Marcela Cisternas1, Francisco Garrido2, Solange Rivera3, Marcela Bitran4, Natalie Thone5, Arnoldo Riquelme6, Natalia Gana7, Claudio Nazar8, Javier Rodriguez9, Marisol Sirhan10, Claudia Valdes11, Felipe Heusser12, and Lili Moraga13
1MD, Associate Professor. Dean’s office, Faculty of Medicine. Department of Clinical Immunology and Rheumatology, School of Medicine, Pontificia Universidad Católica de Chile, Santiago, Chile
2MD, Assistant Professor. Undergraduate Medical School Direction, School of Medicine. Department of Radiology, School of Medicine, Pontificia Universidad Católica de Chile, Santiago, Chile
3MD, Associate Professor. Department of Family Medicine, School of Medicine, Pontificia Universidad Católica de Chile, Santiago, Chile
4PhD, Associate Professor. Center for Medical Education and Health Sciences, Faculty of Medicine, Pontificia Universidad Católica de Chile, Santiago, Chile
5MD, Assistant Professor. Department of Otorhinolaryngology, School of Medicine, Pontificia Universidad Católica de Chile, Santiago, Chile
6MD, Full Professor, Department of Gastroenterology, School of Medicine, Pontificia Universidad Católica de Chile, Santiago, Chile
7Full Professor, Department of Gastroenterology, School of Medicine, Pontificia Universidad Católica de Chile, Santiago, Chile
8MD, Associate Professor. Division of Anesthesiology, School of Medicine, Pontificia Universidad Católica de Chile, Santiago, Chile
9MD, Department of Oncologic Surgery, School of Medicine, Pontificia Universidad Católica de Chile, Santiago, Chile
10MD, Associate Professor, Center for Medical Education and Health Sciences, Faculty of Medicine. Department of Gastroenterology, School of Medicine, Pontificia Universidad Católica de Chile, Santiago, Chile
11Professional Assistant, Center for Medical Education and Health Sciences, Faculty of Medicine, Pontificia Universidad Católica de Chile, Santiago, Chile
12MD, Full Professor, Dean’s office, Faculty of Medicine, Department of Pediatric Cardiology, School of Medicine, Pontificia Universidad Católica de Chile, Santiago, Chile
13MD, Associate Professor. Center for Medical Education and Health Sciences, Faculty of Medicine. Department of Family Medicine, School of Medicine, Pontificia Universidad Católica de Chile, Santiago, Chile
ABSTRACT
Medical education is undergoing significant transformations to better align with evolving healthcare needs. In 2015, the Pontificia Universidad Católica de Chile implemented a major curricular reform in its School of Medicine, shifting from a traditional 7-year program to an integrated, competency-based 6-year curriculum. This study aimed to assess the academic outcomes, clinical competencies, and differences in student well-being between both curricula.
Methods: We conducted a prospective, longitudinal, comparative study of two cohorts: the last cohort under the traditional curriculum and the first cohort under the new curriculum. Three measurements were carried out along the study program: at the beginning, at the middle and at the last year of the program. Academic performance, professionalism, and clinical competencies were evaluated using standardized written tests, OSCEs and the National Medical Exam (EUNACOM). In addition, we compared the courses grades and attrition statistics along the studies. At these three points, students also answered a range of self-reporting instruments regarding distress, burnout, well-being, mindfulness, empathy and the educational environment.
Results: Both cohorts achieved similar average grades and EUNACOM scores. The new curriculum cohort had a significantly lower course failure rate (7.6% vs 13%, p<0.01) and better outcomes in professionalism and communication. Final OSCE scores were slightly higher in Obstetrics/ Gynecology and Family Medicine. Despite these improvements, both cohorts showed high and increasing levels of stress, burnout, and declining empathy, particularly in the final years. While the elevated levels of stress and anxiety observed among medical students are extensively documented in the literature, the COVID-19 pandemic may have exerted an additional influence on these outcomes.
Conclusion: The new curriculum maintained academic performance while enhancing professionalism and reducing failure rates and training time. However, persistent mental health challenges underscore the need for stronger and more effective support systems. These findings reveal the value of competency-based education while highlighting the importance of holistic curricular evaluation.
