
Laura Bauler1 and Wilo Issack2
1PhD, Associate Professor, Department of Biomedical Sciences, Western Michigan University Homer Stryker MD School of Medicine, Kalamazoo, United States
2MD, PGY1 Resident, Department of Medicine, Western Michigan University Homer Stryker MD School of Medicine, Kalamazoo, United States
ABSTRACT
Background: There are gender disparities for women in medicine, with poorer health outcomes and decreased representation in the physician workforce. While many solutions have been proposed, the unconscious bias that perpetuates these disparities is hard to change. In this study, we examined the impact of an educational intervention focused on the history of women’s rights in the United States, on students’ knowledge, perceptions, and attitudes towards women’s rights. The educational intervention was designed using critical theory to improve student knowledge of the social and historical contexts that have led to gender disparities, promoting critical reflection of beliefs in an attempt to modify student attitudes towards women’s rights. We hypothesized that men and women would respond differently to this educational intervention, based on their prior knowledge, experiences, and beliefs.
Methods: The knowledge and attitudes of 159 allopathic medical students were measured between 2023–2024 using a pre- and post-survey to assess the impact of participating in a modified jigsaw educational intervention on gender bias.
Results: Students identifying as women had more formal education or experiences with women’s reproductive rights compared to students identifying as men. On average, students showed improved knowledge, answering 4.94 questions correctly on the pre-survey compared to 8.65 questions on the post-survey (p <0.001); however, women began with a higher knowledge level than men. Finally, student attitudes, as measured by agreement with statements, also changed post-intervention, and written statements indicated students’ desire to advocate for women.
Discussion: This study shows that a single educational intervention can impact students’ short-term knowledge and attitudes toward women’s rights, which is the first step towards creating agency in students to mitigate the gender biases seen in medicine.
Key Words: Gender equity, sexism, marginalized, women, gender gap, workforce diversity
Date submitted: 26-July-2025
Email: Laura Bauler (laura.bauler@wmed.edu)
This is an open access journal, and articles are distributed under the terms of the Creative Commons Attribution-Non Commercial-Share Alike 4.0 License, which allows others to remix, tweak, and build upon the work non-commercially, as long as appropriate credit is given and the new creations are licensed under the identical terms.
Citation: Bauler L and Issack W. Limiting gender bias in medicine by improving student knowledge and attitudes. Educ Health 2025;38:392-403
Online access: www.educationforhealthjournal.org
DOI: 10.62694/efh.2025.445
Published by The Network: Towards Unity for Health
Gender disparities have long been a part of our global human history, and the impacts can be seen at every level of society, from leadership to education and even healthcare outcomes.1,2 In the United States, despite having fought for women’s rights over the last century, with legal rights battles in the 1920s, to the women’s rights movements of the 1960s and 70s, women continue to have reduced autonomy over their lives and bodies compared to men.3 Historically, there have been many limitations to women’s bodily autonomy, including forced sterilization, limited control over reproductive choices, and limited ability to participate in health research.4 Together, these inequities have led to increased suffering for women with health conditions that, with more knowledge of female bodies, could be treated.5 Historically, a person’s sex and gender were used interchangeably, however current social norms recognize intersectionality, which separates a person’s biological sex from their gender. In this study, the terms female and male are used to refer to an individual’s biological sex, while the terms woman and man are used to indicate a person’s gender. Both female biological sex and people who identify as women have been shown to be at increased risk for disparities.1,2
Significant differences in physiology, anatomy, genetics, and hormones exist between females and males that define their health, disease presentation, and medication efficacy.6,7 The medical field has historically failed to acknowledge sex differences, utilizing the male body as the “standard” human in medical research studies.6 Therefore, the healthcare interventions developed and delivered to patients are not reflective of these biological sex differences and result in health disparities for females.
