Figure 1 Comparing the frequency (%) of students’ scores across the CRI-HT-S indicators
Dipika Bumb1 and Nayanjeet Chaudhury2
1MDS, Doctoral researcher (Public Health), Training Expert, Senior Research Fellow, Ramaiah International Centre for Public Health Innovations, Ramaiah University of Applied Sciences, Bengaluru, India
2MD, MPH, Hon. Consultant, Preventive Healthcare, Sri Sathya Sai Institute of Higher Medical Sciences, Bengaluru, Advisor, Ramaiah International Centre for Public Health Innovations, Bengaluru, India
ABSTRACT
Background: Leadership development is an important part of strengthening Human Resources for Health (HRH) and navigating the complex, dynamic, and interdependent nature of health systems in low- and middle-income countries (LMICs). These health systems are frequently characterized by uncertainty, resource limitations, and fragmented service delivery, necessitating contextually grounded and adaptive leadership on all levels. Despite this, conventional public health staff training programs in LMICs often overlook leadership competencies and fail to incorporate learner-centric, affective, and experiential learning methods. The objective of this review was to synthesise evidence from leadership development initiatives implemented in LMICs to identify common success factors, gaps, and contextual adaptations, and to propose a strategic framework for strengthening leadership capacity among human resources for health (HRH) especially for LMICs.
Methods: This study employed a qualitative thematic synthesis of nine leadership development initiatives implemented across LMICs between 2000 and 2022. Initiatives were selected based on defined inclusion criteria: targeting HRH, reporting contextual adaptation, and including participatory or applied pedagogies. Braun and Clarke’s six-step framework for thematic analysis was applied to extract and synthesize key findings from the selected case studies. Results: Four major cross-cutting themes emerged from the synthesis: (1) contextual relevance and local ownership; (2) adaptive and participatory pedagogies; (3) multi-level stakeholder engagement; and (4) progressive skill development and reflective practice. Based on these findings, we propose a comprehensive strategic approach to leadership development that integrates adult learning theories, blended instructional designs, and adaptive training ecosystems. Emphasis is placed on co-design with stakeholders, including policymakers, healthcare providers, academic institutions, and communities, to ensure relevance and sustainability.
Discussion: Aligning global standards with local contexts, this approach positions leadership development as a central driver for the strengthening of health systems. The paper offers practical recommendations for health system leaders, training institutions, and global health policymakers committed to building resilient and inclusive HRH leadership in LMICs. Drawing on thematic insights from nine leadership initiatives, the study emphasizes the importance of participatory teaching-learning methods, stakeholder engagement, and adaptive training ecosystems.
Key Words: Leadership, HRH, public health, learner-centric, adaptive leadership, training ecosystem, pedagogy, adult learning, LMICs
Date submitted: 3-July-2025
Email: Dipika Bumb (drdipikabumb@gmail.com)
This is an open access journal, and articles are distributed under the terms of the Creative Commons Attribution-Non Commercial-Share Alike 4.0 License, which allows others to remix, tweak, and build upon the work non-commercially, as long as appropriate credit is given and the new creations are licensed under the identical terms.
Citation: Bumb D and Chaudhury N. Building public health leadership capacity in LMICs: lessons from global initiatives for training innovation. Educ Health 2025;38:321-335
Online access: www.educationforhealthjournal.org
DOI: 10.62694/efh.2025.388
Published by The Network: Towards Unity for Health
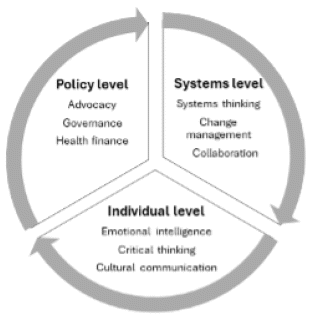
The development of leadership is an evolving, non-linear strategic process (Figure 1), that encompasses competency development1 at the policy,2 systems,3 and individual levels.4 While policy-level competencies shape the macro-environment for systemic improvements, systems-level skills enable efficient functioning within health systems. Individual-level attributes, on the other hand, enhance interpersonal and intrapersonal relationships at the grassroots, thereby fostering trust, inclusivity, and innovation.

Figure 1 Comparing the frequency (%) of students’ scores across the CRI-HT-S indicators
At the policy level, competencies such as policy advocacy5 strategic visioning6 and intersectoral collaboration7 empower leaders to design and implement evidence-based health policies, foster partnerships across sectors, and align with national and global health goals. Policy competencies like governance and health financing8, 9 further enable leaders to ensure transparency, equitable resource allocation, and timely responses to public health emergencies.
At the systems level, it is pertinent to appreciate that health systems are complex, dynamic, self-organizing entities that require constant adaptation to meet evolving needs. The interaction between multiple components defines the functionality at the systems level.5 Leaders can navigate these complex health systems and drive transformative improvements by developing competencies such as systems thinking,3 change management10 and collaboration.11 Leaders with systems-level expertise contribute to strengthening the operational capacities of health systems, thereby improving accessibility, efficiency, and outcomes.
At an individual level, intrapersonal competencies like emotional intelligence,12 cultural competence,13 critical thinking and decision-making,14 and effective communication7 are indispensable for self-growth, creativity,15 and satisfaction at work.16
Learning is an individualized process influenced by individual experiences, cognitive awareness, biases, cultural context, and environment. It results in lasting changes in knowledge and skills, shaped by interactions and lived experiences. Personalized learning approaches cater to unique needs and goals, with technology serving as a key enabler.17 We considered few critical principles from Behaviourism,18 Cognitivism,19 Constructivism,20 alongside the Revised Bloom’s Taxonomy21 and Merrill’s First Principles of Instruction22 to address both the cognitive and affective dimensions of leadership.