Key Words: medical education, curricular reform, competence-based curriculum, active methodologies, professionalism, well-being, educational environment
Date submitted: 23-June-2025
Email: Marcela Cisternas (cisternas.marcela@gmail.com)
This is an open access journal, and articles are distributed under the terms of the Creative Commons Attribution-Non Commercial-Share Alike 4.0 License, which allows others to remix, tweak, and build upon the work non-commercially, as long as appropriate credit is given and the new creations are licensed under the identical terms.
Citation: Cisternas M, Garrido F, Rivera S, Bitran M, Thone N, Riquelme A, Gana N, Nazar C, Rodriguez J, Sirhan M, Valdes C, Heusser F, and Moraga L. Longitudinal evaluation of a major curricular reform in undergraduate medical education: a cohort study from Chile. Educ Health 2025;38:336-346
Online access: www.educationforhealthjournal.org
DOI: 10.62694/efh.2025.376
Published by The Network: Towards Unity for Health
Healthcare systems worldwide are rapidly evolving, requiring the responsive adaptation of medical education. Globalization, technology, online access to knowledge, social accountability and patient safe care have posed new challenges, and healthcare systems must adapt to the new scenarios, such as pandemics, and to meet the evolving needs of society.1 Furthermore, society’s and patients’ expectations have changed, demanding more empathetic doctors, capable of working in interprofessional environments and adapting to emerging technologies.2,3
In Chile, with a population of nearly 20 million people, there are 28 medical schools that graduate 2,500 students each year.4 Although the number of physicians has increased over the past decades, our country continues to face a significant gap in access to specialists, with a rate of 1.5 per 10,000 inhabitants, well below the OECD average of 2.35.5
Traditionally, Chilean medical schools have followed a Flexnerian-type 7-year curriculum with standard teaching and assessment methodologies, where the curriculum is fragmented into basic, preclinical and clinical learnings, and methodologies are mostly in big round classes and tutorial teaching at the patient’s bedside. The lack of content integration, the delayed clinical exposure, and the reliance on passive, teacher-centered pedagogical methodologies raise our concerns regarding the preparedness of future physicians to adequately address the evolving demands of the medical field.
In 2015, after six years of deep community work that involved academics, students and alumni, our school of medicine implemented a major curricular reform that reduced training to six years, becoming the first in Chile to do so. Beyond efficiency, the new curriculum features horizontal and vertical integration, is sequenced by organ and system problems, promotes early clinical contact and places a strong emphasis on professionalism. Active student-centered methodologies were introduced to foster deep learning and to encourage autonomous and continuous self-education.6
To evaluate the quality and effectiveness of the new curriculum, a prospective and longitudinal study was designed following Kern’s approach to curriculum development. Kerns systematic approach to curriculum design incorporates, as its sixth component, the evaluation and feedback of curriculum implementation using objective and structured assessment methods.7,8 The aim was to compare the educational results between two student cohorts: the last one of the traditional curriculum and the first one of the new one. Given the concern for the well-being and mental health of medical students, we estimated that, in addition to academic outcomes, it was necessary to evaluate the students’ distress and well-being in relation to the curricula. Additionally, this study was intended to closely monitor the curricular changes and introduce necessary adjustments in the event of any major difficulties arising.
This paper presents the results of a prospective, longitudinal study comparing cohorts before and after reform, assessing academic outcomes, professionalism, student’s well-being, burnout, and the educational environment
We conducted a prospective and longitudinal study, approved by our Ethics Committee, comparing two student cohorts: the last student under the 7-year curriculum (2014 admission, cohort A) and the first under the 6-year curriculum (2015 admission, cohort B). Both cohorts entered via identical admission requirements, with no special selection for curricular innovation ensuring equivalence at baseline.