The recent emphasis of the healthcare differences by sex and gender can be attributed to the growing number of women entering the medical and research fields; however, challenges exist that limit women’s career success.8 In the US, despite recent increases in women medical trainees reaching or just exceeding 50% in 2023, there are fewer practicing women physicians (~45% full time faculty) compared to men, similar trends are seen across the world.9,10 Women physicians encounter more obstacles than men colleagues, including a lack of mentorship, minimal leadership positions, and limited educational opportunities.1,11 Gender concordance between patient and provider is especially important for improving health outcomes when treating gendered conditions (gynecologic/breast cancer)12–15. Women frequently initiate discussions regarding gender disparity; however, due to their limited representation in leadership roles, their influence and impact on this issue often remain minimal.7,16
While the studies described above have documented gender bias in healthcare outcomes and the medical workforce, few studies have proposed strategies to mitigate these biases. Current medical education has minimal (if any) curricula that address gender biases and sex differences.16–19 The implementation of microaggression training and gender education into medical education can reduce gender-biased attitudes in individuals.20–22 Thus, we hypothesize that educating future medical providers about gender biases may reduce gender bias, and improve future interactions with colleagues and patients alike. The educational pedagogy, critical theory, supports this developmental progression. This teaching philosophy empowers students to be co-participants in the learning process to recognize and examine the institutional inequities that have led to marginalization of certain populations.23,24 Students learn from and with each other to critically evaluate commonly accepted assumptions, identify hidden power structures and patterns of inequity, and challenge their own beliefs.24
In this study, second-year medical students were provided with an educational intervention grounded in critical theory to learn about pre-selected historical events dealing with women’s reproductive rights. We hypothesized that student gender would impact the knowledge perceptions/attitudes, and ultimately behaviors/actions gained following this educational intervention. This comparison by gender is important, as it exposes the differences that may exist in the impact on students from education efforts to reduce gender bias. Exposing students to the existing gender differences and biases found in medicine early in their medical careers could positively influence their views, leading to an improvement in their interactions with future patients and colleagues.
This study was conducted at a Midwest allopathic medical school in the health system science course over a 2-year period (2023 to 2024); learners were second-year medical students. The University’s institutional review board exempted this study (2024-1189). This study uses a mixed methods approach to evaluate quantitative changes in student knowledge and agreement with attitudinal and perception statements, as well as qualitative analysis of free-text responses provided by students. The learning activity was structured using a modified jigsaw methodology, a collaborative learning strategy where students become experts on a topic in small groups and then share their knowledge with the larger group.25 Students individually completed the pre-survey. They then worked in small groups to research pre-defined historical events focused on women’s reproductive health. Each group then presented its findings to the whole class, and a timeline of U.S. historical events that have shaped the current landscape of women’s reproductive health was assembled. Following the student presentations, a whole-class discussion was facilitated by faculty with expertise in ethics and law, giving some of the topics more in-depth attention, highlighting common themes, and addressing any student questions. Following this discussion, students individually completed the post-survey.
Student knowledge, perceptions and attitudes were measured using a pre-event and post-event survey. The post-survey also included questions to evaluate the event. Pre- and post-surveys were anonymous but were linked using a student-defined code. In the pre-survey we collected student demographic information including gender (man, woman, transgender, other), geographical state of upbringing, age, and race; as well as any prior exposure to the content. All variables were categorical to protect student anonymity. Using a 6 point-Likert scale of agreement, students were asked their level of agreement with 8 gender-related experiences statements (pre-survey), 7 knowledge-based statements (4- pre and post and 3- post only), and 7 attitudinal statements (5-pre and post, 2- post only). Six of the eight experience items (indicated by * in the Tables) were adapted from a psychometric evaluation study by Parker et al.26 Eleven multiple choice knowledge questions were posed in the pre- and post-surveys to explore changes in student understanding of the content. The post-survey also contained an open-ended question asking students to “describe at least one aspect of the activity that was beneficial to their learning”. The pre- and post-surveys were piloted by a small group of students and faculty prior to their dissemination but knowledge questions were not validated prior to use.
Quantitative data were analyzed using descriptive statistics (frequencies and percentages). The student-reported gender-stratified data, and comparisons between women and men or pre- and post-data were conducted using a Student’s t-test or Mann-Whitney U test with an alpha of 0.05. To account for multiple comparisons, Bonferroni correction was used, dividing the conventional alpha level of 0.05 by the number of tests conducted, limiting the likelihood of Type I errors. Cohen’s d was used to measure the effect size of each statistically significant comparison. In cases where proportions were compared, a z-test was used for comparison. Only three individuals in the cohort reported being “transgender” (n=1), or “other” (n=2), these students were included in the overall analysis but not in subgroup analysis. In subgroups with less than 10 individuals it may be possible to identify individuals based on their responses and these small subgroups are unlikely to show meaningful differences, thus were not reported in this study. For qualitative data, free-text responses were analyzed using an inductive thematic analysis. Using an iterative process, common themes were identified, refined, and each response was sorted into one or more categories. Quotes were selected that best illustrate the themes.