Behaviourism lays the groundwork for leadership development by focusing on skills acquisition through structured practice and reinforcement, such as improving communication and decision-making among stakeholders under pressure.18 Cognitivism then builds on this foundation by promoting deeper engagement with complex healthcare problems, encouraging healthcare providers to organize and retain information using techniques like reflective exercises, and concept mapping.19 Robust educational research that encompasses curriculum design, assessment, and learning environments must be grounded in learning theories such as constructivism to enhance validity and alignment with professional outcomes.
Learner-centred methodologies align with constructivist principles that emphasize active meaning making and the social context of learning.20 An integrated curriculum developed by amalgamating the theoretical pedagogical paradigms along instructional designs like Revised Bloom’s Taxonomy21 and Merrill’s First Principles of instruction22 refines the teaching-learning process by complementing learners’ needs. It aids in designing learning objectives, course content and evaluation strategies that encourage a progression from basic recall of leadership concepts to more complex levels of analysis, evaluation, and creation.
The capacity building of healthcare providers in building multi-dimensional leadership competencies involves challenges including training planning, design, and implementation at the state level. One important implementation challenge lies in the delivery of programmatic and non-programmatic trainings for different cadres of Human Resources for Health (HRH). These trainings rely heavily on conventional, teacher-centred pedagogical methods. These approaches are didactic, inflexible and lack real-time feedback systems, hindering self-regulated learning.23 Healthcare providers bring a wealth of experience, and their individual learning needs are linked to their ability to solve complex problems and develop mentorship skills.24 Frenk et al.6 suggests that Health Professionals’ Education (HPE) must move beyond traditional methods and adopt innovative, learner-centered, and integrated pedagogical methods. Other challenges include, but are not limited to, the shortage of staff;25 lack of IT infrastructure for planning and scheduling; limited career development opportunities for public health trainers on modern teaching-learning strategies; and the use of technology that can act as an enabler for working health professionals.
In this paper, we aim to propose a holistic strategic approach for HRH leadership development in public health systems in LMICs, indicated with three foundational pillars. In each pillar, we have incorporated examples of well-researched modalities that support their potential to build effective leadership competencies at the government, community, and provider level.
This review was conducted as part of the author’s doctoral research as part of Ramaiah University of Applied Sciences and was not pre-registered in any database, receiving approval from the Institutional Ethics Committee from the Paster Institute, Shillong, Meghalaya (Approval No. DHSR/ IECPI01/24/05). This approval affirms that the study adheres to the principles outlined in the Declaration of Helsinki and the Indian Council of Medical Research (ICMR) guidelines.
This manuscript adopts a qualitative thematic synthesis approach to review leadership development initiatives in low- and middle-income countries (LMICs). A structured literature search was conducted to identify leadership development initiatives targeting Human Resources for Health (HRH) in LMICs.26–34 The search included both peer-reviewed literature and credible grey literature sources published between 2000 and 2025 in the English language. For this review, “data” referred to all descriptive and evaluative information reported in the included studies regarding the design, delivery, and outcomes of leadership development initiatives in LMICs.
For PubMed, we used combinations of MeSH terms and keywords such as “public health leadership,” “leadership training,” “health workforce development,” “capacity building,” “LMICs,” “HRH,” “adaptive leadership,” “pedagogy,” “adult learning,” “low- and middle-income countries”. Scopus and Web of Science were searched using Boolean operators across titles, abstracts, and keywords. Google Scholar was used to capture grey literature and non-indexed studies, with screening limited to the first 200 results ranked by relevance.
In addition, targeted searches of institutional websites and programs were conducted to capture relevant non-indexed but impactful leadership initiatives. Reference chaining and citation tracking were used to identify additional sources cited in included papers. These initiatives were purposively selected to understand what makes public health leadership development initiatives effective in resource-constrained settings. This was based on the following inclusion criteria: (i) they targeted healthcare providers in LMICs; (ii) they described leadership training or development interventions; (iii) they included information on context, approach, or outcomes; and (iv) they were documented in peer-reviewed sources or institutional reports. Studies were excluded if they lacked outcome data, were purely conceptual, or focused on non-health sectors. The selection aimed for maximum conceptual variation rather than statistical representativeness, consistent with qualitative synthesis methodology.
Thematic analysis of the nine leadership studies followed Braun and Clarke’s six-phase framework.35 The trustworthiness of the synthesis was ensured through iterative coding, peer debriefing, and triangulation across multiple sources. The full texts of the nine studies were read and re-read by two authors to ensure deep familiarity with the content. One author performed open coding on the data, generating initial codes related to program design, pedagogy, and outcomes. These were reviewed by the second author to ensure consistency. A record was maintained for coding decisions and thematic development. The codes were then systematically collated and grouped into potential overarching themes. The authors reviewed these potential themes against the coded extracts and the full dataset to refine them. Detailed descriptions of the study settings, intervention types, and participant groups, are mentioned in Table 1, enabling readers to assess the applicability of findings to other contexts.
