for Competency-Based Medical Education (CBME) Curriculum 2024. [Government circular]. 2024.https://www.nmc.org.in/MCIRest/open/getDocument?path=/Documents/Public/Portal/LatestNews/organized_compressed.pdf
6. Pandya H, Chacko T, Mohammed CA. Regulatory system to promote the culture of quality at Indian medical schools: Are we doing enough? The National Medical Journal of India 2022;34(5):298–301. https://doi.org/10.25259/NMJI_996_20
Crossref PubMed
7. Rashmi Ramanathan, Jeevithan Shanmugam, Magadi Gopalakrishna Sridhar, Kalaniti Palanisamy, Seetharaman Narayanan. Exploring faculty perspectives on competency-based medical education: A report from India. Journal of Education and Health Promotion 2021;11(9):1–6. DOI: https://doi.org/10.4103/jehp.jehp_1264_20
8. Desai C, Shah N, Jorwekar G, Badyal D, Singh T. Competency-based medical education: An overview and application in pharmacology. Indian Journal of Pharmacology 2016;48(7):5. https://doi.org/10.4103/0253-7613.193312
Crossref
9. Kandi V. Are Medical Graduates Adequately Trained? A Critical Viewpoint on Factors Influencing Medical Education in India. American Journal of Educational Research 2025;13(1):29–37. https://doi.org/10.12691/education-13-1-4
Crossref
10. Timulak L, Creaner M. Essentials of Qualitative Meta-Analysis. American Psychological Association; 2023. 978-1-4338-3848-4.https://www.jstor.org/stable/j.ctv2vg072m (accessed 7 Nov2024)
Crossref
11. Dongre, AR, Deshmukh, PR, Pandya, H. Converging and Diverging Factors for CBME curriculum for Indian Medical Graduates: Insights from a Qualitative Meta-Synthesis. OSF Registries. 2025. https://osf.io/uhvc9 (accessed 11 Jun2025)
12. Nested Knowledge [Internet]. St. Paul (MN): Nested Knowledge; c2025 [cited 2025 Feb 21]. Available from: https://nested-knowledge.com/
13. Kirkpatrik D. Techniques for Evaluation Training Programs. Journal of the American Society of Training Directors 1959;13:21–26
14. Dixon-Woods M, Cavers D, Agarwal S, Annandale E, Arthur A, Harvey J et al. Conducting a critical interpretive synthesis of the literature on access to healthcare by vulnerable groups. BMC Medical Research Methodology 2006;6(1):35. https://doi.org/10.1186/1471-2288-6-35
Crossref PubMed PMC
15. Teli A, Harakuni S, Kamat C. Quantitative and qualitative evaluation of perception of medical faculty toward competency-based medical education for undergraduate curriculum. BLDE University Journal of Health Sciences 2021;6(2):143. https://doi.org/10.4103/bjhs.bjhs_103_20
Crossref
16. Shanmugam J, Ramanathan R, Kumar M, Gopalakrishna SM, Palanisamy KT, Narayanan S. Perspectives of Teachers at Medical Colleges Across India regarding the Competency based Medical Education Curriculum – A Qualitative, Manual, Theoretical Thematic Content Analysis. Indian Journal of Community Health 2023;35(1):32–37. https://doi.org/10.47203/IJCH.2023.v35i01.007
Crossref
17. Shanmugam J, Ramanathan R, Kumar M, Sridhar MG, Palanisamy KT, Narayanan S. Perspectives of Indian medical students regarding the competency based medical education curriculum – A qualitative, manual, theoretical thematic content analysis. Annals of the National Academy of Medical Sciences (India) 2024;60(3):206–212. https://doi.org/10.25259/ANAMS-2023-6-14-(965)
Crossref
18. Selvi KS, Shanmugarajah MM, Dongre AR. Effect on students’ perception of learning environment among first-year medical students exposed to competency-based curriculum: A mixed-methods evaluation. The National Medical Journal of India 2023;36(1):40–43. https://doi.org/10.25259/NMJI_257_21
Crossref PubMed
19. Soundariya K, Kalaiselvan G, Rajalakshmi M, Sindhuri R. Implementation and Evaluation of Competency-based Medical Education in Phase I of Undergraduate Medical Curriculum. Journal of Advances in Medical Education Professionalism 2022;10(4):228–234. https://doi.org/10.30476/JAMP.2022.94999.1616
PubMed PMC
20. Soundariya K, Nishanthi A, Mahendran R, Vimal M. Evaluation of Competency-Based Medical Education (CBME) curriculum implementation for Phase II Medical undergraduates: A qualitative study. Journal of Advances in Medical Education Professionalism 2025;13(1):36–48. https://doi.org/10.30476/jamp.2024.104312.2052
PubMed PMC
21. Sulena S, Kulkarni A, Mathur M, Jyoti N, Sidhu TK, Badyal D et al. Challenges in Implementing Competency-based Medical Education in India – Stakeholders’ Perspective: A Mixed-method Analysis. International Journal of Applied and Basic Medical Research 2024;14(4):225–232. https://doi.org/10.4103/ijabmr.ijabmr_268_24