In total, 159 students participated in the study; 57.2% were women, and 40.9% were men. Three students did not use their defined code when completing the post-survey, leaving 156 students for paired pre-post analysis. The students in these cohorts came from 25 different states across the US, with an average age of 24.8 years (21–38 range). On average, 18.5% of students were from underrepresented groups in medicine. In total, 13.2% of students previously had formal education in women’s health, and of those, 8.8% were women and 4.4% were men. Students were asked if they had personal knowledge of someone (self/family/friend) who had a challenging experience with women’s health; 53.4% indicated they did, with the majority of those responses coming from women (Table 1).
Table 1 Participant Demographics
To understand if there were differences in student perceptions of women’s health topics by gender, students were asked a series of questions about their lived experiences, observations, and awareness of the impacts of gender on healthcare. Overall, students agreed that medical education and medical knowledge are skewed toward favoring men. Most students agreed they have observed and encountered gender-biased attitudes and behaviors both among peers and in clinical settings. When asked if their gender impacted how faculty evaluated their performance, most students disagreed. When data were stratified by gender, the difference between women’s and men’s responses was statistically significant for most statements, with women more strongly agreeing than men (Table 2). Overall, the patterns seen here are an important indicator of how much gender impacts our experiences and perceptions. Taken together, this data suggests that there is a bias in student perceptions about gendered topics in medicine, with women observing these gendered biases at a much higher rate than men.
Table 2 Students’ Lived Experiences and Awareness about Gender in Healthcare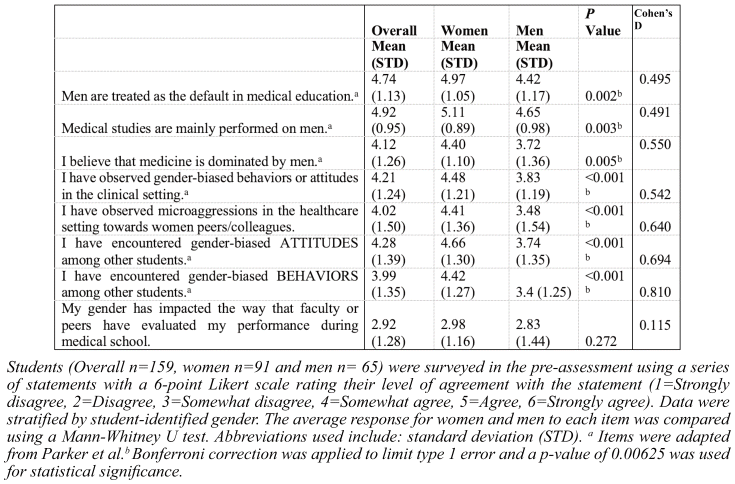
To determine if student perceptions can be impacted by increasing their knowledge, an educational intervention was designed to teach students about historical events that have impacted the current climate surrounding women’s reproductive health. We hypothesized that increasing students’ knowledge would affect their perceptions and attitudes, potentially influencing their behavior, and that this would occur differentially by gender. Only knowledge and attitudes were measured in this study.
Students’ knowledge about historical events related to women’s reproductive health were compared pre- and post-intervention with an 11-item assessment. Overall, student knowledge improved from a score of 4.94 to 8.65 questions correct on average (p <0.001). The average scores of women (5.18 to 8.94, p <0.001) were slightly higher than those of men (4.61 to 8.27, p <0.001), but both groups showed a statistically significant increase in knowledge. Student agreement with four pre-post knowledge statements showed a statistically significant improvement for three statements; women started and ended with higher levels of agreement than men, but both groups showed significant improvement in knowledge. Finally, a majority of students indicated that they agree, or strongly agree, that their understanding of women’s reproductive rights increased following the event (Table 3). Women were significantly more likely to agree than men that they wanted to learn more about women’s reproductive justice. This same trend was also seen in responses to the open-ended question of “describe one aspect of this activity that was beneficial to your learning” free-text comments provided by students(98%, n=153/156), where a majority of students (50%, n=76 of the 153 comments) indicated increased knowledge on the various topics covered was most beneficial to them following the event. Quotes are provided below to highlight this trend.