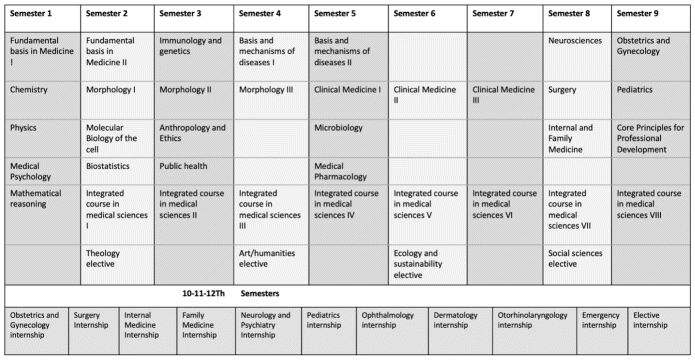
The structure of the new curriculum (Table 1):
Table 1 Structure of the new curriculum (2015)
Outcomes evaluated (Table 2,3):
Table 2 Academic outcome’s assessment tools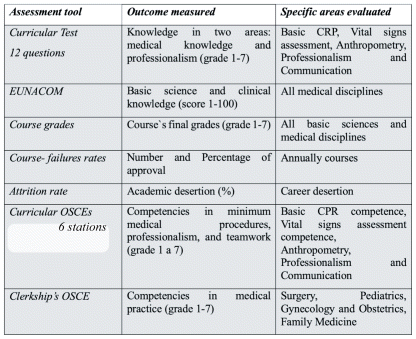
Table 3 Assessment tool for students’ perceptions of distress, well-being and educational environment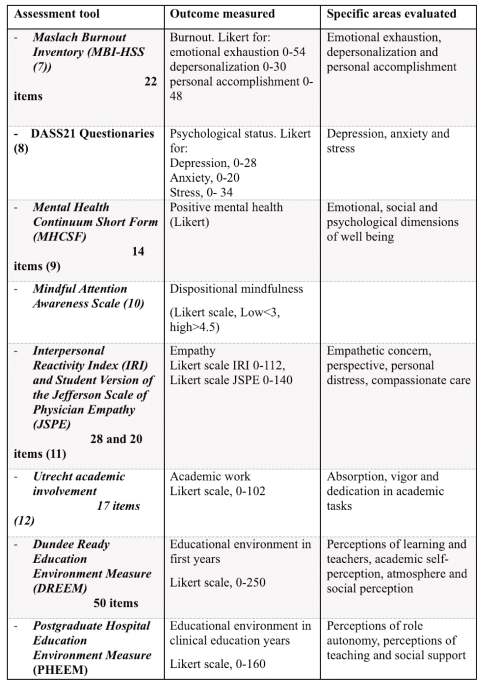
To compare repeated measures of categorical variables within the same cohort, the X2 Friedman’s test was used and for numerical variables, the ANOVA or Student’s t-test was applied. To compare the two cohorts’ continuous results, we used the ANOVA test for independent measures. An alpha value of 5% was established a priori. Analyses were performed in STATA v15.0.
Both cohorts were equivalents regarding admission requirements and demographics characteristics (age, gender), with 123 students admitted in cohort A and 132 in cohort B.
Annual grades (1 to 7 scale) of the pre-internship undergraduate years were similar between both cohorts (mean 6.12 in cohort A and 6.26 in cohort B) and the same at the internship period (6.75) Attrition rate was less than 1% in both cohorts. Sixteen students from Cohort A and 10 from Cohort B failed at least in one pre-internship course (failure rate 13 % vs 7.6%, p<0.01)
Students in both cohorts obtained comparable results on the EUNACOM, exhibiting no significant differences in achievement percentages, pass rates, or average and total scores.
In the curricular written test, cohort B demonstrated superior performance compared to cohort A in the first and second assessments. Specifically, cohort B achieved significantly better results on questions evaluating professionalism. In the final assessment, both cohorts achieved similar results.