Crossref
22. Booth A, Noyes J, Flemming K, Gerhardus A, Wahlster P, Van Der Wilt GJ et al. Guidance on choosing qualitative evidence synthesis methods for use in health technology assessments of complex interventions. 2016.http://www.integrate-hta.eu/downloads/
23. Critical Appraisal Skills Programme. CASP Checklist: For Qualitative Research. 2024.https://casp-uk.net/casp-tools-checklists/qualitative-studies-checklist/
24. Tong A, Flemming K, McInnes E, Oliver S, Craig J. Enhancing transparency in reporting the synthesis of qualitative research: ENTREQ. BMC Medical Research Methodology 2012;12(1):181. https://doi.org/10.1186/1471-2288-12-181
Crossref PubMed PMC
25. Indian Council of Medical Research, New Delhi. Ethical Requirements for Systematic Review and Meta-analysis Proposals. 2024.https://www.icmr.gov.in/icmrobject/uploads/Guidelines/1724842157_ethical_requirements_for_systematic_review_metaanalysis_propo (accessed 12 Dec2024)
26. Albanese MA, Mejicano G, Anderson WM, Gruppen L. Building a competency-based curriculum: the agony and the ecstasy. Advances in Health Sciences Education 2010;15(3):439–454. https://doi.org/10.1007/s10459-008-9118-2
Crossref
27. Adelman C. Kurt Lewin and the Origins of Action Research. Educational Action Research 1993;1(1):7–24. https://doi.org/10.1080/0965079930010102
Crossref
28. Medical Council of India. Faculty Development Initiatives: 10 years’ experience - Status Report. https://www.nmc.org.in/wp-content/uploads/2020/09/FDP-initiative-UG-Med-Education.pdf (accessed 4 Jun2025)
29. National Medical Commission. National Faculty Development Programme | NMC. https://www.nmc.org.in/information-desk/for-colleges/national-faculty-development-programme/ (accessed 3 Jun2025)
30. Vyas R, Morahan PS, Yuan S, Amaral E, Burch V, Campos HH et al. FAIMER Global Faculty Development: A Sustainable Partnership Model to Advance Health Professions Education. Academic Medicine 2023;98(10):1131. https://doi.org/10.1097/ACM.0000000000005264
Crossref PubMed PMC
31. Yuan S, Rahim A, Kannappan S, Dongre A, Jain A, Kar SS et al. Success stories: exploring perceptions of former fellows of a global faculty development program for health professions educators. BMC Medical Education 2024;24(1):1072. https://doi.org/10.1186/s12909-024-05823-2
Crossref PubMed PMC
32. Wolf-Branigin M. Using complexity theory for research and programme evaluation. New York: Oxford University Press; 2013. https://doi.org/10.1093/acprof:oso/9780199829460.001.0001
Crossref
33. Barman L, Silén C, Bolander Laksov K. Outcome based education enacted: teachers’ tensions in balancing between student learning and bureaucracy. Advances in Health Sciences Education 2014;19(5):629–643. https://doi.org/10.1007/s10459-013-9491-3
Crossref PubMed
34. Heifetz RA, Laurie DL. The work of leadership. Harvard Business Review 1997;75(1):124–134. https://pubmed.ncbi.nlm.nih.gov/10174450/
35. Dongre AR, Deshmukh PR. Current Status of Medical Educational Research in India and Way Forward. Journal of Research in Medical Education Ethics 2019;9(1):73–78. https://doi.org/10.5958/2231-6728.2019.00013.1
Crossref
36. Kumar D, Varma J, Dongre A, Pandya H. Scoping review of published research on medical education in India during the Covid-19 pandemic. The National Medical Journal of India 2023;35(4):243–246. https://doi.org/10.25259/NMJI_636_21
Crossref PubMed
37. Harden RM, Grant J, Buckley G, Hart IR. Best Evidence Medical Education. Advances in Health Sciences Education: Theory and Practice 2000;5(1):71–90. https://doi.org/10.1023/A:1009896431203
Crossref
38. Dongre A, Pandya H. Navigating complexities: Improving evidence quality in Indian medical education research. Global Journal of Health Sciences and Research 2025;3(1):1–5. https://doi.org/10.25259/GJHSR_30_2025
Crossref
39. Dolmans DHJM, Tigelaar D. Building bridges between theory and practice in medical education using a design-based research approach: AMEE Guide No. 60. Medical Teacher 2012;34(1):1–10. https://doi.org/10.3109/0142159X.2011.595437
Crossref PubMed
40. Kotter J. Leading Change: Why Transformation Efforts Fail. Engineering Management Review, IEEE 2007;37. https://doi.org/10.1109/EMR.2009.5235501
© Education for Health.
Education for Health | Volume 38, No. 4, October-December 2025