Table 3 Student Agreement with Knowledge Statements Relating to Women’s Reproductive Rights
“It was beneficial to gain an overview of the historical context that has led to today’s current state of women’s health and reproductive rights, as well as to be aware of the current practices that are still carried and enforced across the country.”—Woman
“My main takeaway is that I learned to highlight the importance of our history of healthcare in our country and recognize that I was unaware of a majority of the topics we covered today.”—Man
“Although I was familiar with a lot of the events discussed today, I learned quite a bit about historical events that I had not previously heard of. Additionally, I learned how recent historical events are affecting medical practice today and what they technically mean in a legal scope.”— Woman
“This session brought to light many acts of mistreatment and improper medical management that I was not aware of previously. It made me more deeply consider reproductive rights and health compared to what I thought previously.”—Man
Student attitudes about women’s reproductive justice were measured pre-and post-intervention by asking students to respond to a series of statements on the pre-post surveys and in the post-survey feedback and comments. Students’ overall ratings of the attitude statements were quite high on the preintervention survey, resulting in minimal change in the post-survey (Table 4). Interestingly, when asked to rate agreement with the statement: “Healthcare is a right”, women more strongly agreed on post-survey (pre 5.76 versus post 6.0, p<0.001), while men decreased their initial level of agreement with that statement (pre 5.44 versus 4.72, p<0.001). On the post-event survey, overall, students agreed with the statement: “this event impacted my attitude towards women’s rights” with an average Likert score of 4.60 (+/− 1.33); with no statistically significant differences found between genders (p=0.79). Similar trends were seen for the statement: “This event encouraged me to fight against the reproductive injustices seen for women”, with an overall rating of 4.92 (+/−1.17), (women 5.06 (+/−1.12), men 4.75 (+/−1.14); p=0.1). Finally, 15% of the free-text comments about the event suggested a desire to move beyond knowledge towards action, and included statements about their thoughts, feelings, or desires to impact the future. Examples of these statements can be found in the quotes below.
Table 4 Student Agreement with Attitude and Perception Statements
“I learned that the road to women’s reproductive rights and justice has only recently been uncovered and that it is our responsibility to be aware, protect, and fight for our female patients and their reproductive rights.”—Woman
“I enjoyed seeing the historical events of reproductive justice and relevant Supreme Court rulings placed in chronological order as I can better understand where and how reproductive freedoms still need to be advocated and fought for.”—Woman
“I thought learning about how these decisions are made was important because it could affect us all in the future. Not only on a societal level but on a personal level, being aware of the decisions made is important in how we will all practice medicine in the future.”—Man
It was beneficial to “[Understand] that this struggle still extends forward, and we play an important role in fighting this issue.”—Man
“I learned about specific cases impacting women’s rights and now feel much more capable of advocating for women’s rights.”—Woman
Overall, this study shows gender discrepancies in students’ perceptions about the impact of gender on medicine. In general, women tend to agree more strongly with the observation/experience of the effects of gender in medicine than men. Despite starting with different levels of experience and knowledge of gender in medicine, all students showed significant learning following the event. Additionally, students largely agreed that the event impacted their attitudes towards women’s rights. This suggests that despite starting from different places, both women and men saw improvements in knowledge and reported impacts on attitude following the event. From the students’ lived experiences, we were pleased to see that students in this study did not report having observed biases in the evaluation of student performance in medical school; however, it is important to note that students were in their second year foundational science courses, with minimal experience in the clinical setting. Most evaluations completed thus far in our curriculum consisted of summative examinations or clinical OSCEs with faculty who had more formal training in education, which may lead to more unbiased evaluations. The literature does not support the lack of gender bias in evaluations for more subjective assessments.27–32
In studies comparing medical student genders (women vs men), gender bias has been repeatedly identified. Women experience lower performance evaluations, fewer procedural opportunities, and fewer positive traits are identified in recommendation letters. Most of these evaluations are subjective and, therefore, are impacted by unconscious biases.27–30,33,34 Further, female physicians are more likely to experience a toxic work environment, by receiving greater criticism and disparaging comments and having their competence questioned by patients and colleagues compared to a lesser degree for male physicians.30 The limited numbers of female physicians in many medical specialties make it more challenging for female trainees to find a mentor compared to males.31 Together, this leads to diminished confidence and increased burnout rates.11,35 Women are often excluded from leadership positions and academic promotions, even among specialties engaging in diverse recruiting practices.35
Our study corroborates prior research, indicating that women are more prone to witnessing and encountering gender bias in the field of medicine compared to men.34,36 Dedicating a learning event solely to the topic of women’s rights can play a constructive role in addressing gender bias in medicine by creating a space for dialogue, a chance for both genders to explore systems of oppression, and developing solutions to the gender-related inequities seen in healthcare.