Three OSCEs were administered: One in the first year, one in the middle of the curriculum, and one at the end of four clerkships. Both cohorts achieved similar results in the measurements carried out at the beginning (first year) and at the middle of the curriculum. Cohort B achieved slightly better outcomes in Obstetrics and Gynecology and in Family Medicine clerkships’ OSCEs than cohort A. (Table 4)
Table 4 Final OSCE performance by discipline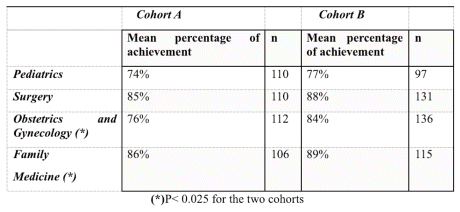
The most relevant results in the self-report of students’ perceptions indicated a deterioration of mental health over the years. Cohort B entered the program with significantly lower levels of stress, depression, and anxiety; however, these scores increased significantly throughout their studies (Figure 1)
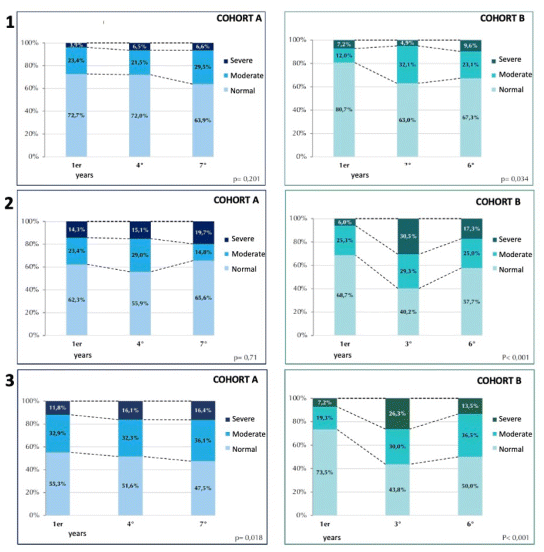
Figure 1 DASS21 results, showing the three dimensions: Depression (1), Anxiety (2) and Stress (3)
This increase in distress was not reflected in the level of positive mental health, which showed an improvement. No correlations were found between the increase in psychological distress and the levels of dispositional mindfulness, which remained stable. Additionally, there was a marked decrease in empathy levels in both cohorts (Table 5).
Table 5 Assessment results for students’ perceptions of distress, well-being and educational environment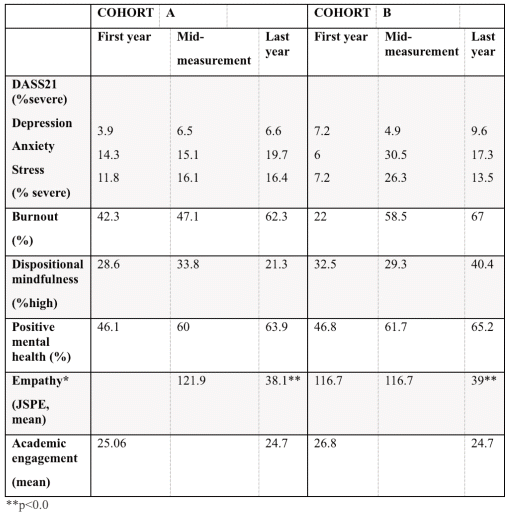
It is striking to observe the comparatively lower prevalence of burnout in cohort B (22%) upon their admission to the School of Medicine, which increased threefold at the last assessment. Two-thirds of the students of both cohorts reported experiencing burnout during their internship. (Figure 2) It is important to note that the internships were conducted in the year 2020, coinciding with the COVID-19 pandemic.
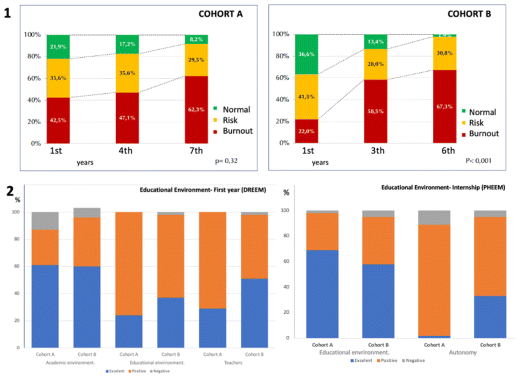
Figure 2 Burnout students’ perceptions (1) and educational environment (2)
Evaluations of the educational environment were significantly positive. In both cohorts, in the first and last year of studies, 98% of students rated the educational and social environment as “Good” or “Excellent,” while 95% evaluated the faculty and instructional quality as “Very Good” or “Excellent.” During the internship, 94% of students in Cohort B reported a highly positive or excellent perception of their own skills and work achievements, compared to 87% in Cohort A (Figure 2).