Table 1 Thematic analysis of leadership development initiatives implemented in LMICs.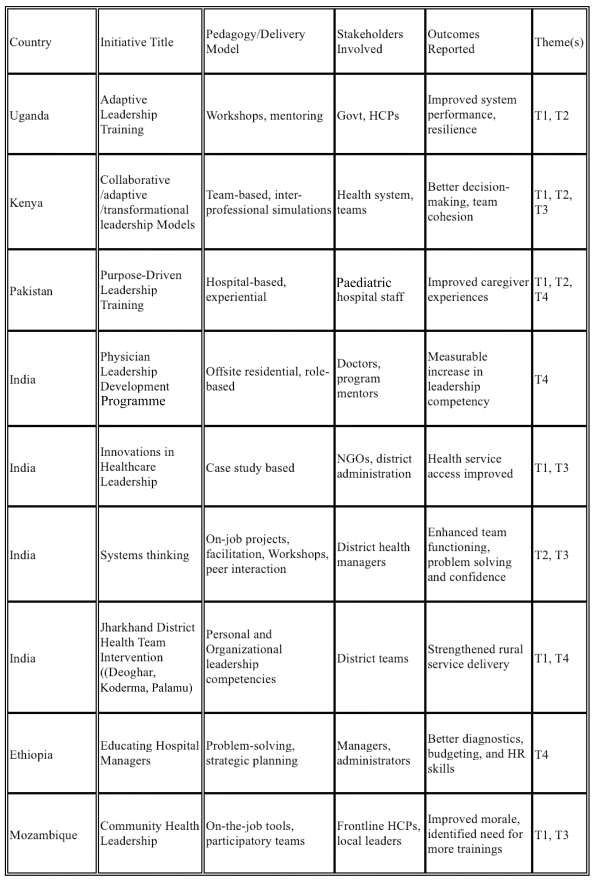
The literature search led to the identification of the nine relevant leadership initiatives across LMICs. 25–34 An initial codebook was developed inductively by reading and re-reading the included studies. Codes were iteratively refined through constant comparison, leading to a final set of 26 codes grouped under the four overarching themes presented in the results. Each included study contributed to one or more codes. Coding was conducted manually by the first author, with periodic peer debriefing by the second author to ensure interpretive consistency. Table 1 maps these contributions, showing the alignment between source studies and thematic categories. The thematic analysis of these initiatives25–34 yielded four recurring themes that represent common success factors in program design, pedagogy, and outcomes.
Programs in India, Pakistan and Mozambique effectively localized content and tailored leadership skills to a service delivery model involving frontline workers (e.g., rural health teams in Jharkhand, VHSNC engagement, family experience of pediatric patients), enabling participants to construct meaning through real-world problem solving in their settings. Contextual grounding allowed learners to apply leadership skills in complex, resource-constrained systems, a key tenet of constructivist learning.
Programs in India, Uganda, Kenya used participatory, case-based learning and on-the-job mentoring. This approach enhanced responsiveness to complex, real-time challenges. Participatory techniques like mentoring, case-based learning, and simulations enabling reflective reasoning and experiential learning were also mentioned by an initiative in Pakistan.28 These strategies allowed healthcare leaders in programs from the above-mentioned countries to process knowledge actively and respond adaptively to real-time system challenges.
Multi-Level Stakeholder Engagement is supported by Behaviorist and Cognitivist principles, where skill-building in stakeholder communication and decision-making are reinforced through repeated practice, feedback, and structured social learning. Collaborative engagement between system actors as seen in studies from India, Pakistan, Kenya, and Rwanda also promoted goal alignment and system thinking, a cognitive function central to leadership behavior change. These programs emphasized integration between government bodies, community leaders, and healthcare providers. This multilevel approach ensured alignment between training content and system priorities.
This theme integrates all three paradigms. Initial leadership skill acquisition is underpinned by Behaviorism (e.g., structured feedback, reinforcement of desired behaviors), while Cognitivism supports higher-order processes such as self-awareness, problem-solving, and strategic thinking. Constructivist elements emerge through mentorship and peer reflection, encouraging participants to synthesize learning through dialogue and practice. Programs from countries like Ethiopia and India employed models that included critical thinking, mentorship, and feedback mechanisms. These programs reported improved self-efficacy and organizational performance.
The thematic heatmap (Figure 2) was generated by mapping the nine leadership development initiatives in LMICs25–34 against the four identified themes, illustrating their relative coverage and highlighting themes that need attention to support an integrated model.
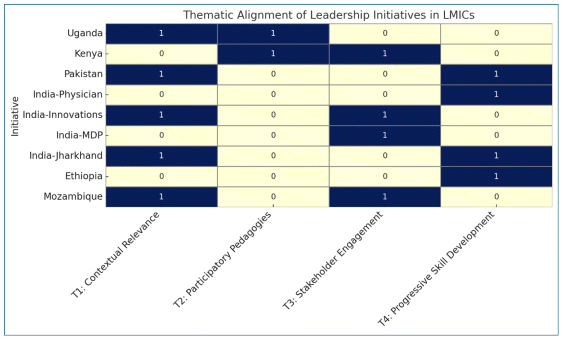
Figure 2 Alignment of leadership initiatives in LMICs with the identified themes.
Notably, no single program addressed all four themes, underscoring significant scope for designing more holistic leadership training models. Among the initiatives, the programs implemented in Jharkhand, India, and Pakistan demonstrated the broadest thematic coverage, addressing three out of the four themes and thus representing more comprehensive approaches to leadership development. In contrast, initiatives like the India-Physician program and India’s Management Development Program (MDP) were more narrowly focused, aligning with only one theme each.