While there are specific strategies that have been implemented to try and overcome some of these limitations for women in medicine, including the use of specifically gender-neutral objective grading tools and rubrics, recommendation letter templates, faculty education about gender differences, and increasing the recruitment and representation of women in the faculty and leadership workforce, many interventions have shown limited impact, so additional solutions are still needed.29,37–39 This study was designed to increase students’ knowledge about gender disparities seen in healthcare using a critical theory pedagogy, to allow students to explore the social structures driving these problems and trigger changes in attitudes that subsequently can alter behaviors, reducing gender bias. We were able to highlight the impact that gender disparities have on health outcomes and expose students to the historical trauma experienced by marginalized groups within the healthcare system, which helps to explain patient mistrust of the healthcare system.
In this intervention we intentionally approached gender bias from the perspective of patient outcomes rather than focusing on gender bias in the medical workforce. This allowed us to use an emotional appeal technique, aimed to promote sympathy/compassion for women rather than pointing a finger at trainees to change their behavior.40,41 Increasing the sympathy of trainees towards female patients may also lead to changes in gender bias towards colleagues in the healthcare workforce. The focus on patient outcomes was also beneficial from the study design perspective, in that it helped avoid the impacts of the Hawthorne effect on student responses.42 If the event was designed to educate students about the gender disparities seen in the medical education and healthcare system, then student responses may have been skewed towards answers that they believed study investigators desired instead of their actual beliefs and perceptions about gender (the Hawthorne effect).11,30,34,35
Student knowledge and attitudes were impacted following our educational intervention for both genders. Interestingly, we saw gender bias in responses to the questions of whether healthcare is a privilege or a right, a topic that has long been debated in US culture, and which is a political topic.43 Based on our current healthcare landscape and outcomes, it could be argued that healthcare is a privilege; but should it be? Depending on an individual’s past experiences with healthcare, people often have strong personal beliefs about this issue that can even impact their own pursuit of health interventions.44,45 As such, it was surprising to see a change in students’ perception of this statement following our educational intervention. It is unclear why women more strongly supported the statement that healthcare is a right, while men disagreed more following the intervention. This may suggest that students interpreted this question in the post-survey in a different manner. We hypothesize that for women, this may be due to gender alignment with the content, leading to a firmer stance on the need for healthcare to be a right for women. In contrast, we hypothesize that men may have interpreted the event to suggest that healthcare is not always available or equitable for everyone; thus, it was viewed more as a privilege. Further studies are needed to understand this disparitiy in student responses.
This study was conducted at a single institution with two cohorts of students, which limits generalizability. Among the cohort there were only three individuals who indicated they identified as transgender or “other” which limits the conclusions which can be drawn about these populations. Additionally, whether this event has a lasting impact on students’ knowledge and core beliefs still needs to be determined; it is unlikely that a single event will be sufficient to change knowledge, attitudes, or behavior in a lasting way, necessitating further incorporation of gender-specific topics into the curriculum. Efforts to support increased sex and gender topics in the curriculum are currently being pursued by numerous organizations, including the Group on Women in Medicine and Science, the American Medical Women’s Association, and the Sex and Gender Health Education initiative, in addition to individual faculty.17,46–48
With the rapidly expanding medical knowledge that medical students need to learn and understand, it is essential that we don’t lose track of the vital components of our history that impact the way that medicine is practiced. Incorporating history, justice, and hot topics into medical education provides a framework for students to better understand their patients, which improves care outcomes. Similarly, it is essential to recognize that sex and gender both impact health. Helping students to identify and understand the differences that exist allows better outcomes for patients and providers alike.