The field of medicine has undergone substantial changes in recent decades. The validated approach in healthcare today is “patient-centered”, emphasizing a personalized approach in an ambulatory setting, with a major focus on health promotion and disease prevention. This approach adheres to high standards of professionalism and should be delivered by an interprofessional team.15 Medical schools must foster the formation of leaders and change agents who are autonomous, responsible for their education, capable of making decisions based on a growing body of information, skilled in analyzing evidence, and committed to placing the patient at the center of their practice, meeting actual healthcare needs.16
According to the Liaison Committee on Medical Education (LCME), between 2017 and 2018, nearly 80% of medical schools in the United States had undergone or are implementing a deep reflection process, leading to significant curricular changes and reforms. The same is reported elsewhere in Europe and Asia, highlighting a widespread need to implement substantial changes in the content of undergraduate medical curricula, as well as teaching and assessment methods.17–19
Medical education has wrestled with the question of whether the length of time required for physician preparedness may be reduced. Shortening the degree program facilitates educational cost reduction, enhances access, and enables the graduation of younger physicians, thereby extending their career spans and serving the public good.20,21
Building upon international reports and with the analysis of the processes of self-evaluation and quality assurance, our School of Medicine implemented a curricular reform in 2015, guided by learning goals, emphasizing basic-clinical integration and early clinical exposure. It addressed the country’s main public health challenges, incorporated a strong focus on professionalism, ethics, and the humanities, and utilized active methodologies to promote continuous self-learning, leadership, and innovation. The curricular organization and its efficiency allowed the implementation of a 6-year curriculum plan.
While our school’s reform is inspired by international curricular models, its implementation in a Latin American context is unique and provides a framework for other Chilean schools.
A central element of the implementation of our curricular reform was the development of a prospective, comparative, and longitudinal study to assess the quality and outcomes of the new curriculum.
The mental health and well-being of health science students are of increasing concern over recent decades, with reports indicating a high prevalence of burnout, anxiety, and depressive symptoms among the students. Several factors influence this situation, including the heavy academic workload, extended working hours, and students’ self-imposed expectations, among others.22 A curricular change involving non-traditional methodologies challenges students, potentially serving as an additional factor contributing to anxiety and stress, so it was believed that assessing distress and well-being during the implementation was essential.
The results indicated that the new curriculum performed at least as well as the previous one, with the added benefit of producing general practitioners in a shorter time frame. This could be particularly beneficial for our country, which exhibits a disparity in access to healthcare, with a low rate of medical specialists per capita relative to recommended standards.
The similarity in average grades between both cohorts throughout the years and the comparable score on EUNACOM national examination between both cohorts suggests that the new curriculum sustains the quality of fundamental medical knowledge. The reduction in the failure rate in cohort B may indicate that the competency-based curriculum contributed to a better mastery of essential content and reduced academic barriers.
Results from the OSCE and professionalism-specific assessments revealed notable differences between cohorts. Cohort B performed better in professionalism and communication in early and mid-stage evaluations, suggesting that the new curriculum has strengthened these key competencies from the early years of training. The slight difference in final OSCEs in Obstetrics and Gynecology and Family Medicine by cohort B also suggests that the new curriculum may afford an advantage in clinical areas relevant to primary care, aligning with the curriculum’s focus on public health and local needs.