Across the findings, contextual relevance, and local ownership, Theme 1 emerged as the most addressed domain, reflecting a shared recognition that leadership programs must include the social, cultural, and systemic realities of local health systems. However, adaptive, and participatory pedagogies (Theme 2) were less frequently integrated, despite strong global evidence supporting their effectiveness in adult learning and behavior change. Multi-level stakeholder engagement (Theme 3) was moderately present and can be acknowledged as a critical systems enabler, particularly in initiatives involving community or governmental collaboration. Finally, progressive skill development and reflective practice (Theme 4) were inconsistently embedded, even though they are essential for sustaining leadership behavior and fostering organizational learning.
Programs that integrated these themes demonstrated improvements in system responsiveness, frontline confidence, and community involvement. However, no single initiative addressed all four themes comprehensively, signaling the fragmentation and inconsistency of leadership development efforts across LMICs. Figure 3 was developed by synthesizing the thematic gaps identified across the nine initiatives into a unified framework. These findings highlight the fragmented nature of leadership training across LMICs among HRH and the pressing need for integrated, context-sensitive frameworks. These gaps guided the formulation of a three-pronged strategic approach comprising a learner-centric curriculum, an adaptive training ecosystem and multi-stakeholder engagement to address challenges in the current training ecosystems. Its relevance lies in translating evidence into a practical, action-oriented model that policymakers, training institutions, and health leaders can readily apply.

Figure 3 Proposed holistic approach for leadership development among HRH in LMICs
Historically, leadership training often involved top-down, hierarchical approaches, reflecting the colonial legacies and centralized governance structures that prioritized authority and compliance over collaboration and innovation.36 Over the decades, the increasing complexity of health challenges ranging from infectious disease outbreaks37 to the growing burden of non-communicable diseases has necessitated a shift towards more adaptive, participatory, and inclusive leadership models. This transformation has been driven by globalization, advancements in technology, and the recognition of health as a fundamental human right.38 These changes in the concept of leadership from an inherent skill to a transferrable skill demands the application of a unified approach incorporating pedagogical theoretical paradigms and adult learning principles blended with instructional designs. Together, these linkages validate the theoretical robustness of the integrated leadership curriculum. By mapping themes to Bloom’s Taxonomy and Merrill’s First Principles, the findings demonstrate how instructional design, theory-driven pedagogy, and context-specific adaptation synergize to promote leadership capacity among public health providers in LMICs.
A relevant example of this approach is India’s Mission Karmayogi 2020, an initiative aimed at enhancing the capacity of civil servants through a technology-driven, flexible, and lifelong learning approach that follows a 70-20-10 system.39 This emphasis on role-based leadership provides a strong opportunity to tailor leadership training to the specific needs of HCPs, ensuring the curriculum is relevant to their daily responsibilities and challenges.
The ability to adapt to change is the hallmark of a good leader and organization; however, a change in any system faces an initial resistance to non-traditional methods, whether it is the implementation of a new protocol for maternal health or a policy change at the state level. This could be an opportunity to gradually introduce and normalize innovative practices, such as interactive learning, mentorship, and self-directed education, in a way that respects cultural norms.40 In high-context cultures in LMICs where communities prefer indirect communication and relationships over other aspects, leadership training should emphasize collaborative learning and peer support, thus aligning with local values of social harmony and respect.41
An additional approach to reduce the high workload on healthcare providers is to design flexible and modular training programs that will be incorporated within their daily work activities. This would allow HCPs to continue to develop leadership skills without overwhelming their schedules. An adaptive learning ecosystem emphasizes personalized or group continuous learning, real-time feedback, technology use for improving efficiency and effectiveness in contemporary health professional training42. Figure 4 illustrates how common barriers and resource limitations, can also present opportunities for innovation. This reframing reinforces the adaptive ethos of the proposed training ecosystem.23,25,40–42
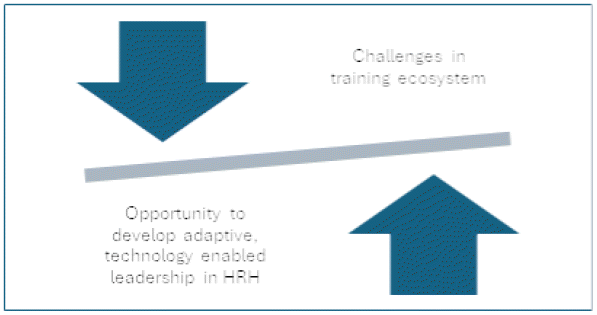
Figure 4 The relationship between challenges and opportunities for leadership development in the training ecosystem.
As mentioned earlier, healthcare is a complex adaptive system. It demands multi-sectoral and multi-disciplinary collaboration between different stakeholders as a key driver to foster leadership at all levels that leads to the fulfilment of shared goals both at individual and organizational levels.43 The varying cultural, economic, and political landscapes in LMICs necessitate a more nuanced approach to ensure relevance and applicability while recognizing the diversity of socio-political contexts and tailoring the strategies accordingly.