Our study found a pre-existing gender bias in students’ perceptions and observations about gender in medicine, upon which an educational intervention can make an impact. Increases in student knowledge about sex and gender topics in medicine, and changes in attitudes towards women’s rights were observed immediately following the event. If a single educational intervention can have an immediate impact, imagine the impact of fully incorporating these topics into medical curricula. Further, teaching our students to identify oppressive structures so they can advocate for solutions to the problems they witness in medicine helps create a better future for everyone.
1. UN Women. Progress on the Sustainable Development Goals: The Gender Snapshot 2025. Published online 2025. Available from: https://www.unwomen.org/en/digital-library/publications/2025/09/progress-on-the-sustainable-development-goals-the-gender-snapshot-2025
2. Evans ML, McGregor AJ. Improving the health of women across the life span: recognizing biological barriers and beyond. Clinical Therapeutics. 2020;42(3):382–384. https://doi.org/10.1016/j.clinthera.2020.02.004
Crossref PubMed
3. Prescott H, Thompson L. A right to ourselves: women’s suffrage and the birth control movement. The Journal of the Gilded Age and Progressive Era. 2020;19(4):542–558. https://doi.org/10.1017/S1537781420000304
Crossref
4. Waltz M, Lyerly A, Fisher J. Exclusion of women from phase 1 trials: perspectives from investigators and research Oversight Officials. Ethics Human Research. 2023;45(6):19–30. https://doi.org/10.1002/eahr.500170
Crossref
5. Samaei M, Jenkins MR, McGregor AJ. Closing the gap: How women can benefit more from science, research, policies, and health services. Med. 2022;3(5):302–308. https://doi.org/10.1016/j.medj.2022.04.012
Crossref PubMed
6. Evans ML, McGregor AJ. Improving the health of women across the life span: recognizing biological barriers and beyond. Clinical Therapeutics. 2020;42(3):382–384. https://doi.org/10.1016/j.clinthera.2020.02.004
Crossref PubMed
7. Hay K, McDougal L, Percival V, et al. Disrupting gender norms in health systems: making the case for change. The Lancet. 2019;393(10190):2535–2549. https://doi.org/10.1016/S0140-6736(19)30648-8
Crossref
8. ALobaid AM, Gosling C, Khasawneh E, McKenna L, Williams B. Challenges faced by female healthcare professionals in the workforce: a scoping review. JMDH. 2020; Volume 13:681–691. https://doi.org/10.2147/JMDH.S254922
Crossref
9. Lautenberger D, Dandar V. The state of women in academic medicine 2023–2024: Progressing Equity. Published online November 2024. Available at: https://www.aamc.org/data-reports/data/state-women-academic-medicine-2023-2024-progressing-toward-equity
10. OECD. Health at a Glance 2023: OECD Indicators. OECD; 2023. https://doi.org/10.1787/7a7afb35-en
11. Dossa F, Baxter N. Reducing gender bias in surgery. British Journal of Surgery. 2018;105(13):1707–1709. https://doi.org/10.1002/bjs.11042
Crossref PubMed
12. Tsugawa Y, Jena AB, Figueroa JF, Orav EJ, Blumenthal DM, Jha AK. Comparison of hospital mortality and readmission rates for Medicare patients treated by male vs female physicians. JAMA Internal Medicine. 2017;177(2):206. https://doi.org/10.1001/jamainternmed.2016.7875
Crossref PMC
13. Zhao C, Dowzicky P, Colbert L, Roberts S, Kelz RR. Race, gender, and language concordance in the care of surgical patients: A systematic review. Surgery. 2019;166(5):785–792. https://doi.org/10.1016/j.surg.2019.06.012
Crossref PubMed
14. Bertakis KD, Azari R. Patient-Centered Care: The influence of patient and resident physician gender and gender concordance in primary care. Journal of Women’s Health. 2012;21(3):326–333. https://doi.org/10.1089/jwh.2011.2903
Crossref