The assessment of mental health and well-being revealed high levels of stress, anxiety, and burnout in students from both curricula, particularly in the final stages of the program. Nearly 50% of students reported moderate or high levels of stress, and approximately one-third exhibited moderate to severe symptoms of depression. The high prevalence of burnout, affecting two-thirds of students by the end of their studies, underscores the need to reinforce psychosocial support strategies within the curriculum and educational environment. These findings align with the existing literature, which indicates that medical students often experience high levels of stress and burnout.23 The final measurement was carried out in 2020, during the COVID-19 pandemic, a global stressor that not only placed extraordinary demands on the healthcare community but also imposed considerable challenges on the education of health professions students.24
A major strength of this study lies in its prospective, longitudinal and comparative design, enabling the evaluation of two entire cohorts under different curricula. The use of multiple validated instruments and a national standardized exam provides a robust and multidimensional assessment, capturing not only academic achievement but also professional development and student well-being. While limited to a single institution, this approach offers valuable insights for other regional medical schools to consider similar reforms.
In conclusion, the new 6 years competency-based curriculum has proven to be at least as effective as the previous curriculum in terms of academic performance and preparation for the national examination. It also offers additional advantages in developing key competencies such as professionalism and communication. The reduction in failure rates and consistent performance in standardized exams highlight the value of this new curricular approach.
However, the prevalence of mental health issues, particularly stress, anxiety, depression, and burnout, indicates an urgent need to incorporate emotional and psychosocial education and support measures within the program. Our medical school recognizes this challenge and is developing curricular strategies and wellness resources to mitigate these negative effects, ensuring that the educational environment promotes medical competencies while also importantly supports balanced personal development. One of such initiatives is the inclusion of a self-care program in the curriculum, which has proven effective in reducing students’ burnout and stress.
In summary, the new 6-year competency-based curriculum maintained academic quality, reduced training time, and strengthened professionalism and communication. It also responds to urgent national health workforce needs and aligns with global trends in medical education reform. However, student well-being continues to present a significant challenge, requiring holistic institutional and curricular responses.
1. Stevens FCJ, Goulbourne JDS. Globalization and the modernization of medical education. Medical Teacher. 2012;34(10):e684–689. https://doi.org/10.3109/0142159X.2012.687487
Crossref PubMed
2. Thistlethwaite JE. Interprofessional education: implications and development for medical education. Educación Médica. 2015;16(1):68–73. https://doi.org/10.1016/j.edumed.2015.04.00
Crossref
3. Tokuç B, Varol G. Medical Education in the Era of Advancing Technology. Balkan Medical Journal. 2023;40(6):395–399. https://doi.org/10.4274/balkanmedj.galenos.2023.2023-7-79
Crossref PubMed PMC
4. Subsecretaría de Educación Superior. Buscador de carreras; 2025. Available from: https://www.mifuturo.cl/buscador-de-carreras/.5
5. O’Ryan M, Roncagliolo P. Training present and future doctors for Chile: how many and for what? The urgent need to review the physician quota generation model. Revista Médica de Chile. 2024;152(8):909–926. https://doi.org/10.4067/s0034-98872024000800909
6. Cisternas M, Rivera S, Sirhan M, Thone N, Valdés C, Pertuzé J, Puschel K. Reforma curricular de la carrera de Medicina de la Pontificia Universidad Católica de Chile. Revista Médica de Chile. 2016;144(1):102–107. https://doi.org/10.4067/S0034-98872016000100013
Crossref