For example, in India, the National Health Mission (NHM), which is a flagship program that aims to improve healthcare delivery across rural and underserved regions, primarily focuses on multi-stakeholder engagement between the central and state governments, healthcare providers, and community leaders. One of the key components of the NHM is the Village Health Sanitation and Nutrition Committees (VHSNCs), which bring together local community members, healthcare workers, and government officials to take part in health planning, monitoring, and decision-making.44
Similarly, in Kenya, an initiative emphasized role-based leadership to ensure that healthcare professionals can effectively manage local health challenges effectively by engaging with the Ministry of Health, healthcare providers, and community leaders.45 Ethiopia’s Health Extension Program (HEP) brings together the government, healthcare workers, and local communities to strengthen primary healthcare delivery in rural areas.46 The active involvement of local stakeholders in leadership training ensures that healthcare providers are prepared to address the unique needs of their communities.
In Rwanda, the Health System Strengthening Project leveraged collaboration between the government, international partners, and local health leaders to enhance the leadership capabilities of healthcare providers at all levels. This multi-stakeholder engagement ensured leadership development is responsive to national health policies and local healthcare delivery.47
These examples demonstrate a collaborative approach and the importance of buy-in from stakeholders of all disciplines for transformative changes in the health systems. Briefly, in LMICs where resources, infrastructure, and healthcare priorities vary widely, a flexible training ecosystem and leadership program allows for context-specific adaptations and tailored learning experience, ensuring that training programs are both relevant and practical via stakeholder collaboration. This gives an opportunity to leverage global best practices enhancement while allowing for local customization. Combining these three elements into a cohesive strategy may enhance the leadership among human resources to lay the foundation of a resilient, inclusive, and accountable health systems.
This integrated approach aims to shift health leadership from a top-down directive model to one that is co-owned, embedded within communities, and sustained through continuous learning.
This manuscript contributes to a growing body of evidence that advocates for contextually adaptive leadership development strategies in LMICs. The thematic analysis of nine diverse leadership initiatives underscores critical gaps and enablers in designing effective programs for Human Resources for Health (HRH). The findings reiterate that leadership development cannot remain a peripheral or one-size-fits-all intervention; this must be proposed as a core, strategic lever for strengthening health systems, one that aligns with local realities, fosters multi-level engagement, and is embedded within adaptive learning ecosystems.
Our proposed three-pronged strategy offers a composite response to these issues. WHO-ASPHER (2020) calls for system-wide leadership competencies that include stakeholder collaboration, communication, and ethical reasoning.48 Doci et al. emphasized that focusing on leaders’ cognitive processes enhances leadership training and leads to sustained improvements in behavior. This cognitive approach aligns with constructivist principles, which promote active, hands-on engagement with real-world challenges.49 Learners collaborate and solve problems through simulations and case-based exercises, accelerating their leadership development. Baker et al. demonstrated that a constructivist-based leadership development program significantly improved participants’ leadership skills, self-awareness, and ability to cultivate collaborative environments.50
Similarly, Zulfiqar et al. applied Bloom’s taxonomy to assess leadership awareness in university leaders and found that structured leadership training significantly increased their ability to articulate a vision, model effective behavior, and foster collective goals.51 Badali et al. further reported that using Merrill’s principles of instruction in a MOOC (Massive Online Open Course) significantly enhanced participants’ learning outcomes and satisfaction compared to traditional methods.52 Furthermore, recognizing mentorship as a complex adaptive system and integrating it into longitudinal learning cycles supports the ecosystem approach outlined in this paper.53 Similarly, Learning Health Systems are proposed as sustainable mechanisms to bridge evidence-based practice and continuous professional development, by using suitable mentoring models, integrating digital infrastructure, and providing real-time feedback.54 Archisman et al, has systematically presented the other health research and health care provider-related leadership workshops and short-term programs undertaken at different locations in India.55
The COVID-19 pandemic has revealed the power of digital learning globally, accelerating a paradigm shift in how health professionals acquire and apply new competencies, making learning accessible anytime and anywhere. This unprecedented disruption spurred the rapid development and scaling of platforms driven not only by private entrepreneurial ventures but also by national and sub-national public sector initiatives, enabling primary healthcare systems to integrate technology-enabled, role-aligned, and flexible capacity-building models.
The WHO Academy offers multilingual, open-access courses that have reached millions of learners worldwide, including frontline health workers in LMICs, Project ECHO’s tele mentoring model56 builds communities of practice that improve provider capability and, in several settings, patient outcomes. These platforms directly contribute to an adaptive training ecosystem by offering asynchronous and self-paced learning, localization of content to meet regional health priorities, and scalability. Their microlearning modules, peer-learning forums, and embedded feedback mechanisms align with the ecosystem’s emphasis on continuous, iterative improvement and learner autonomy. These exemplars illustrate how digital continuing professional development can stitch together the cognitive, affective, and behavioral dimensions of leadership through case-based sessions, reflective prompts, and feedback.
The authors acknowledge the challenges involved in generalizing the proposed strategies across diverse socio-political contexts, particularly within LMICs. Implementing these strategies often faces hurdles such as resource limitations, resistance to change, and threats to sustainability. To address these barriers, implementers must adopt a phased rollout approach, engage stakeholders early to foster collaboration and buy-in, and invest in capacity-building initiatives that strengthen the human and institutional resources necessary for success (Figure 5). This image was created after studying the references to showcase the interaction between the training ecosystem and the leadership development program, emphasizing that effective leadership capacity-building functions within a dynamic feedback loop. This interplay ensures that training content, delivery methods, and evaluation processes remain responsive to system needs, thereby reinforcing both program sustainability and health system performance.