15. Greenwood BN, Carnahan S, Huang L. Patient–physician gender concordance and increased mortality among female heart attack patients. Proceedings of the National Academy of Science USA. 2018;115(34):8569–8574. https://doi.org/10.1073/pnas.1800097115
Crossref
16. Verdonk P, Benschop YWM, De Haes HCJM, Lagro-Janssen TLM. From gender bias to gender awareness in medical education. Advances in Health Science Education. 2009;14(1):135–152. https://doi.org/10.1007/s10459-008-9100-z
Crossref
17. Rojek MK, Jenkins MR. Improving medical education using a sex- and gender-based medicine lens. Journal of Women’s Health. 2016;25(10):985–989. https://doi.org/10.1089/jwh.2016.5948
Crossref
18. Miller VM, Flynn PM, Lindor KD. Evaluating sex and gender competencies in the medical curriculum: A case study. Gender Medicine. 2012;9(3):180–186.e3. https://doi.org/10.1016/j.genm.2012.01.006
Crossref PubMed
19. Paul CR, Chheda S, Beck Dallaghan G, et al. Gender bias in patient care learning experiences: reflective writings of third-year medical students. Medical Science Educator. Published online December 13, 2024. https://doi.org/10.1007/s40670-024-02216-4
20. Hui K, Sukhera J, Taylor V, Zaheer J. Recognizing and addressing implicit gender bias in medicine. Canadian Medical Association Journal. 2020;192(42):e1269–e1270. https://doi.org/10.1503/cmaj.200286
Crossref PubMed PMC
21. Wortmann L, Haarmann L, Yeboah A, Kalbe E. Gender medicine teaching increases medical students’ gender awareness: results of a quantitative survey. GMS Journal for Medical Education. 2023;40(4):1–17. https://doi.org/10.3205/zma001627
22. Kling JM, Rose SH, Kransdorf LN, Viggiano TR, Miller VM. Evaluation of sex- and gender-based medicine training in post-graduate medical education: a cross-sectional survey study. Biology of Sex Differences. 2016;7(S1):38. https://doi.org/10.1186/s13293-016-0097-3
Crossref PubMed PMC
23. DasGupta S, Fornari A, Geer K, et al. Medical education for social justice: Paulo Freire revisited. Journal of Medical Humanities. 2006;27(4):245–251. https://doi.org/10.1007/s10912-006-9021-x
Crossref PubMed
24. Van Wyk N. Health education as education of the oppressed. curationis. 1999;22(4):29–34. https://doi.org/10.4102/curationis.v22i4.748
Crossref
25. Cochon Drouet O, Lentillon-Kaestner V, Margas N. Effects of the Jigsaw method on student educational outcomes: systematic review and meta-analyses. Frontiers in Psychology. 2023;14:1216437. https://doi.org/10.3389/fpsyg.2023.1216437
Crossref PubMed PMC
26. Parker RB, Parker PD, Larkin T, Cockburn J. A psychometric evaluation of the Gender Bias in Medical Education Scale. BMC Medical Education. 2016;16(1):251. https://doi.org/10.1186/s12909-016-0774-2
Crossref PubMed PMC
27. Klein R, Julian KA, Snyder ED, et al. Gender bias in resident assessment in graduate medical education: Review of the literature. Journal of General Internal Medicine 2019;34(5):712–719. https://doi.org/10.1007/s11606-019-04884-0
Crossref PubMed PMC
28. Khan S, Kirubarajan A, Shamsheri T, Clayton A, Mehta G. Gender bias in reference letters for residency and academic medicine: a systematic review. Postgraduate Medical Journal. 2023;99(1170):272–278. https://doi.org/10.1136/postgradmedj-2021-140045
Crossref PubMed
29. Murphy M, Record H, Callander JK, Dohan D, Grandis JR. Mentoring relationships and gender inequities in academic medicine: findings from a multi-institutional qualitative study. Academic Medicine. 2022;97(1):136–142. https://doi.org/10.1097/ACM.0000000000004388
Crossref
30. Marchetti KA, Ferreri CA, Bethel EC, et al. Gender-based disparity exists in the surgical experience of female and male urology residents. Urology. Published online February 2024:S0090429524000086. https://doi.org/10.1016/j.urology.2023.11.035
31. Burke E, Heron EA, Hennessy M. Gender bias in academic medicine: a resumé study. BMC Medical Education. 2023;23(1):291. https://doi.org/10.1186/s12909-023-04192-6