7. Cisternas M, Rodríguez J, Llanos C, Garrido F, Nazar C, Thone N, Sirhan M, Gana N, Valdés C, Rivera S. Implementación de la reforma curricular de la Escuela de Medicina de la Pontificia Universidad Católica de Chile: analizando la experiencia. Revista Médica de Chile. 2022;150(6):821–827. https://doi.org/10.4067/S0034-98872022000600821
Crossref
8. Thomas P, Kern D, Hughes M, Tackett S, Chen B. Curriculum development for medical education: a six step approach. 4th ed. Johns Hopkins University Press; 2022
Crossref
9. Gil-Monte PR. The factorial validity of the Maslach burnout inventory-general survey (MBI-GS) Spanish version. Salud Publica de México. 2002;44:33–40. https://www.researchgate.net/publication/11453119_The_factorial_validity_of_the_Maslach_Burnout_Inventory-General_Survey
10. Lovibond S, Lovibond PF. Manual for the Depression Anxiety Stress Scales. 2nd edition. Sydney: Psychology Foundation; 1995
11. Echeverría G, Torres M, Pedrals N, Padilla O, Rigotti A, Bitran M. Validation of a Spanish version of the mental health continuum-short form questionnaire. Psicothema. 2017;29(1):96–102. https://doi.org/10.7334/psicothema2016.3
Crossref PubMed
12. Soler J, Tejedor R, Feliu-Soler A, Pascual JC, Cebolla A, Soriano J, Alvarez E, Perez V. Psychometric proprieties of Spanish version of Mindful Attention Awareness Scale (MAAS). Actas Españolas de Psiquiatría. 2012;40(1):19–26. https://pubmed.ncbi.nlm.nih.gov/22344492/
13. Hojat M, DeSantis J, Shannon SC, Mortensen LH, Speicher MR, Bragan L, LaNoue M, Calabrese LH. The Jefferson Scale of Empathy: a nationwide study of measurement properties, underlying components, latent variable structure, and national norms in medical students. Advances in Health Sciences Education. 2018;23(5):899–920. https://doi.org/10.1007/s10459-018-9839-9
Crossref PubMed PMC
14. Parra P, Pérez C. Propiedades psicométricas de la escala de compromiso académico, UWES-S (versión abreviada), en estudiantes de psicología. Revista de Educación de Ciencias de la Salud. 2010;7(1),128–133. https://www.researchgate.net/publication/288624459_Propiedades_psicometricas_de_la_escala_de_compromiso_academico_UWES-S_Version_Abreviada_en_estudiantes_de_Psicologia
15. NEJM Catalyst. What is patient-centered care?; 2017. Available from: https://catalyst.nejm.org/doi/full/10.1056/CAT.17.0559
16. Khay-Guan Y. The future of medical education. Singapore Medical Journal. 2019;60(1):3–8. https://doi.org/10.11622/smedj.2019003
Crossref
17. German Rectors’ Conference. The structure of Medical Education in Europe: Implementing Bologna – On the way to a European success story? International Conference hosted by the German Rectors’ Conference (HRK); 2008. Available from: https://www.egms.de/en/meetings/hrk2008/
18. Reis S. Curriculum reform: Why? What? How? and how will we know it works?. Israel Journal of Health Policy Research. 2018;7(1):30. https://doi.org/10.1186/s13584-018-0221-4
Crossref PubMed PMC
19. Lam TP, Lam YY. Medical education reform: the Asian experience. Academic Medicine. 2009;84(9):1313–1317. https://doi.org/10.1097/ACM.0b013e3181b18189
Crossref PubMed
20. Gonnella JS, Callahan CA, Erdmann JB, Veloski JJ, Jafari N, Markle RA, Hojat M. Preparing for the MD: How long, at what cost, and with what outcomes?. Academic Medicine. 2021;96(1):101–107. https://doi.org/10.1097/ACM.0000000000003298
Crossref
21. Reyes H. Acortar los estudios de pre título en Medicina, en Chile: ¿Ahora y para todos?. Revista Médica de Chile. 2016;144(1):7–10. https://doi.org/10.4067/S0034-98872016000100001
Crossref
22. Wilkinson E. Medical students face high levels of mental health problems but stigma stops them getting help. BMJ. 2023;381:p933. https://doi.org/10.1136/bmj.p933
Crossref
23. Nair M, Moss N, Bashir A, Garate D, Thomas D, Fu S, Phu D, Pham C. Mental health trends among medical students. Baylor University Medical Center Proceedings. 2023;36(3):408–410. https://doi.org/10.1080/08998280.2023.2187207
Crossref PubMed PMC
24. Zúñiga D, Torres-Sahli M, Nitsche P, Echeverría G, Pedrals N, Grassi B, Cisternas M, Rigotti A, Bitran M. Reduced burnout and higher mindfulness in medical students after a self-care program during the COVID-19 pandemic. Revista Médica de Chile. 2021;149(6):846–855. https://doi.org/10.4067/s0034-98872021000600846
Crossref
© Education for Health.
Education for Health | Volume 38, No. 4, October-December 2025