Figure 5 Interaction between the training ecosystem and the leadership development program.
By proactively managing these elements, health systems can improve the feasibility and long-term sustainability of leadership development strategies. Equally important is the integration of continuous monitoring and feedback mechanisms, which play a critical role in ensuring that leadership programs achieve their intended outcomes.
Despite its importance, tracking long-term results remains challenging in LMIC settings due to socio-political and financial variability. A robust M&E system is critical for nurturing a strong group of leaders prepared for future public health challenges. Future efforts must embed flexible, iterative monitoring and evaluation (M&E) frameworks into program design from the outset. These frameworks must include clearly defined methods to assess leadership competencies at individual, organizational, and systemic levels, while also tracking related incremental improvements in health outcomes.
This framework is more than a training model; it is a shared vision for strengthening leadership at every level of the health system. Grounded in equity, adaptability, and local ownership, it re-emphasizes the goals of WHO’s Workforce 2030 and the Sustainable Development Goals, particularly SDG 3’s call for healthier lives, SDG 4’s focus on lifelong learning, and SDG 17’s emphasis on partnerships. Its design allows for flexible adaptation, making it as relevant in an LMIC setting as in a national training institute. By creating space for South–South learning collaborations, the approach enables developing countries facing similar workforce challenges to share innovations, adapt solutions, and build collective capacity for change.
At its core, this framework is about resilience not as a static trait, but as a leadership skill that can be taught, practiced, and embedded in the culture of health systems via digital learning, participatory methods, and multi-stakeholder engagement. This coherent strategy offers LMICs a pathway to leapfrog traditional training bottlenecks, ensuring that no cadre, no community, and no patient is left behind in the pursuit of stronger public health leadership.
1. Strudsholm T, Vollman AR. Public health leadership: Competencies to guide practice. Healthcare Management Forum. 2021;34(6):304–356. https://doi.org/10.1177/08404704211032710
Crossref
2. Doshmangir L, Sakha MA, Mostafavi H, et al. Essential core competencies for health policy graduates: A multi-method consensus study. Health Research Policy and Systems. 2024; 22:136. https://doi.org/10.1186/s12961-024-01221-8
Crossref
3. Czabanowska K. Leadership in public health. Eurohealth. 2020;26(2):25–29
4. Rocco ML, Davis KR. Expanding the boundaries of leadership development: Propositions for leadership educators. New Directions for Student Leadership. 2024; 183:51–58. https://doi.org/10.1002/yd.20623
Crossref
5. Paina L, Peters DH. Understanding pathways for scaling up health services through the lens of complex adaptive systems. Health Policy and Planning. 2012;27(5):365–373. https://doi.org/10.1093/heapol/czr054
Crossref
6. Frenk J, Chen L, Bhutta ZA, Cohen J, Crisp N, Evans T, Zurayk H. Health professionals for a new century: Transforming education to strengthen health systems in an interdependent world. The Lancet. 2010;376(9756):1923–1958. https://doi.org/10.1016/S0140-6736(10)61854-5
Crossref
7. El-Jardali F, Fadlallah R. A systems thinking approach to inform policy decisions for health systems strengthening: An analytical framework for country-level application. Health Research Policy and Systems. 2018;16(1):1–8. https://doi.org/10.1186/s12961-018-0327-z
8. Roberts MJ, Hsiao W, Berman P, Reich MR. Getting health reform right: A guide to improving performance and equity. Oxford: Oxford University Press; 2008. https://doi.org/10.1093/acprof:oso/9780195371505.001.0001
Crossref
9. Shrestha P, Burns C, Russell DJ. Leadership in health care crisis management: Challenges and opportunities. Journal of Health Management. 2021;23(4):563–577. https://doi.org/10.1177/09720634211050394
10. Kotter JP. 8-Step Process for Leading Change [Internet]. Kotter Inc. Available from: https://www.kotterinc.com/methodology/8-steps/
11. Zia ud Din M, Yuan X, Ullah Khan N. The impact of public leadership on collaborative administration and public health delivery. BMC Health Services Research. 2024; 24:129. https://doi.org/10.1186/s12913-023-10537-0
Crossref PubMed PMC
12. Goleman D. Emotional Intelligence: Why It Can Matter More Than IQ. New York: Bantam Books; 1998
13. Betancourt JR, Green AR, Carrillo JE, Ananeh-Firempong O. Defining cultural competence: a practical framework for addressing racial/ethnic disparities in health and health care. Public Health Reports. 2003;118(4):293–302. https://doi.org/10.1093/phr/118.4.293
Crossref PubMed PMC
14. Facione PA. Critical Thinking: What It Is and Why It Counts. Millbrae, CA: Insight Assessment; 2011
15. Amabile TM, Kramer S. The Progress Principle: Using Small Wins to Ignite Joy, Engagement, and Creativity at Work. Boston: Harvard Business Press; 2011