Crossref
32. Fjørtoft K, Konge L, Christensen J, Thinggard E. Overcoming gender bias in assessment of surgical skills. Journal of Surgical Education. 2022;79(3):753–760. https://doi.org/10.1016/j.jsurg.2022.01.006
Crossref PubMed
33. Dossa F, Baxter NN. Reducing gender bias in surgery. British Journal of Surgery. 2018;105(13):1707–1709. https://doi.org/10.1002/bjs.11042
Crossref PubMed
34. Yaman R, Hagen KM, Ghaith S, Luong H, Almader-Douglas D, Langley NR. Gender bias in medical education: A scoping review. The Clinical Teacher. 2023;20(4):e13592. https://doi.org/10.1111/tct.13592
Crossref PubMed
35. Bosco L, Lorello GR, Flexman AM, Hastie MJ. Women in anaesthesia: a scoping review. British Journal of Anaesthesia. 2020;124(3):e134–e147. https://doi.org/10.1016/j.bja.2019.12.021
Crossref PubMed
36. Brown MEL, Hunt GEG, Hughes F, Finn GM. ‘Too male, too pale, too stale’: a qualitative exploration of student experiences of gender bias within medical education. BMJ Open. 2020;10(8):e039092. https://doi.org/10.1136/bmjopen-2020-039092
Crossref PubMed PMC
37. Fjørtoft K, Konge L, Christensen J, Thinggard E. Overcoming gender bias in assessment of surgical skills. Journal of Surgical Education. 2022;79(3):753–760. https://doi.org/10.1016/j.jsurg.2022.01.006
Crossref PubMed
38. Ryan JF, Istl AC, Luhoway JA, et al. Gender disparities in medical student surgical skills education. Journal of Surgical Education. 2021;78(3):850–857. https://doi.org/10.1016/j.jsurg.2020.09.013
Crossref
39. Reghunathan M, Carbullido MK, Blum J, Wong S, Gosman AA. Standardized letters of recommendation in plastic surgery: The impact of gender and race. Plastic Reconstructive Surgery. 2022;149(5):1022e–1031e. https://doi.org/10.1097/PRS.0000000000008991
Crossref PubMed
40. Shiota MN, Vornlocher C, Jia L. Emotional mechanisms of behavior change: Existing techniques, best practices, and a new approach. Policy Insights from the Behavioral and Brain Sciences. 2023;10(2):201–211. https://doi.org/10.1177/23727322231195907
Crossref
41. Fox S, Amichai-Hamburger Y. The power of emotional appeals in promoting organizational change programs. Academy of Management Perspectives. 2001;15(4):84–94. https://doi.org/10.5465/ame.2001.5897664
Crossref
42. Sedgwick P, Greenwood N. Understanding the Hawthorne effect. British Medical Journal. 2015;351: h4672. https://doi.org/10.1136/bmj.h4672
Crossref PubMed
43. Bauchner H, Fontanarosa PB. Health care is a right and not a privilege. JAMA. 2020;323(11):1049. https://doi.org/10.1001/jama.2020.0891
Crossref PubMed
44. Toth-Manikowski SM, Swirsky ES, Gandhi R, Piscitello G. COVID-19 vaccination hesitancy among health care workers, communication, and policy-making. American Journal of Infection Control. 2022;50(1):20–25. https://doi.org/10.1016/j.ajic.2021.10.004
Crossref
45. Elliott TR, Perrin PB, Powers MB, Jacobi KS, Warren AM. Predictors of vaccine hesitancy among health care workers during the COVID-19 Pandemic. International Journal of Environmental Research and Public Health. 2022;19(12):7123. https://doi.org/10.3390/ijerph19127123
Crossref PubMed PMC
46. American Medical Women’s Association. Sex and gender health collaborative. Accessed February 5, 2025. Available from: https://www.amwa-doc.org/sghc/
47. Barr E, Chin EL, Newman CB, et al. Reflecting on progress in and establishing benchmarks for sex and gender health education. Academic Medicine. 2024;99(1):16–21. https://doi.org/10.1097/ACM.0000000000005444
Crossref
48. Chin EL, Hoggatt M, McGregor AJ, et al. Sex and Gender Medical Education Summit: a roadmap for curricular innovation. Biology of Sex Differences. 2016;7(S1):52. https://doi.org/10.1186/s13293-016-0091-9
Crossref PubMed PMC
© Education for Health.
Education for Health | Volume 38, No. 4, October-December 2025