16. Mosadeghrad AM, Ferdosi M. Leadership, job satisfaction and organizational commitment in healthcare sector: proposing and testing a model. Materia Socio-Medica. 2013;25(2):121–126. https://doi.org/10.5455/msm.2013.25.121-126
Crossref PubMed PMC
17. Shemshack A, Spector JM. A systematic literature review of personalized learning terms. Smart Learning Environments. 2020; 7:33. https://doi.org/10.1186/s40561-020-00140-9
Crossref
18. Skinner BF. Science and Human Behavior. New York: Macmillan; 1953
19. Pakpahan FH, Saragih M. Theory of cognitive development by Jean Piaget. Journal of Applied Linguistics. 2022;2(2):55
Crossref
20. Dongre A, Pandya H. Navigating complexities: Improving evidence quality in Indian medical education research. Global Journal of Health Sciences and Research. 2025; 3:1–5. https://doi.org/10.25259/GJHSR_30_2025
Crossref
21. Anderson LW, Krathwohl DR, editors. A taxonomy for learning, teaching, and assessing: A revision of Bloom’s taxonomy of educational objectives. New York: Longman; 2001
22. Merrill MD. First principles of instruction. Educational Technology Research Development. 2002; 50:43–59. https://doi.org/10.1007/BF02505024
Crossref
23. Matsuyama Y, Nakaya M, Okazaki H, et al. Does changing from a teacher-centered to a learner-centered context promote self-regulated learning: a qualitative study in a Japanese undergraduate setting. BMC Medical Education. 2019; 19:152. https://doi.org/10.1186/s12909-019-1550-x
Crossref PubMed PMC
24. Rodríguez DC, Jessani NS, Zunt J, Ardila-Gómez S, Muwanguzi PA, Atanga SN, Sunguya B, Farquhar C, Nasuuna E. Experiential learning and mentorship in global health leadership programs: Capturing lessons from across the globe. Annals of Global Health. 2021;87(1):61. https://doi.org/10.5334/aogh.3194
Crossref PubMed PMC
25. Nwankwo ONO, Auer C, Oyo-Ita A, Eyers J, Wyss K, Fink G, Bosch-Capblanch X. Human resources for health: A framework synthesis to put health workers at the centre of healthcare. BMJ Global Health. 2024;9: e014556
Crossref PubMed PMC
26. Nakanjako, D., Namagala, E., Semeere, A. et al. Global health leadership training in resource-limited settings: a collaborative approach by academic institutions and local health care programs in Uganda. Human Resources for Health 2015;13: 87. https://doi.org/10.1186/s12960-015-0087-2
Crossref PubMed PMC
27. Chelagat TK, Rice J, Onyango J, Kokwaro G. An assessment of impact of leadership training on health system performance in selected counties in Kenya. Front Public Health. 2021 Feb 25; 8:550796. https://doi.org/10.3389/fpubh.2020.550796. PMID:33681150; PMCID:PMC7956995
Crossref PubMed PMC
28. Rasheed MA, Hussain A, Hashwani A, Kedzierski JT, Hasan BS. Implementation evaluation of a leadership development intervention for improved family experience in a private paediatric care hospital, Pakistan. BMC Health Services Research. 2022; 22:954. https://doi.org/10.1186/s12913-022-08342-2
Crossref
29. Gulati K, Singh AR, Kumar S, Verma V, Gupta SK, Sarkar C. Impact of a leadership development programme for physicians in India. Leadership in Health Services. 2020;33(1):73–84. https://doi.org/10.1108/LHS-05-2019-0027
30. Pathak M, Bansal K. Leadership innovations in healthcare: a case study of transformative strategies in Madhubani, Bihar. International Journal of Novel Research Development. 2024 Feb;9(2): b455–b460. Available from: https://ijnrd.org/viewpaperforall.php?paper=IJNRD2402158
31. Prashanth NS, Marchal B, Devadasan N, Singh R, Goicolea I, Kegels G, et al. Advancing the application of systems thinking in health: a realist evaluation of a capacity building programme for district managers in Tumkur, India. Health Research Policy and Systems. 2014;12:42. doi:10.1186/1478-4505-12-42
Crossref PubMed PMC
32. Kumar A, Satia JK. Rural health innovation through leadership development and organizational effectiveness. Jharkhand Journal of Sociology Development. 2010;3(2):1–15. https://www.researchgate.net/publication/228195942_Rural_Health_Innovation_through_Leadership_Development_and_Organisational_Effectiveness
33. Kebede S, Abebe Y, Wolde M, Bekele B, Mantopoulos J, Bradley EH. Educating leaders in hospital management: a new model in Sub-Saharan Africa. International Journal for Quality in Health Care. 2010;22(1):39–43. https://doi.org/10.1093/intqhc/mzp051
Crossref
34. Perry C. Empowering primary care workers to improve health services: results from Mozambique’s leadership and management development program. Human Resources for Health. 2008; 6:14. https://doi.org/10.1186/1478-4491-6-14
Crossref
35. Braun V, Clarke V. Using thematic analysis in psychology. Qualitative Research in Psychology. 2006;3(2):77–101. https://doi.org/10.1191/1478088706qp063oa
Crossref
36. Smith K, Bhavsar M. A new era of health leadership. Healthcare Management Forum. 2021;34(6):332–335. https://doi.org/10.1177/08404704211040817
Crossref PubMed PMC
37. World Health Organization. Retention of the health workforce in rural and remote areas: A systematic review. Human Resources for Health Observer Series. 2020;(25). Geneva: WHO. https://www.who.int/news/item/08-12-2020-retention-of-the-health-workforce-in-rural-and-remote-areas-a-systematic-review
38. Holst J. Global Health – emergence, hegemonic trends and biomedical reductionism. Global Health. 2020;16(1):42. https://doi.org/10.1186/s12992-020-00573-4
Crossref PubMed PMC
39. Mission Karmayogi. [Internet]. 2020 [cited 2025 Feb 21]. Available from: https://karmayogibharat.gov.in/programme.php
40. Sharma N, Doherty I, Dong C. Adaptive learning in medical education: The final piece of technology enhanced learning? Ulster Medical Journal. 2017;86(3):198–200. PMID: 29581634; PMCID: PMC5849979
PubMed PMC
41. Atwater L, Yu J, Tawse A, et al. Relevance of culture in studies of leadership: ignored or dismissed? Asia Pacific Journal of Management. 2021; 38:687–708. https://doi.org/10.1007/s10490-019-09678-w
Crossref
42. Plooy E, Casteleijn D, Franzsen D. Personalized adaptive learning in higher education: A scoping review of key characteristics and impact on academic performance and engagement. Heliyon. 2024;10(21): e39630. https://doi.org/10.1016/j.heliyon.2024.e39630
Crossref PubMed PMC
43. Smith K, Bhavsar M. A new era of health leadership. Healthcare Management Forum. 2021;34(6):332–335. https://doi.org/10.1177/08404704211040817
Crossref PubMed PMC
44. National Health Mission (NHM). [Internet]. [cited 2025 Feb 21]. Available from: https://mohfw.gov.in/sites/default/files/56987532145632566578.pdf
45. USAID. Kenya Health Systems Strengthening. [Internet]. [cited 2025 Feb 21]. Available from: https://www.usaid.gov/sites/default/files/2022-05/Health_Systems_Strengthening_fact_sheet.pdf
46. Haileamlak A, Ataro I. The Ethiopian Health Extension Program (HEP) is still relevant after 15 years of implementation although major transformation is essential to sustain its gains and relevance. Ethiopian Journal of Health Sciences. 2023;33 (Spec Iss 1):1–2. https://doi.org/10.4314/ejhs.v33i1.1S. PMID:38362471
PubMed
47. Bonds MH, Rich ML. Integrated health system strengthening can generate rapid population impacts that can be replicated: lessons from Rwanda to Madagascar. BMJ Global Health. 2018;3: e000976. https://www.pivotworks.org/publications/integrated-health-system-strengthening-can-generate-rapid-population-impacts-that-can-be-replicated-lessons-from-rwanda-to-madagascar/
Crossref PubMed PMC
48. Czabanowska K, Shickle D, Burazeri G, Gershuni O, Otok R, Azzopardi Muscat N; World Health Organization Regional Office for Europe; Association of Schools of Public Health in the European Region. WHO–ASPHER Competency Framework for the Public Health Workforce in the European Region. Copenhagen: WHO Regional Office for Europe; 2020. 73 p. Available from: https://apps.who.int/iris/bitstream/handle/10665/347866/WHO-EURO-2020-3997-43756-61569-eng.pdf(Accessed 2025 Jul 3)
49. Dóci E, Stouten J, Hofmans J. The cognitive-behavioral system of leadership: cognitive antecedents of active and passive leadership behaviors. Frontiers in Psychology. 2015; 6:1344. doi:10.3389/fpsyg.2015.01344
Crossref PMC
50. Baker JD, Smith SM, Brown RL. Constructivist leadership development: A case study of a leadership program in higher education. Journal of Leadership Education. 2020;19(3):45–62
51. Zulfqar A, Valcke M, Quraishi U, Devos G. Developing academic leaders: Evaluation of a leadership development intervention in higher education. SAGE Open. 2021;11(1). https://doi.org/10.1177/2158244021991815
Crossref
52. Badali M, Hatami J, Farrokhnia M, Noroozi O. The effects of using Merrill’s first principles of instruction on learning and satisfaction in MOOC. Innovations in Education and Teaching International. 2020;59(2):216–225. https://doi.org/10.1080/14703297.2020.1813187
Crossref
53. Teo MYK, Ibrahim H, Lin CKR, et al. Mentoring as a complex adaptive system – a systematic scoping review of prevailing mentoring theories in medical education. BMC Medical Education. 2024; 24:726. https://doi.org/10.1186/s12909-024-05707-5
Crossref
54. Rajit D, Johnson A, Callander E, et al. Learning health systems and evidence ecosystems: A perspective on the future of evidence-based medicine and evidence-based guideline development. Health Research Policy and Systems. 2024;22(1):4. https://doi.org/10.1186/s12961-023-01095-2
Crossref PubMed PMC
55. Mohapatra A, Kaur J, Mukherjee R, Aravind RS, Deshmukh V, Bassi S, Swain S, Wig R, Kumar S, Arora NK. An exploratory-descriptive analysis of training programs for leadership in health research and services in India. Indian Journal of Public Health. 2024 Apr–Jun;68(2):243–50. https://doi.org/10.4103/ijph.ijph_762_23
Crossref PubMed
56.Arora S, Kalishman SG, Thornton KA, Komaromy MS, Katzman JG, Struminger BB, Rayburn WF, Bradford AM. Project ECHO: A Telementoring Network Model for Continuing Professional Development. J Contin Educ Health Prof. 2017 Fall;37(4):239–244. doi: 10.1097/CEH.0000000000000172. Erratum in: J Contin Educ Health Prof. 2018 Winter;38(1):78. https://doi.org/10.1097/CEH.0000000000000192
Crossref PubMed
© Education for Health.
Education for Health | Volume 38, No. 4, October-December 2025